This article was initially printed in PRIORITIES, our quarterly periodical.
By Jack Raso
ACSH Scientific Advisor Emil W. Chynn, M.D., a native Manhattanite who lives on Sixth Avenue in Greenwich Village, seems a very busy Renaissance man. He is, for example, a sportsman, a part-time M.B.A. student, a writer, a researcher, an inventor, and a private practitioner of laser surgery for vision correction 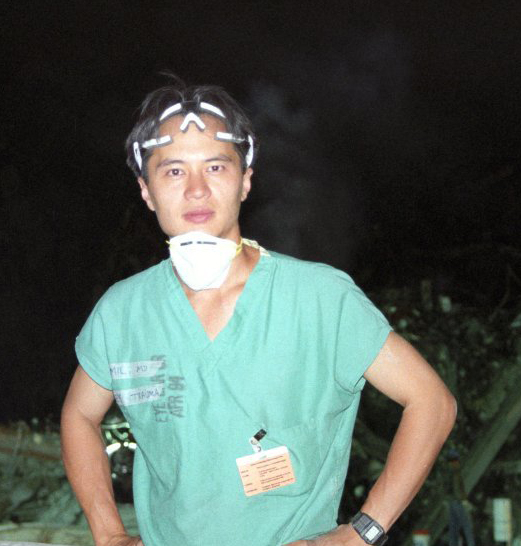 (ParkAvenueLasek). On the day of the in-flight attack on the World Trade Center, this ophthalmologist headed purposefully and unselfishly toward “ground zero”—unbidden, unaccompanied, unguided, and ill-equipped. He volunteered there daily for six consecutive days.
(ParkAvenueLasek). On the day of the in-flight attack on the World Trade Center, this ophthalmologist headed purposefully and unselfishly toward “ground zero”—unbidden, unaccompanied, unguided, and ill-equipped. He volunteered there daily for six consecutive days.
During the first half of October, I asked questions of Dr. Chynn by email and by phone concerning this experience. His account follows.
"On Tuesday, shortly after 9:00 A.M., a friend of mine called me as I was about to leave for work. She told me that a plane had hit the World Trade Center. I went to the street with my neighbors and saw the twin towers on fire. Sixth Avenue in Greenwich Village was filled with pedestrians; no cars were moving. It seemed a tragic variation of a scene from Times Square on V-E Day.
I called the downtown hospitals I’m affiliated with—New York Eye and Ear Infirmary (where I’m an eye trauma surgeon) and St. Vincent’s (which is one of the two downtown hospitals designated as a major trauma center)—to let them know that I was available for emergency duty. Both hospitals advised me to “stand by,” as they hadn’t received any victims. From my experience as an intern on call the day the World Trade Center was bombed, in 1993, I knew that significant time could elapse between the primary incident and the first arrival of victims in the ER. So, I decided to go to the site unofficially and see if I could provide any immediate help.
I returned to my apartment to gather ophthalmic paraphernalia: (a) 30 eye kits
Bausch & Lomb had provided for my LASIK practice, each consisting of “eye shields,” goggles, tape, antibiotic drops, and artificial tears; and (b) other ophthalmic paraphernalia, including saline solution and the eye surgical kit I had first used during study in India as a resident with the Massachusetts Eye and Ear Infirmary.
Physicians, nurses, and EMTs seeking to volunteer at the WTC site went there separately from one another but met en route, informally. I was one of the first doctors at the scene; the group I was in arrived around 11:00 A.M. The chaos was total, with fire engines burning, cars exploding, debris falling, and a thick blanket of ash and paper over everything in sight.
My group—initially of about 12 healthcare workers—included an anesthesiologist, a trauma resident, and a few nurses. None of us had hardhats, thick gloves, walkie-talkies, or masks capable of preventing inhalation of the particles of concrete in the air.
There was no triage center at the site. So we decided that our first need was to set up one. Ambulance crews waited as others and I walked toward the area of densest smoke. We first considered as a possible triage site the remains of a firehouse. I re-jected this place because what was left of the station appeared shaky, lacked electrical power, and was riddled with debris. I spotted a Burger King restaurant that looked relatively intact. It was at One Liberty Plaza, across the street from the firehouse site.
There, we were moving a bunch of apple pies to make space for our IVs when we discovered our lack of crucial items: catheters, basic surgical instruments, and ACLS (advanced cardiac life support) supplies. If any victims were brought to us in critical condition, there would be real trouble. One doctor cried in frustration, beating his head on a wall.
Around 1:00 P.M., the dense smoke suddenly thinned, and we saw vestiges of 2 World Trade Center directly for the first time. We came to a standstill, realizing that very few victims of the attack would become available for treatment.
Later that afternoon, a podiatrist was asked to perform an amputation to free a victim from rubble. The podiatrist refused on grounds that the surroundings were unstable. Eventually the victim was freed without amputation. This style of decision making was characteristic among physicians volunteering at the site; each doctor was deciding on the fly and without any official guidelines. We treated only two victims the day of the attack, and only three the following day—by the end of which my group consisted of 20 to 30 healthcare workers.
Outside a hospital hierarchy, healthcare workers from different facilities lack a chain of command. For the first three days of the crisis, no one was officially coordinating medical care at the site. In default of such coordination, my companions and I took turns in leading our group. For the first couple of days, every hour a fire department commander or police chief would approach us and ask: “Who’s in charge?” We would accede to whoever of us seemed the least tired. Occasionally, even a medical student took charge.
On Wednesday afternoon, a firefighter burst into our triage center and yelled that everyone must evacuate the building, which apparently was buckling. All of us ran out. By Thursday, my group consisted of 40 to 50 healthcare workers. That night, we set up a replacement triage center near the Millennium Hilton Hotel, about a block away from One Liberty Plaza.
By Friday, September 14, well equipped members of Emergency Disaster Medical Services (EDMS) arrived at our triage center to take it over. We were relieved at this. In a disaster area such as the World Trade Center site, coordination problems are almost inevitable. But in such circumstances any medical team needs organization, and resources, equivalent to those of the firefighters and police officers at the scene.
I treated no life-threatening injuries at the site. Most of those we treated in the six days I volunteered at the site were rescue workers. Mostly, I treated abraded corneas and eyes affected by foreign bodies. I had expected that I would treat more lacerated corneas and ruptured eyeballs than I treated. If hundreds of victims of the attack had survived its aftermath, probably many of them would have died during triage for lack of both preparation and equipment."
Dr. Chynn was interviewed at the World Trade Center site on national television. Afterwards, he coordinated some of the donation efforts of ophthalmic companies and began to drum up charitable contributions through his LASIK practice.
It is not reasonably deniable that unorganized medical volunteers aren’t likely to meet the medical needs of an emergency of the magnitude of what prompted the exodus from the World Trade Center site and its environs. Advises Dr. Chynn: “Each American city should found, fund, and staff a local emergency medical response team similar to that of EDMS, which is federal. Doctors, nurses, and EMTs would be on call throughout each day to establish triage and to coordinate ongoing medical services.”
More images can be found here
Image courtesy of Emil W. Chynn, MD