Lead in drinking water became a political and media cause celebre in 2014 when there were reports of child “lead poisoning” in Flint, Michigan, after the notorious and unfortunate water supply blunders. The Flint problem could easily have been avoided with some common sense and legally required water management procedures.
Lead avoidance is good, but the facts are that US population lead exposure has been significantly reduced beginning with banning lead paint and in the 1980s when EPA mandated catalytic converters in motor vehicles, essentially eliminating leaded gasoline. The 1976-1980 National Health and Nutrition Examination Survey (NHANES II) found that national geometric mean blood lead levels in children were more than 15 µg/deciliter (micrograms per 100 cc). Today, the median levels are on the order of 0.5 µg/dL, more than 95% reduction and still declining. Lead reduction in the US environment and most drinking water is a national success story, and the EPA should be applauded for the leaded gasoline elimination.
There are still some children with very high blood lead levels. The CDC believes this is primarily due to old lead paint and dust in homes that have not been mitigated. Lead paint was banned for residential use in 1978.
The real story about Flint
Due to the high cost of buying treated water from Detroit, Flint’s municipal government decided to switch back to their old water plant on the Flint River while they planned to construct a new pipeline from Lake Huron. They did not do the required standard testing to determine whether treatment modifications were necessary. Flint River water is much more corrosive than Lake Huron water which Detroit used, but Flint made no adjustments to control these corrosive effects. The influx of new corrosive water released and suspended accumulated sludge deposits from the old distribution pipes resulting in discolored low-quality water containing bacteria and lead. The water was so obviously contaminated and unpalatable that most people avoided drinking it.
The media and politicians had no understanding of the reality and correctability of the problem - declaring children were being brain-damaged. It became a national issue partly because two presidential candidates (Clinton and Sanders) arrived to make political hay out of the situation. Actually, there was no brain damage, as shown by the thousands of blood lead measurements conducted in Flint. Dr. Hernan Gomez is a physician and epidemiologist in Flint who has tracked lead reduction in Flint children for years. The Figure represents about 16,000 blood lead measurements, illustrating the true extent and history of lead in pediatric blood levels in Flint.
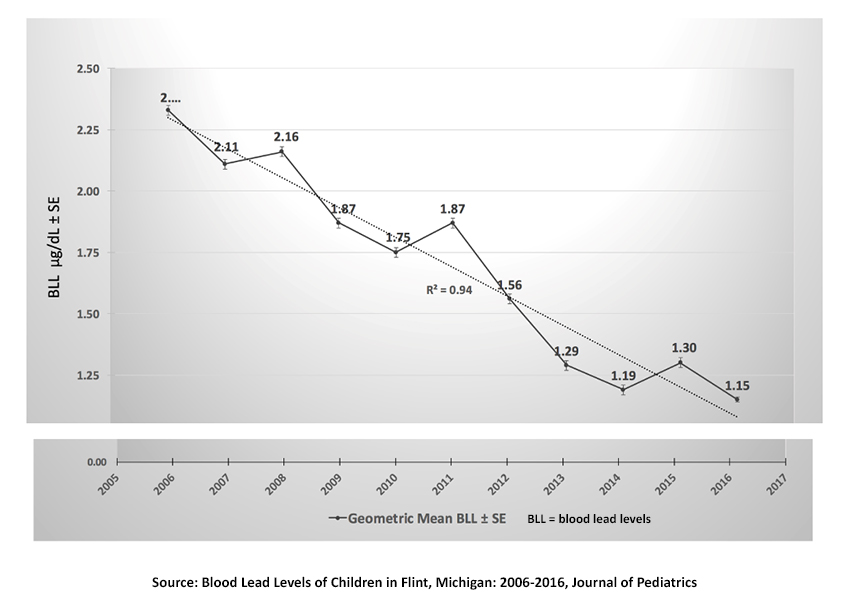
- The half-life of lead in blood is about 30 days.
- Between 2014-2016, the period during the water problem, lead levels showed a slight increase in 2015 and then a decline in 2016.
- The CDC examined more than 9000 child blood lead samples in the period and found that about 2% (59 to 71) temporarily rose from below five µg/dL (the then-current CDC 97.5th percentile reference level). Still, there was no increase and, in fact, a slight decline for those above ten µg/dL. So, it never approached the 1976-1980 national levels.
- The likely health outcome was 88 cases of legionellosis and 12 deaths that could have been associated with inhaling aerosols from showering with the contaminated water. Neither received much press or political concern.
There was a flurry of misdirected consequences. Congress allocated $100 million to replace all lead service lines in Flint; the EPA revised its 1991 Lead and Copper regulations - regulations that had not been fully implemented or enforced by the States in the 30 years since its promulgation. [1]
Experience shows that excellent corrosion control is achievable in almost all water supplies and produces other water quality benefits. Several potential sources of lead leaching into drinking water include brass faucets, old galvanized iron pipe residues, and old lead solder, which was banned in the 1980s. Replacing lead service lines does not affect those sources. Indiscriminate lead service line replacement is slow (years), expensive (~$10,000 each), and not entirely effective. Corrosion control is rapid, comprehensive, and inexpensive.
The fallout from Flint resulted in much misinformation, politically driven wasteful spending, misplaced public fears, and skewed priorities from the real needs of water suppliers. The blood data show that we do not have a lead emergency. The US is among the first countries to successfully provide significant reductions in lead exposures from all sources, beginning over 40 years ago. It is probably impossible to achieve zero blood lead because of trace levels in foods, but we are pretty close.
The more critical drinking water priorities include maintaining and replacing old infrastructure and legionellosis prevention. Legionella pneumophila, a bacteria associated with Legionnaire’s Disease, can regrow in water. Today, legionellosis is the only known cause of waterborne disease deaths in the US, caused by inhalation of water aerosols (not drinking). About 60 % of reported waterborne disease outbreaks are for legionellosis and all of the deaths. The EPA has not taken any serious steps to reduce those real risks. So, let’s get our drinking water protection priorities straight.
Lead reduction in the US is a national success story.
[1] The 1991 Lead and Copper regulation required corrosion control based on a worst-case screening test using stagnant (overnight) first-drawn water from the most likely taps in the community. Excess levels require community-wide corrosion control, which, if unsuccessful in reducing levels of lead, requires a schedule for the replacement of lead service lines
Source: Blood Lead Levels of Children in Flint, Michigan: 2006-2016 Journal of Pediatrics DOI: 10.1016/j.jpeds.2017.12.063
