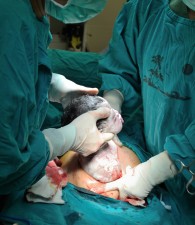
Cesarean Delivery via Shutterstock
In roughly 50 years, births by cesarean section in the United States have increased seven fold, from 4.5 percent in 1965 to 32.2 percent of all deliveries in 2014. What's more, the rise appears to be a global trend, and the procedure is the topic of an interesting report in the December 1st issue of JAMA.
In the study by US researchers across three universities, data from 2005 to 2012 was collected for all 194 World Health Organization member states. For 2012, the global number of cesarean deliveries was estimated at 22.9 million, yielding a global cesarean delivery rate of 19.4 per 100 live births, or 19.4 percent.
Analysis indicated that the "necessary" cesarean delivery rate in relation to maternal and neonatal mortality -- where the procedure was needed, not optional -- was approximately 19 cesarean deliveries per 100 live births.
Back in 1985, recognizing the growing issue, the WHO issued recommendations for an optimal cesarean delivery rate of 10-15 percent. However, an optimal cesarean rate is an unrealistic expectation to apply across all countries, given the disparity in health care access, resources, societal and cultural norms and values.
Twenty five years later, in an updated statement in 2010 WHO back-pedalled from its initial blanket statement, commenting: "... that as countries increase their caesarean section rates up to 10 percent, maternal and neonatal mortality decrease. However, caesarean section rates higher than 10 percent are not associated with reductions in maternal and newborn mortality rates."
Based on their findings, the study's authors today suggest that national target rates for C-sections may be too low. Yet looking at the limitations of the study, a recommendation of such seems premature. The data was obtained from several different sources. Additionally 22 countries did not have cesarean delivery data, and their rates were estimated using regression models, which were also used to estimate cesarean delivery rates for 113 countries which did not have rates for 2012.
Moreover, a study of this caliber, looking at populations, cannot allow for a causal relationship to be adopted. This study has merely shown an association between increasing cesarean delivery rates and decreasing mortality.
But what about the factors at play behind the scenes? There is much disparity between the provision of antenatal, intrapartum and peripartum health care. Lack of timely antenatal care interventions, hospital resources and skilled health personnel are all factors that may alter the statistics on a country-by-country basis, all of which have been unaccounted for.
Furthermore, varying definitions in what may be considered a necessary case requiring a cesarean delivery can be a confounder.
For example, in some cases of breech delivery, where the fetus presents with the feet first, a trial of vaginal delivery is acceptable, provided the obstetrician is competent in the techniques needed for a successful vaginal delivery of a breech presentation. With litigation issues and malpractice insurance both on the rise, the opportunity for these valuable techniques to be passed on to oncoming obstetricians is being thwarted by defensive medicine.
While the statistics of this study tell an important story, the real question that remains to be answered is despite the health risks, why are cesarean delivery rates rising so dramatically? Excluding emergency cases and unforeseen complications -- which pose a serious threat to maternal and/or fetal demise -- why are women now opting to have planned cesarean deliveries versus vaginal deliveries? Have they forgotten that a C-section -- even a planned, elective one -- is still a surgery, and should not be approached in a casual manner?
Each surgical procedure comes with it risks which include, but not limited to, hemorrhage, infection, and unintentional damage to surrounding tissues and organs. In the case of cesarean sections, mother and fetus are both at risk for harm during delivery. And all of this risk is for what gain? To have a Christmas Day baby? To avoid the pain of childbirth?
And clinicians are not exempt from blame. A bit of good clinical sense, common sense and a backbone can serve to sway persistent mothers from requesting the procedure. Part of a clinician's job is to educate their patients. They should let it be known that if things go wrong the mother could, for example, end up incontinent, without an uterus, or even dead.
Even the most experienced obstetrician can make a mistake. In that light, a cesarean section should not be a want, but instead a necessity, offered on a case-by-case basis when the medical situation warrants it.


