I recently returned from spending two weeks on a college campus in upstate New York. While there, I was surprised to see, in every building that I entered, signs posted with health information about mumps. Mumps... the same viral infection that was predicted to be eliminated from the United States by 2010.
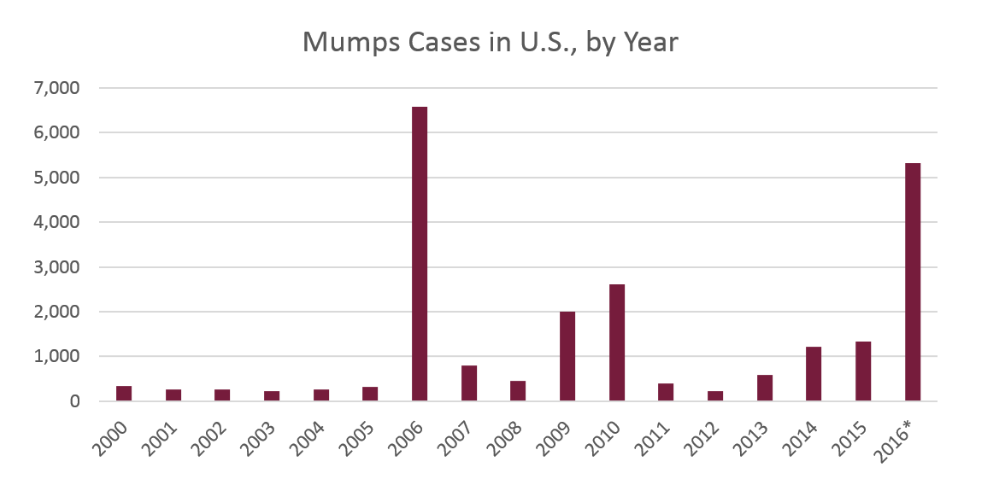
Before the mumps vaccine was available in 1967, there were an estimated 150,000 - 200,000 cases reported each year. Since then, the number of cases of mumps has decreased by 99% in the United States. That being said, there remains a lot of fluctuation from year to year, easily seen in the graph below. To this point, there is an outbreak of mumps currently in Washington state, with nearly 300 cases reported - a large number compared to the normal ebb and flow of mumps from year to year.
The mumps vaccine is the lesser known cousin included in the 'MMR' vaccine (the other two infectious diseases in there are measles and rubella.) When both doses of the mumps vaccine are administered, it is roughly 88% effective. Although this level of protection could be higher, if someone told you that you had an 88% chance of winning the lottery, you would probably buy the ticket.
Mumps can be easily recognized by puffy cheeks and a swollen jaw caused by swollen salivary glands. Common symptoms are fever, headache, muscle aches, fatigue and loss of appetite. Symptoms typically appear 16-18 days after infection, and most people recover in a few weeks.
For the most part, outbreaks occur in areas where there are a lot of individuals living in close contact such as schools, camps, dormitories, etc. Although the reason for the large number of mumps cases in 2016 and recent outbreaks is not clear, there are a few theories circulating.
A commentary from the Journal of Infectious Diseases highlights a few possible factors, including
- Fluctuations in the efficacy of the vaccine
- Increasing population density in communal living situations
- Individual immunity waning over time, raising the possibility of a third booster later in life
- The vaccine strain (derived from strain type A) may be less effective against the types of strains circulating today (type G strains)
- The level of protection needed to prevent outbreaks may need to be higher than the previously suggested.
Before the vaccine was widely distributed, ∼90% of all children had a mumps infection early on in life. Those people are the most protected amongst our population, having acquired immunity through an actual infection. However, these people are now older, leaving a large subset of the population (everyone under 50) to rely solely on vaccine-mediated immunity. And, although the vaccine is good, the predicted amount of immunized people to stop an outbreak is 92% - a tall order for any vaccine.
If everyone received the vaccine, this level of protection is obtainable. However, the growing anti-vaccine movement, which is especially critical of the MMR vaccine due to the false link created between it and autism, may create just enough of a dip to give a virus like mumps a chance to enter into the population and wreak havoc again.
References:
1. ://www.cdc.gov/mumps/outbreaks.html
2. Kutty PK, Kruszon-Moran DM, Dayan GH, et al. Seroprevalence of antibody to mumps virus in the US population, 1999–2004, J Infect Dis, 2010, vol. 2025(pg. 667-674)



