The HPV vaccine has been the subject of some controversy in the United States. Some public health officials (and pharmaceutical companies) would like the vaccine to be mandatory, but since the recommended age is pre-teen, some parents fear this sends a bad message about sexual activity in an already over-sexualized culture.
Both sides make flawed arguments. The bottom line is the vaccine prevents cancer.
Human papillomavirus is definitely a scourge. It causes 99% of cervical cancers in women, and it is also behind an increase in head and neck cancers, mostly in younger white people (i.e., those in their 40s and 50s). While this is certainly a public health concern, HPV poses nothing like the risk that measles, diphtheria, or whooping cough do. And the vast majority of people who become infected with HPV, even the high-risk strains, do not go on to develop cancer.
Similarly, parents who claim that an HPV vaccine is the key to a life of carnal pleasures are over-reacting. There are plenty of excellent reasons to avoid having sex while young, pregnancy and antibiotic-resistant gonorrhea being among them.
Regardless of where one falls on this debate, new research from Australia shows good news: Men who are unvaccinated for HPV are receiving protective benefits from the women who are vaccinated. In other words, this is a prime example of herd immunity in action.
Australia's HPV Vaccination Program
Beginning in 2007, Australia began a free HPV vaccination program, first aimed at females aged 12 to 26. Eventually, in 2013, boys were included. (The vaccine protected against HPV-16 and HPV-18, both "high-risk" strains that cause cancer, as well as HPV-6 and HPV-11 which cause genital warts.) Researchers wanted to determine if those who remained unvaccinated were receiving indirect protection.
The team studied 511 heterosexual males aged 16 to 35 who were unvaccinated for HPV and had sex with at least one woman. Penile swab samples were collected and analyzed for HPV DNA. They found that the younger men (aged 25 and below) were less likely than older men (aged 26 to 35) to be infected with the HPV strains targeted by the vaccine.
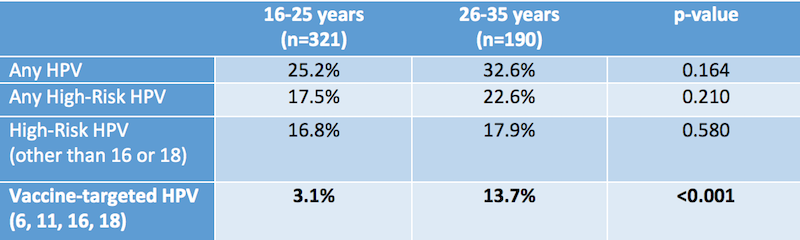
As shown, the difference in prevalence of vaccine-targeted HPV strains between younger men (3.1%) and older men (13.7%) was large and statistically significant. The reason, the authors suspect, is because young women (who tend to have sex with similarly aged men) have a higher HPV vaccine rate than older women (who tend to have sex with similarly aged men).
One could argue that the reason younger men have a lower prevalence of HPV is because they haven't yet had enough sexual encounters to become infected. True, the younger men had fewer lifetime sexual partners than the older men. But other data show they were still being exposed to HPV since the prevalence of HPV strains not targeted by the vaccine was roughly the same in both the younger and older men. (See the top three rows in the chart.) That strongly indicates that the vaccine is providing herd immunity against the strains it targets.
Perhaps Australia's success will influence other countries to implement a similar program.
Source: Dorothy A. Machalek et al. "Human Papillomavirus Prevalence in Unvaccinated Heterosexual Men After a National Female Vaccination Program." J Infect Dis (2017) 215 (2): 202-208. Published: 03 November 2016. DOI: 10.1093/infdis/jiw530