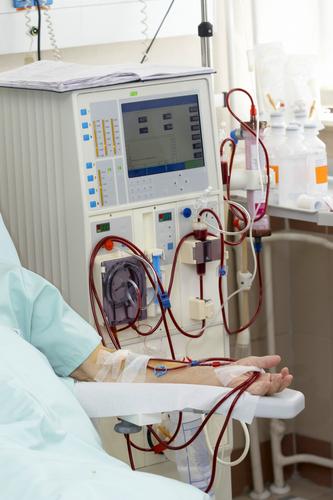
Setting the scene
In 1960 Clyde Shields, a mechanic at Boeing was told he had renal failure – a death sentence. But Dr. Belding Scribner started him on an experimental technique, dialysis, which extended Clyde’s life for another eleven years and made him patient zero in a revolution in health care.
By 1962, the first dialysis center had opened in Seattle and the care of patients with what we now call end-stage renal disease (ESRD) evolved. It was expensive, and so in 1972 the first legislative experiment with “socialized medicine” care provided care for all patients with ESRD through Medicare.
Today Medicare spends more than $10 billion on dialysis, medications and laboratory testing for some 370,000 patients.
90% of patients undergo hemodialysis, in one of 5800 freestanding centers, and have their blood filtered by a machine three times a week to remove the impurities that their kidneys can no longer remove. It is an outpatient service, Medicare Part B, so patients are required to make a 20% copayment for their treatment. CMS pays $230.39 per treatment – multiplied by the cost of the year the patient co-payment is about $7200, and this does not include the cost of their medications. For many patients, the cost to stay alive is substantial.
Playa 1 – The American Kidney Foundation (AKF)
Founded in 1971, it has attempted to help with the financial hardships of ESRD care. They created a program Health Insurance Premium Program (HIPP) to provide insurance premium payments so that patients could afford care. The problem is that this AKF program is funded by the second player – the for-profit dialysis networks, and the money earmarked for the HIPP program. The monies donated by the dialysis companies returns to them through Medicare, Medicaid, and private insurers who by for treatments, creating a conflict of interest. To be fair, the AKF recognized a conflict and attempted to create a firewall of sorts. First, they got the approval of the Office of the Inspector General for Health and Human Services that such an arrangement was not a “kickback.” More importantly, patients are required to choose their insurance program; the AKF does not make the choice.
“You must carefully review all forms of health insurance coverage (Medicare, Medicaid, Medigap, COBRA, EGHP, and commercial insurance) and available assistance for paying health insurance premiums (Medicaid, state and local assistance, charitable organizations) and select the combination that best serves your specific financial needs and medical condition.”
But to understand the conflict, we must as we learned from Watergate, ‘follow the money.”
Playa 3 – The American Renal Association
Fresenius Medical Care and DaVita are for-profit companies operating more than 70% of the freestanding dialysis centers and have combined operating profits of $2 billion. In 2010, they provided the AKF with 80% of its budget, $174 million. The American Renal Association (ARA) is a smaller player with about 3.5% of the market. When you go to their website, you get their approach right away from their tagline, “The Nephrologist is the Center of Our Universe.” No pretending here about being patient-centric. Using techniques developed by Fresenius and DaVita as early as 2011, these folks have found a way to game the well-intended work of the AKF - running the “coupon” shell game of the pharmaceutical industry with AKF’s HIPP program.
While Medicare pays $230 per treatment, private insurers pay more, lots more.
Typically two to four times as much. Maintaining a dialysis patient with a private insurance increases the income to the “center of our universe” – the ARA’s nephrologists. The selection of insurance carriers for dialysis patients is confusing and complex. The nephrologist and his staff already have a trusting relationship with patients. Who is better able to advise the patient in which direction to take? The AKF explicitly does not get involved, and into the vacuum of advice jumps the patient’s nephrologist, the American Renal Association. They have done the pharmaceutical industry one better; they have co-opted the “charitable” largesse of the dialysis market’s big players, Fresenius and DaVita and use the AKF as their unwitting conduit.
United Healthcare is suing the ARA over this behavior trying to recoup millions of dollars. Again we see a struggle between providers and insurers over who keeps the profits - who gets to keep our money.



