It is a requirement of the State of New York that every prescriber of medications takes a 3-hour course on opioid prescription and patient management. Despite the fact that, at several times during the 3 hours of video I felt that an opioid would be helpful, I found several concepts worth sharing. After all, the media continually is beating the drum about the opioid crisis. But what measures are being taken? Here are a few things that I learned or relearned.
- I took this directly from the presentation. In 2000 deaths from prescription medications began to rise, in 2008-2010 that increase flattened out. How come? Well, the rise in 2000 was a result of our national thought leaders telling physicians that pain was a 5th vital sign [1] and that for too long we had not met our patient’s needs. As a result, prescribers began more readily to prescribe pain meds – just as our leaders recommended. And the pharmaceutical companies seeing increased demand formulated new products, such as OxyContin, which contained a large dose of oxycodone and became heavily abused, resulting in many addictions. In 2008-2010 those drug formulations changed [3] as did the thought leader’s view of that 5th vital sign. Now, we w
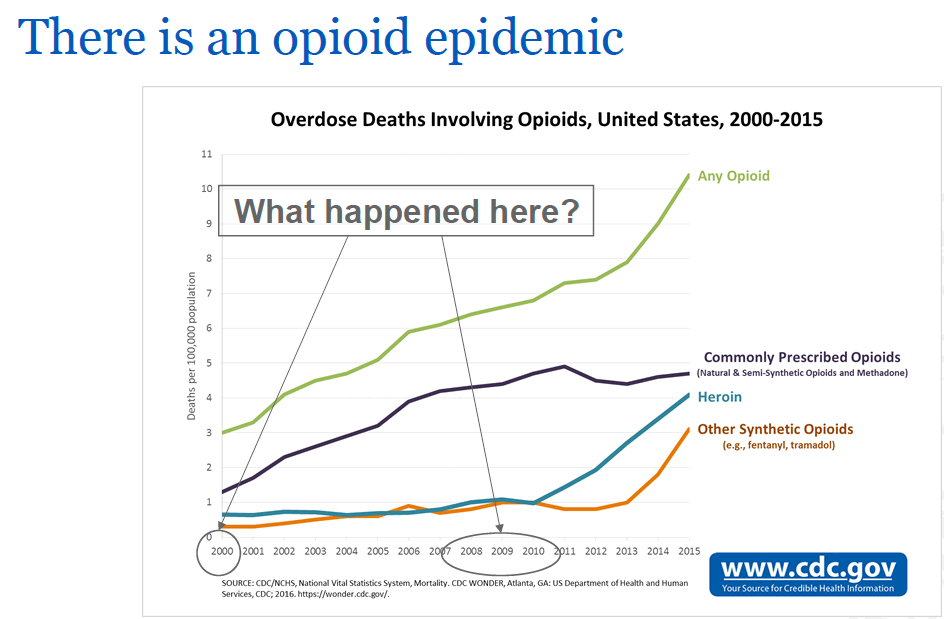 ere instructed that we had, perhaps swung too far the other way writing too many pain prescriptions and should be more restrictive in our prescribing habits for pain medications. As physicians reduced prescriptions patients and abusers sought alternatives. And unfortunately, the market provided lower costing substitutes, heroin and fentanyl which are now the primary cause of opioid deaths in the U.S.
ere instructed that we had, perhaps swung too far the other way writing too many pain prescriptions and should be more restrictive in our prescribing habits for pain medications. As physicians reduced prescriptions patients and abusers sought alternatives. And unfortunately, the market provided lower costing substitutes, heroin and fentanyl which are now the primary cause of opioid deaths in the U.S.
- Pain medications do not necessarily eliminate pain, although they can. More often they reduce the perception of pain by patients on average by about 30%. We need to tell this to our patients so that their expectations are more closely matched to the outcome.
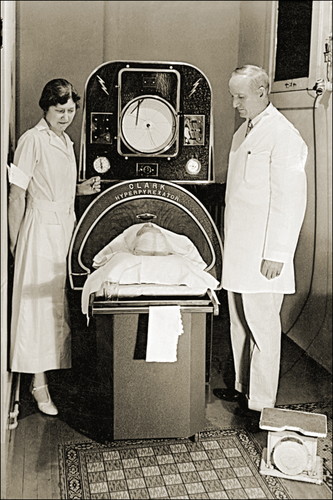
- “We will not be able to treat our way out of the epidemic.” Here is their analogy. Detox programs, rehabilitation, methadone maintenance are all important but are primarily methods of damage control. Prevention by education and careful prescribing has a greater chance of success. They harkened back to the 1950’s when polio was a real disease with real consequences for our population. [2] The treatment for some forms of polio involved an iron lung. The polio epidemic was not solved by buying more iron lungs, but by preventing polio. Same for opioid addiction.
- “Palliative care focuses on quality of life issues.” This for me was a critical point. Palliative care does not exclude curative care but has a significant role in any chronic illness. One way we can improve health outcomes is by including consideration of quality of life issues when we treat any chronic disease. That means increasing services that enhance life, Meals on Wheels, home visits by nurses or therapists, creating environments where the chronically ill can stay at home rather than burden emergency rooms or hospitals. Palliative care is not a replacement it is a necessary adjunct in caring for those with chronic illness.
- And a few definitions that might be helpful in understanding addictions. Tolerance refers to a physiologic adaptation that results in us requiring more medication to get the same outcome. Physical dependence is manifested when you have symptoms of withdrawal (dis-ease, faster heart rate, palpitations, restlessness, anxiety) when a medication is withdrawn or the dose lowered. Finally, addiction – behaviors that demonstrate impaired control over drug use, frequently resulting in harm to you physically or to your relationship with others.
Overall, New York’s health officials are making some good points and trying to make a difference. Good for them.
[1] Heart rate, respiratory rate, temperature, blood pressure are the four other vital signs.
[2] Few people today remember this period, and that is part of why anti-vaccination advocates can gain any foothold.
[3] Abuse resistant OxyContine was approved in 2010




