When is it time to put the scalpel (or stethoscope) down? In an era of rising life expectancies and changing attitudes towards the when and if of retirement; when 23% of physicians are over 65, and there are physician shortages, are there guidelines for what a doctor can or should do? Much about the current state of the ‘aging’ physician is discussed in an article The Aging Physician and the Medical Profession A Review in JAMA Surgery by Dellinger, Pelligrini, and Gallagher.
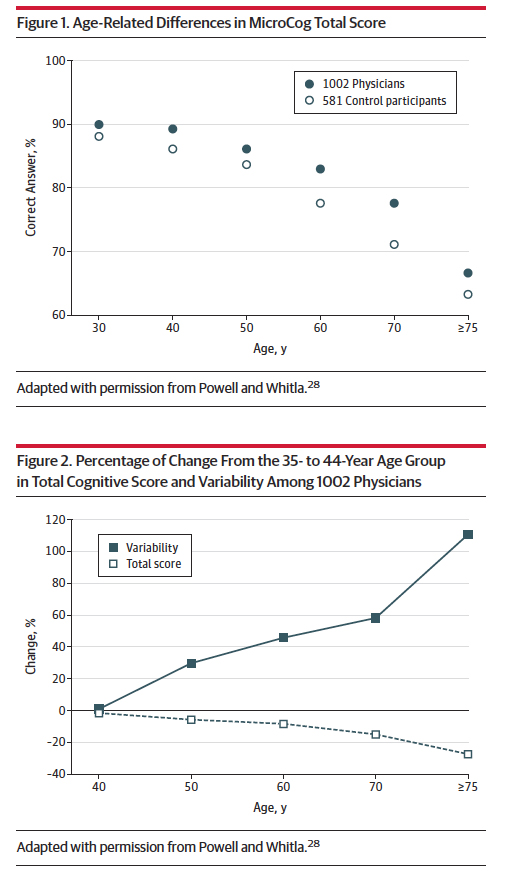 The two graphs, taken from the article, effectively summarize the science. 1002 physicians and 581 age matched controls were given a simple test of cognition. While physicians scored better than the controls, it is clear that both groups suffered cognitive declines over time. There should be no surprise to any of us. But it is the second graph that is more important. The variability of the cognitive scores increased dramatically with increasing age for the physicians – that is, as doctors age, many remain competent, some not so much. How do you manage this variability? Mandatory retirement, as is required of airline pilots, law enforcement officers and my favorite, ‘nuclear weapons couriers,’ would deprive many excellent physicians of an opportunity to continue to practice and potentially exacerbate the physician shortage. The American College of Surgeons (ACS) has recommended “voluntary and confidential baseline physical examination and visual testing for overall health assessment, with regular re-evaluation thereafter.” Interestingly, the ACS suggests that evaluating cognitive function be done “using online tools” and reminds surgeons of their professional obligations to disclose “concerning findings.” Cognitive decline continues to stigmatize even among health professionals.
The two graphs, taken from the article, effectively summarize the science. 1002 physicians and 581 age matched controls were given a simple test of cognition. While physicians scored better than the controls, it is clear that both groups suffered cognitive declines over time. There should be no surprise to any of us. But it is the second graph that is more important. The variability of the cognitive scores increased dramatically with increasing age for the physicians – that is, as doctors age, many remain competent, some not so much. How do you manage this variability? Mandatory retirement, as is required of airline pilots, law enforcement officers and my favorite, ‘nuclear weapons couriers,’ would deprive many excellent physicians of an opportunity to continue to practice and potentially exacerbate the physician shortage. The American College of Surgeons (ACS) has recommended “voluntary and confidential baseline physical examination and visual testing for overall health assessment, with regular re-evaluation thereafter.” Interestingly, the ACS suggests that evaluating cognitive function be done “using online tools” and reminds surgeons of their professional obligations to disclose “concerning findings.” Cognitive decline continues to stigmatize even among health professionals.
The cognitive studies mentioned do help guide policy, given the large variability of cognitive decline, a blanket rule-based on age would be inappropriate. Also, with increasing numbers of physician employees, the Age Discrimination In Employment Act prohibits mandatory retirement based on age. While we might develop national guidelines for when to begin testing physicians’ health, cognition, and competence, the considerable variability in the changes requires a more nuanced, local determination of what should be done for a particular physician. At this juncture, only three hospital systems have instituted mandatory health and cognitive evaluations. The difficulty in any such program and perhaps part of the reason that the ACS treated cognitive decline differently from physical or visual decline is “[Physicians] see their role as physicians as a treasured element of their identity.” Mandatory or “nudged” retirement can create a hole in a doctor’s life that golf cannot fill. I agree with the author's recommendation:
“…mandatory wellness testing and peer evaluation has the benefit of potentially identifying physicians whose competence is declining before patients are harmed and also connecting these physicians with programs that could restore their ability to practice safely. A local focus of such programs also makes sense given that institutions have much more robust information about a physician’s day-to-day practice performance than national organizations would.”
Having retired from clinical practice (neither mandated or nudged) I understand the anxiety and loss inherent in giving up a thirty-year calling. Many physicians still have the ability to contribute; they want to give back. It is incumbent upon the profession to find ways for retired physicians to continue to participate within their new limits. Peer review of patient care, helping patients navigate the health system, mentoring medical students and residents are all activities that require more physicians. The professional and the national societies have an obligation to the public to identify when physicians no longer “practice safely,” they have an equal responsibility to their colleagues to help them maintain their abilities and find meaningful ways to continue to contribute.




