It is impossible to spend a career in drug discovery research without having the following argument dozens of times:
Someone: "Drug prices are too high. We should break the patents and let generic companies make them cheaply."
Me: "Fine, but be prepared for innovation to come to a screeching halt. Companies are not going to spend billions of dollars to discover and develop new drugs if a generic company is going to start selling their products for a fraction of the price."
In fact, I made just this point in The Wall Street Journal back in 2012.
The problem with my argument is that it pits a current real-life situation (high drug prices) against a fuzzy and theoretical possibility – maybe a new treatment for something in the future. After all, people cannot possibly know what cures or treatments will be found 10 or 20 years from now, nor can they know what future malady they may suffer from or whether some new drug might treat it. This is human nature. A hundred-dollar copay is worth two in the bush. People simply don't want to have to pay high (and I agree, they are very high) prices for something now for something that may or may not happen in the future.
While the "drugs in the future" argument is largely theoretical to those paying high prices now, the discovery of the COVID-19 vaccines, arguably the most important medical advance in our lifetimes, changes the conversation. We are now talking about a real situation with real, immediate consequences. And these consequences could be catastrophic if President Biden succeeds in negating the patents of the three approved (U.S.) vaccines that are now going into arms and saving countless lives.
It is impossible to watch or read the news without hearing about the "South African variant" or "UK" (B.1.1.7) variants. Although the Pfizer-BioNtech vaccine is very effective against both of these, will it be effective against other variants, which will inevitably emerge in the future? No one knows.
As someone with a decade of antiviral research under my belt, I can tell you without reservation that (largely because of resistance) effective drugs for RNA viral infections are few and far between. The most effective (and important) drugs against RNA viruses are those that cure hepatitis C, a serious infection of the liver that has infected 170 million people worldwide. But the interval between the discovery of the virus and the approval of the first truly effective drug was 24 years, during which time billions of research dollars were spent as one drug after another failed, often in late-stage clinical trials (1).
Although the alteration of an mRNA vaccine to cover future variants is more like 2.4 months than 24 years it still raises the same question. If I'm Pfizer CEO Albert Bourla, I am going to be mighty reluctant to commit the time and resources to develop a modified vaccine so another company that incurred no development costs can undercut the price, effectively squeezing Pfizer out of the market.
This is not a theoretical argument. Below are the stock prices of Pfizer and Moderna following the Biden announcement.
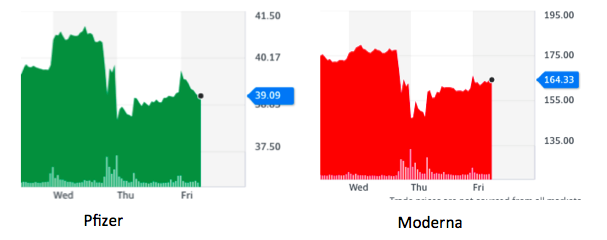
Biden is playing with fire. Pfizer, which took no money from the U.S., and Moderna, which spent $1 billion of its own before accepting $1.5 billion in aid from the U.S., are entitled to make a reasonable profit for their time and money. But if Biden is successful, can you think of any reason that either company would jump in again when/if a new resistant variant emerges, which is "immune" to the current vaccine? I can't. These are companies, not charities. There are a number of ways to ensure that poorer countries can be inoculated without penalizing the companies that were successful in discovering these amazing vaccines.
Think of what life would be like now without them. It's not pretty.
NOTE:
(1) The first really effective drug was Sovaldi, which was blasted by the press and consumers for costing $1,000 per pill. Not mentioned of course, was that (a) Gilead, the company selling the drug, was offering patient assistance and other discounts, and (b) even at full price the length of treatment – 12 weeks – meant that the cost would be $84,000. This is not very different than the previous treatment (IFN/ribavirin), which was given from 6-24 months, costing roughly the same over the course of the treatment, and had a success rate of about 40%, and came with intolerable side effects.




