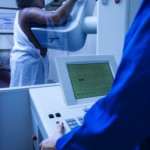
 The United States Preventive Services Task Force (USPSTF) stood firm to their 2009 recommendation that women should receive biennial mammograms from ages 50 to 75. The report also continues the party line that starting mammograms at a younger age (i.e. age 40) is a decision that should be made on the individual basis with input from a physician. The decision, which was made by reviewing all of the latest data on the utility and frequency of mammograms, also advises that there is insufficient evidence to make a recommendation for woman over the age of 75. Furthermore, the agency states that current data suggests that biennial mammograms are of the greatest benefit to women in their sixties.
The United States Preventive Services Task Force (USPSTF) stood firm to their 2009 recommendation that women should receive biennial mammograms from ages 50 to 75. The report also continues the party line that starting mammograms at a younger age (i.e. age 40) is a decision that should be made on the individual basis with input from a physician. The decision, which was made by reviewing all of the latest data on the utility and frequency of mammograms, also advises that there is insufficient evidence to make a recommendation for woman over the age of 75. Furthermore, the agency states that current data suggests that biennial mammograms are of the greatest benefit to women in their sixties.
USPSTF co-chair Michael LeFevre MD described the updated recommendations as more along the lines of if it ain't broke, don't fix it,' than it is a paradigm shift and it certainly appears so. However, there were some changes to the 2015 iteration. Most notably there is an absence of information on self-breast exams. The decision to omit this language is not, according to LeFevre, to discourage women from reporting irregularities in their breasts to their physicians, but to remove confusion generated from the 2009 report, which cited some evidence that suggested self-examinations might do more harm than good. Also new to the report is a mention of a variety of adjunctive and advanced screening tests, such as tomosynthesis (3-D mammography). However, the USPSTF only notes these to point out that to date there is insufficient evidence to recommend these be added to the biennial mammograms.
The initial USPSTF recommendations set off a whirlwind of controversy particularly for its recommendation against women receiving routine mammograms before age 50 and against annual mammograms in favor of biennial ones. We here at the ACSH have written about the controversy extensively in the past. The main point of contention critics of more frequent mammograms find is that the more you screen for cancer, the more cancer you will inevitably find, which is problematic because many of the detected masses will go a lifetime without being detrimental to a woman s health.
ACSH s Dr. Gil Ross weighs in: While it seemed counter-intuitive when these recommendations first came out, I d have hoped that both American women and their doctors would have gotten more comfortable with them by now. The concept that too much screening is no good for you should be acknowledged: too many women were getting biopsied and even having their breasts removed for non-problems, and this had to stop. It s a bit hard to realize that over-diagnosis and over-treatment can be worse than not enough, but that s the situation, and the Task Force should be commended for re-evaluating the evidence and sticking to their guns.


