A group called "World Action on Science and Health" (WASH) has declared March 20-26 as "Salt Awareness Week;" their goal being to encourage people all over the world to cut back on their salt consumption. The ostensible aim of this move is to improve health by getting people to consume no more than 5 grams of salt per day. Since salt is 40 percent sodium (the component that's the real target), that would be 2,000 mg of sodium daily. And in kitchen terms, one teaspoon of table salt would be about 2400 mg of sodium. That's not a lot of salt!
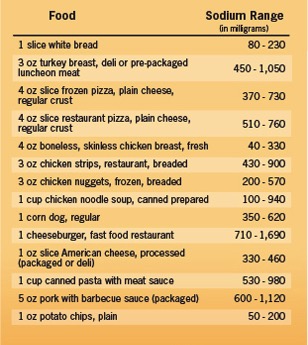
However, most of the salt we consume doesn't come from the salt shaker at meals. Instead, it's already present in most of the processed foods we eat, as shown below (courtesy American Heart Association): Hard to believe one slice of white bread can contain as much sodium as an ounce of potato chips!
 And although WASH won't tell you so, there really isn't strong evidence that this degree of restriction is right for us all. The point of such restrictive sodium guidelines is to reduce the incidence and prevalence of high blood pressure (hypertension), which in turn would decrease the occurrence of stroke and heart attacks. But it isn't that simple, according to information summarized in a recent ACSH publication —
And although WASH won't tell you so, there really isn't strong evidence that this degree of restriction is right for us all. The point of such restrictive sodium guidelines is to reduce the incidence and prevalence of high blood pressure (hypertension), which in turn would decrease the occurrence of stroke and heart attacks. But it isn't that simple, according to information summarized in a recent ACSH publication — Does "Excess" Dietary Salt Cause Cardiovascular Toxicity?
In that document, Dr. Lila Abassi reviews the relevant epidemiological evidence relating dietary salt and hypertension/cardiovascular disease. She notes that for people with severe chronic heart failure, having too low blood levels of sodium is associated with reduced survival.
Further, Dr. Abassi also reviewed the results of three large population-level studies which don't lend much credence that sodium restriction should be the goal for all. In the Trials of Hypertension Prevention, there were initially reductions in the risk of cardiovascular outcomes, but these were not maintained long-term. In another large, international study, which measured sodium excretion, there were increased risks of adverse cardiovascular events for people with both high and low levels of excretion. But in this study, there was no intervention —i.e. no group that changed their amount of sodium intake. Finally, a meta-analysis of over 100 randomized studies, found no direct link between sodium reduction and mortality, even though there was a significant inverse relationship between dietary sodium reduction and blood pressure reduction.
At best, from these studies, one might say that both very low and very high sodium intakes seemed to be associated with adverse outcomes. These results don't give one a lot of confidence in the advice that everyone should be on a sodium-restricted diet.
The best advice? Moderation, and attention to your risk factors such as family history of hypertension or cardiovascular disease, and your medical history. But driving yourself crazy to meet these very restrictive guidelines is unlikely to prolong a healthy life.




