Several years ago, a school bus full of elementary students in Massachusetts was evacuated. A potentially deadly item was found on the floor. Was it a gun? A bomb? A blood-contaminated hypodermic needle?
No, it was a peanut.
Over-the-top responses to peanuts aren't uncommon. People are under the impression that the mere whiff of a peanut is enough to send some kids to the emergency room. But, that's simply not true. The molecules in peanuts that are responsible for aroma are not the same as the ones that trigger allergies. Also, an allergic reaction only occurs if peanuts are eaten or inhaled; touching a peanut briefly will not trigger an allergic reaction, unless the child then rubs his or her eyes or mouth.
High-profile stories (such as the one about a woman with an extreme peanut allergy who died after kissing her boyfriend) lead the public to think that this sort of thing occurs regularly. But it does not.
A commonly cited statistic is that 150 to 200 Americans die from peanut allergies annually. However, that figure appears to be a back-of-the-envelope estimate with little evidence to support it. Journalism professor Meredith Broussard reported that merely 11 Americans died from all food allergies combined in 2005. Even if the larger estimate is true, it's still five times fewer than the number of people who die falling out of bed1, and it's roughly equivalent to the number who die from autoerotic asphyxiation.
Peanut-Free School Zones Don't Work
Still, many will argue that going to extreme lengths to protect children who suffer from severe allergies is worth the hassle. Even if kids are unlikely to die, protecting them from anaphylaxis is worthwhile. Fair enough. That reasoning is precisely why some schools have implemented various types of restrictions or bans on peanuts. Do they work? No.
A new article published in the Journal of Allergy and Clinical Immunology surveyed schools in Massachusetts. They compared the rates of epinephrine administration (a proxy for anaphylaxis) from 2006-2011 between schools with various peanut restrictions and schools without them. Obviously, one would expect that schools with restrictive policies wouldn't need to use EpiPens2 very often. But that's not what they found. (See figure.)
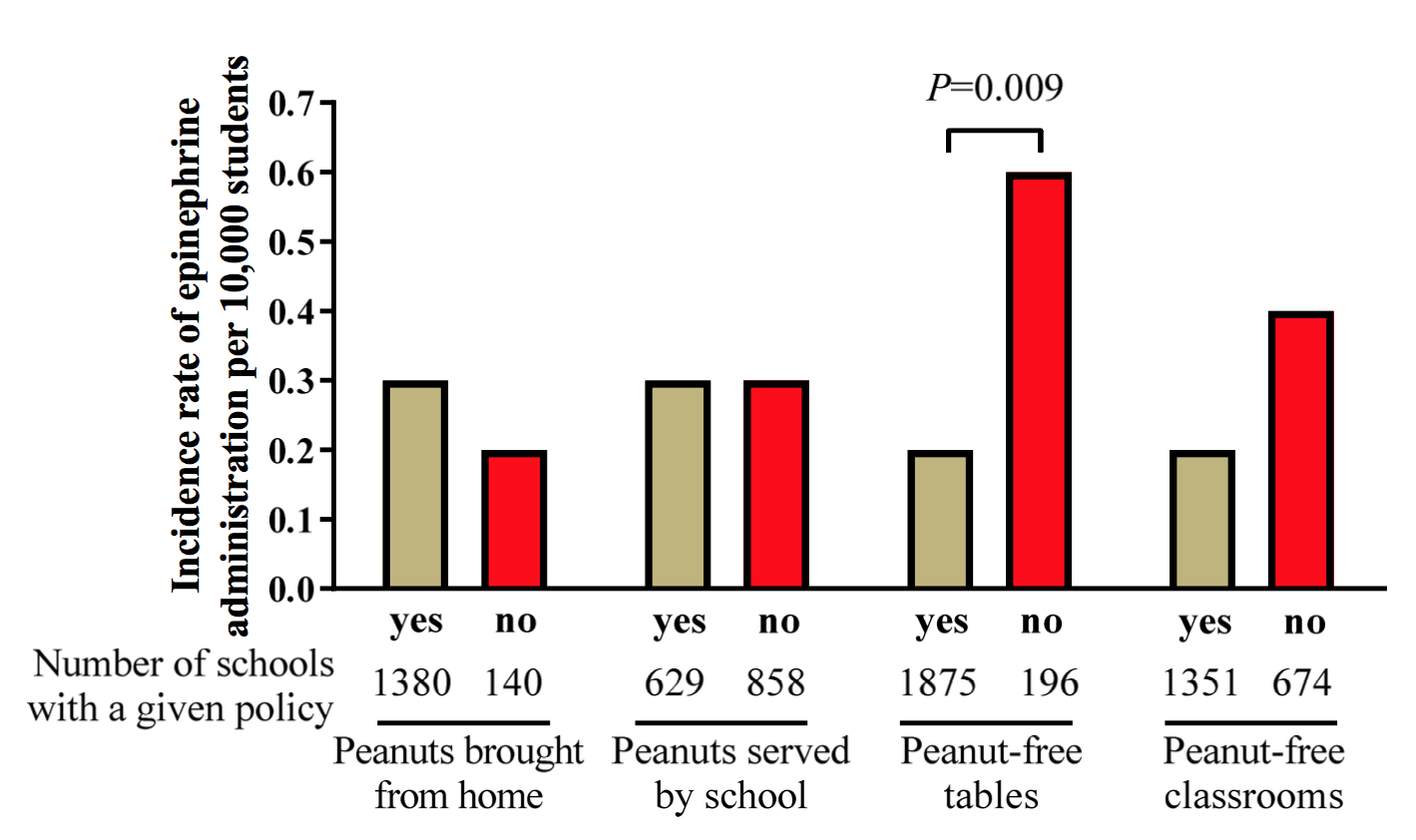
As shown, restrictive peanut policies don't reduce anaphylaxis. Furthermore, schools that were truly "peanut-free" (i.e., the school did not serve peanuts and banned students from bringing them) had the exact same rate of epinephrine administration as schools without those policies. The only policy that worked, the authors found, was for lunchrooms to establish peanut-free tables.
The temptation of society to ban things "for the public good" is incredibly strong. It would be nice, however, if less hysteria and more data factored into policymaking.
Notes
(1) According to the CDC, 922 Americans fell out of bed and died in 2015. To confirm that number, click here. After clicking "I Agree," select the year 2015 and ICD-10 code W06 (fall involving bed).
(2) EpiPens aren't the only epinephrine auto-injectors on the market. CVS is selling Adrenaclick to many patients for $10.
Source: Lisa M. Bartnikas, Michelle F. Huffaker, William J. Sheehan, Watcharoot Kanchongkittiphon, Carter R. Petty, Robert Leibowitz, Marissa Hauptman, Michael C. Young, Wanda Phipatanakul. "Impact of School Peanut-Free Policies on Epinephrine Administration." J Allergy Clin Immunol (in press). Published online: 2017. DOI: 10.1016/j.jaci.2017.01.040




