Monday night, comedian and late-night television host Jimmy Kimmel told the terrifying tale of the discovery and treatment of his newborn son's unexpected congenital heart defect. He began by reassuring the audience of a happy ending but was visibly overwhelmed by recounting his and his family's experience since Billy's birth. To view his heartfelt, emotional account, see video here.
Guided by Kimmel's recounting, we can generate a timeline that underscores the importance of routine hospital care in the perinatal period and why he was right to thank the entire medical team on air. It is important to understand this is a period of dynamic, continuous change in the infant . The cardiopulmonary (aka heart and lung) circulation in the pre- to postnatal period undergoes significant variability-- what was vital to sustaining life in utero (and its fluid-filled environs) is not necessarily needed upon entry into the oxygen-rich air. (1)
Below I will list the events that occurred and then define what it meant medically.
Jimmy Kimmel's Timeline (2):
- On April 21, 2017, my wife gave birth to a baby boy. Easy delivery, 6 pushes he was out. He appeared to be a normal, healthy baby.
The birth was a vaginal one given the pushing. Fast delivery in a mother who has had other children is quite routine. The body has memory. Due to the diverse complexity and wide spectrum of heart conditions in the pediatric realm, appearing "normal" after birth is not uncommon. There is a great capacity to compensate for many variants. They may be physically fragile, but biologically infants are quite resilient.
- Until about 3 hours after he was born, we were out of the delivery room, in the recovery room. Our whole family was there. We introduced him to his 2.5 year old sister. She was cute with him. We were happy. Everything was good. My wife was in bed relaxing.
The effects of labor and delivery can manifest after the act of birth. This is why it is important to deliver in a hospital setting and not jump on fads (see Water Birth: To Breathe or Not to Breathe?) as hospitals offer interventions if there are any issues. Though most babies are healthy, in general, if there is an issue -- especially one that involves potential deprivation of oxygen to crucial organs like the brain-- there should be no avoidable delays in care. The earlier the better, which is why hospitals and doctors have reduced infant mortality compared to a hundred years ago.
- A very attentive nurse found a heart murmur when checking him out, which can be common. And, he was a bit purple which is not common, and she asked me to come with her. My wife and I assumed it was nothing since our daughter had a heart murmur too and we didn't notice he wasn't the color he was supposed to be.
It is not uncommon for parents not to notice aberrations. For one, childbirth just took place, and that alone is riddled with adrenaline, excitement, fear, relief, exhaustion, more fatigue, and exuberance.
"A bit purple" can describe a host of conditions, everything from where there are too many red blood cells, thickening the blood and potentially leading to clots, to a purplish discoloration of the hands and feet which is a common finding in a healthy just born baby. (3) It is a nonspecific identifier and no one wants to send parents into a panic so doctors and nurses are constantly deconstructing all the signs and symptoms in the context of the type of birth, need for medical intervention, family history, maternal record, etc.
"Heart murmur" is also general, it can be benign or evidence of severe forms of cardiac conditions. By definition, it means that when listening to the heart an abnormal sound caused by turbulent blood flow is heard. When the sound is heard in the cardiac cycle and its intensity helps determine severity and significance. Some are routine, others ominous but a heart murmur in the first 24 hours of life is not necessarily pathologic. However, an EKG and echocardiogram (ultrasound of the heart) as well as X-ray of the chest, might be warranted.
- I accompanied Billy and the nurse down the hall to the Neonatal Intensive Care Unit (NICU) where another excellent nurse checked him out and called a doctor in…and now all of a sudden it felt serious… then doctors, nurses and equipment came in and they determined he was not getting enough oxygen to his blood…which as far as I understood at the time was one of two things… his heart or his lungs… and you hope it was lungs because sometimes they have fluid in them after delivery and it is potentially a minor thing, but they did an X-ray and his lungs were fine…which meant the heart wasn't fine…
Hospitals typically have a well baby nursery and a NICU. As you can gather by the terms, the former houses newborns with no issues (or minor ones) while the NICU is for any moderate to severe developments. There is usually not an in between or step down unit. Neonatologists (pediatricians who specialize in prematurity and illnesses of the newborn period in general) manage these divisions.
Checking the pulse oximetry (you will hear the term "pulse ox") is a noninvasive first measure to determine if the oxygen levels are sufficient. Assessing all four extremities (e.g. pulse, blood pressure) is critical when considering a congenital heart defect. Disparities can tip you off to disorders like coarctation of the aorta, for instance. Vital signs are extremely informative and help map out the ensuing plan. (See Do Vital Signs Wrong and Pay Ultimate Price).
An X-ray will determine if a heart looks too big on an initial surveillance. It can be obtained quickly and yield good information. It can also answer these and many other questions: Are the lungs adequately inflated or collapsed? Are the abdominal contents entering the thoracic region (aka chest)? Is the diaphragm displaced? Is there pneumonia or fluid where it shouldn't be? Are the ribs and bones intact? Is the anatomy normal? (4)
- More nurses, doctors and equipment came in, my wife was in recovery... it was terrifying, I was standing in the middle of very worried looking people. A pediatric cardiologist was called. Did echocardiogram (ECHO, sonogram of the heart) and found he was born with heart disease.
An ECHO is a noninvasive ultrasound of the heart. It is a very informative study in a newborn, especially given the fact babies this young don't move around a lot and don't have much subcutaneous fat so the images acquired are very useful.
- The heart disease is Tetralogy of Fallot with Pulmonary Atresia. It is hard to explain. His pulmonary valve was completely blocked and he has a hole in the wall between the left and right sides of the heart. Then, they brought my wife in and wheeled her in… told us what our options were. Transferred Billy to Children's Hospital Los Angeles by ambulance.
This diagnosis also covers a wide spectrum. The aspect of pulmonary atresia is a substantial one. Many factors influence who is more complex in the longer term. For example, what is the status of the pulmonary artery? How extensive?
The normal heart has two atria and two ventricles (or chambers) that make up the left and right components. It is a coordinated system that permits the masterful circuitry of routing deoxygenated blood from the body to the lungs where it can be oxygenated so as to be pumped back to the body to fuel and nourish our vital organs. This hole between the ventricles Kimmel refers to serves to erroneously mix the oxygenated and deoxygenated blood.
Tetralogy of Fallot consists of four components that occur in a vast range. Ventricular septal defect, a hole between the right and left ventricle mixing the blood that has oxygen with the blood that lacks it, giving the patient that purplish look. Pulmonary stenosis, is a narrowing of the outlet for blood from the right ventricle. The increased resistance to blood leaving the right ventricle along with the increased blood entering the ventricle because of the septal wall defect causes the right ventricle's muscle to get bigger, right ventricular hypertrophy. Finally, the aorta, the major artery carrying blood away from the heart is malpositioned and is above the septal defect rather than over the left ventricle.
It is important to identify these conditions before progression of secondary events. These days, prenatal ultrasound picks up these types of diagnoses much of the time, so plans are already in place before the primary hospitalization. However, as evidenced here, this is not always the case.
- Cardiac surgeon on Monday (4/24/17) morning opened his chest, fixed one of two defects in his heart…went in with scalpel, did magic couldn't even begin to explain, opened the valve and the operation was a success——longest 3 hrs of my life…they didn't do everything…he will have another open heart surgery in 3-6 months to close those holes, but they want to wait until he is bigger…and then a 3rd noninvasive procedure hopefully in his early teens to replace the valve he has now…
The outcome and prognosis depends on the extent of disease and repair and requires an expert surgeon trained in pediatric cardiac surgery. Babies are much tinier than adults, so interventions require calculations in milligrams per kilogram and precision. Too much force with oxygen can burst a lung. Feeding through an improperly placed tube can cause aspiration. And so on. The margin for error is extremely narrow in babies.
Managing intravenous lines, blood pressures, wound sites, anesthesia, heart rhythms and blood counts are among the huge litany of obligatory monitoring. This is partially evident by the following photo Jimmy Kimmel displayed:
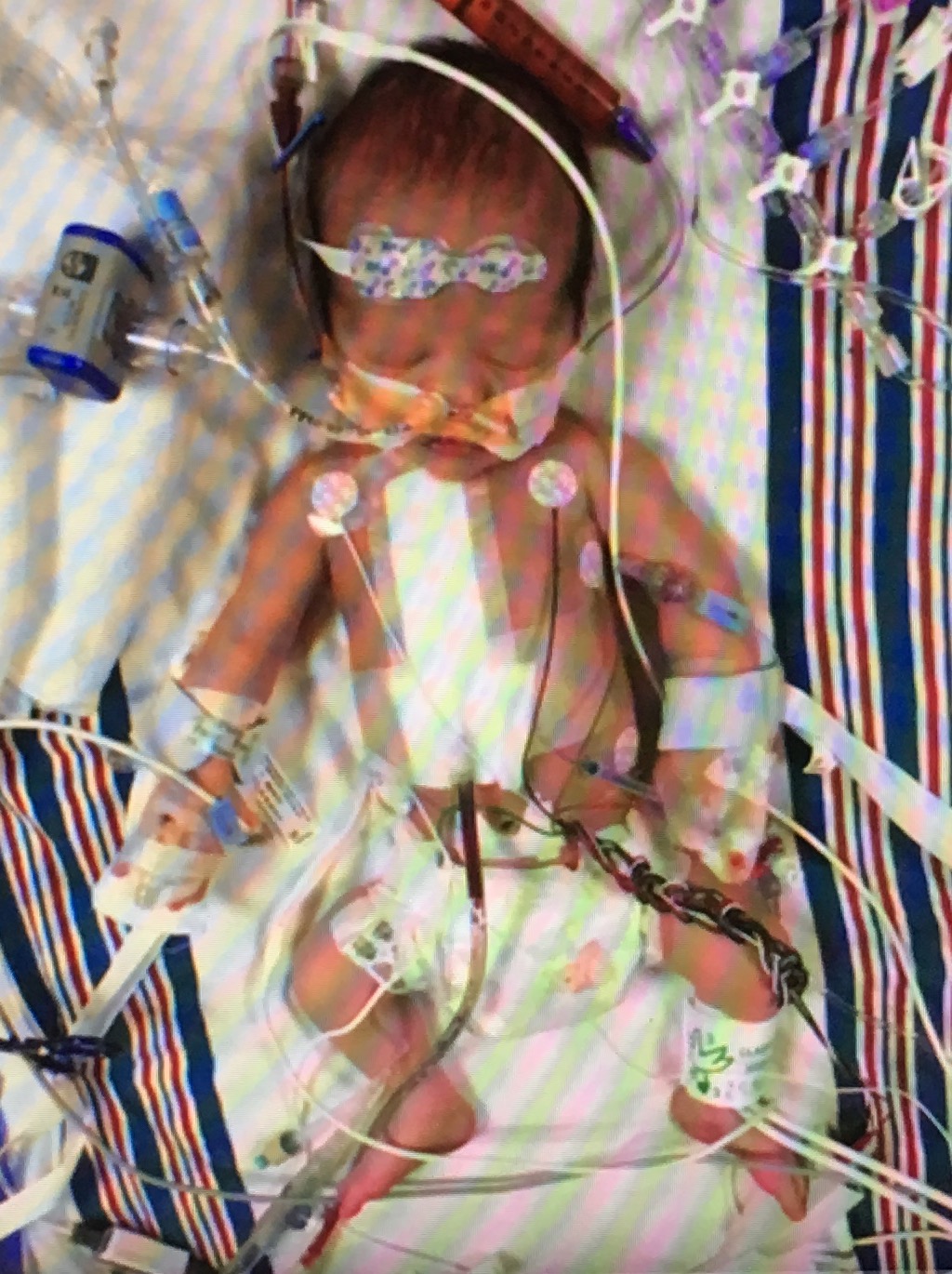
For those reasons, it is common to perform many surgeries when the infant is "bigger." The reality is the complications with anesthesia and the like are reduced the bigger the baby is since all dosages are based on a baby's kilogram weight. The more the baby weighs, the safer the procedure. Also, the size of the operative field and anatomy itself is larger as well.
- 6 days after open heart surgery we got to bring him home which is amazing, he’s doing great, eating, sleeping, peed on his mother…doing all things supposed to do…enormous team effort…
The fact the baby is home so soon is a fantastic outcome. Kimmel showed this photo to lighten the story of the ordeal:
What's next for the Kimmel family? The greatest indicators of well-being in a baby include the ability to eat, sleep, pee and poop well. If all of those activities are occurring with ease, it is very reassuring. If not diagnosed and partially corrected, an infant would demonstrate a failure to thrive (poor weight gain, growth), sweat upon feeds, turn blue or have difficulty breathing. Infants eating is like our going to the gym. It is their big workout. If problems arise in eating, heart disease is often a culprit.
The good news: Children with this condition and its accompanying spectrum do very well today but multiple surgeries are common. They are going to have long-term continued assessment by cardiac specialists. Kimmel had Shaun White on the same episode, a person with that diagnosis who not only went on to lead a normal, productive life, but to become an Olympian.
There may be some heart rhythm abnormalities but these can be readily treated today.
Notes:
(1) For example, inside the womb, the baby is nurtured via the umbilical cord. With delivery and cutting of the cord, the pressure differential changes in the heart and lungs upon first breath. Holes that remained open in the heart before birth start to close at known intervals in the newborn phase. Often, in the situation of a congenital heart anomaly, a hole remains open to compensate for the defect. For those that prematurely close in this context, the resulting impact is to imperil the infant.
(2) The bullet points are either directly taken or paraphrased from Jimmy Kimmel's (5/1/17) monologue. Photos within the article were obtained from screenshots of this video.
(3) The former is called polycythemia and can be caused by delayed clamping of the cord, for instance, and the latter named acrocyanosis.
(4) A "minor thing" that is not uncommon in newborns is to experience transient tachypnea of the newborn (TTN). This can often happen in an infant born via c-section or when a vaginal birth occurs rapidly - both scenarios involve limited to no time traveling through the birth canal so that extra fluid might remain delaying a baby's transition into the world. Routinely, some respiratory therapy and a little supplemental oxygen along with the passage of time can do the trick without any lingering effects.




