
In certain areas of the country, "tick checks" are an everyday activity - especially for the kind of ticks that carry diseases like Lyme disease. However, even if ticks are found and removed, it is not simple or easy to recognize if that tick left Lyme disease behind.
Now, new research published in Science Translational Medicine may lead to a new test that takes the guessing game out of diagnosing Lyme disease. Even better, it could distinguish Lyme disease from other tick-borne illnesses that share many of the same symptoms.
Lyme disease is caused by a bacterial infection with Borrelia burgdorferi, which is passed through the bite of the deer tick. The tick must be attached for 36-48 hours or more before the bacterium can be transmitted. The infection can result in the nonspecific flu-like symptoms of fever, chills, fatigue, and aches. But, the telltale sign is the rash known as erythema migrans - or bull's eye rash. The problem is that this rash does not appear in every case of Lyme disease or may be missed if it is located in a hard to see area such as the back. Alternatively, other bites, from a spider for example, may appear like a bull's eye rash to an untrained eye. The bottom line is that Lyme disease can be difficult to diagnose, even with a rash that resembles the the bullseye rash.
A group from Colorado State University is working on this problem. They sought to find biomarkers (or signs in the body of changes in the metabolism) of people infected with Lyme disease versus people infected with southern tick-associated rash illness (STARI). Because STARI and Lyme disease are caused by different bacteria (the bacteria that causes STARI is unknown, but, has been shown to not be caused by B. burgdorferi) their infections elicit different responses in our bodies. They used mass spectrometry to analyze the blood serum of patients.
After analyzing the differences in the levels of metabolites in patients with Lyme and STARI, the researchers were able to create a profile of differences that could differentiate between the two. In doing so, they identified the type of illness in each patient with startling accuracy - 98 times out of 100. Not only that, they could then use that profile to identify an infection - by comparing infected people versus healthy people.
This type of technology is being used more and more. We wrote about a similar method just a few weeks ago, being developed to distinguish between a bacterial infection and a viral infection. Researchers are not looking at the differences in the pathogen anymore, but, in our bodies' response to that pathogen. Developing these technologies may lead to incredibly important diagnostic advances in the future.
Lyme disease is a growing concern in certain parts of the country, with roughly 30,000 new cases reported each year. Although 95% of the cases of Lyme disease were from 14 states (see map below and note #1) in 2015, the range is growing with each year, as is the number of cases.
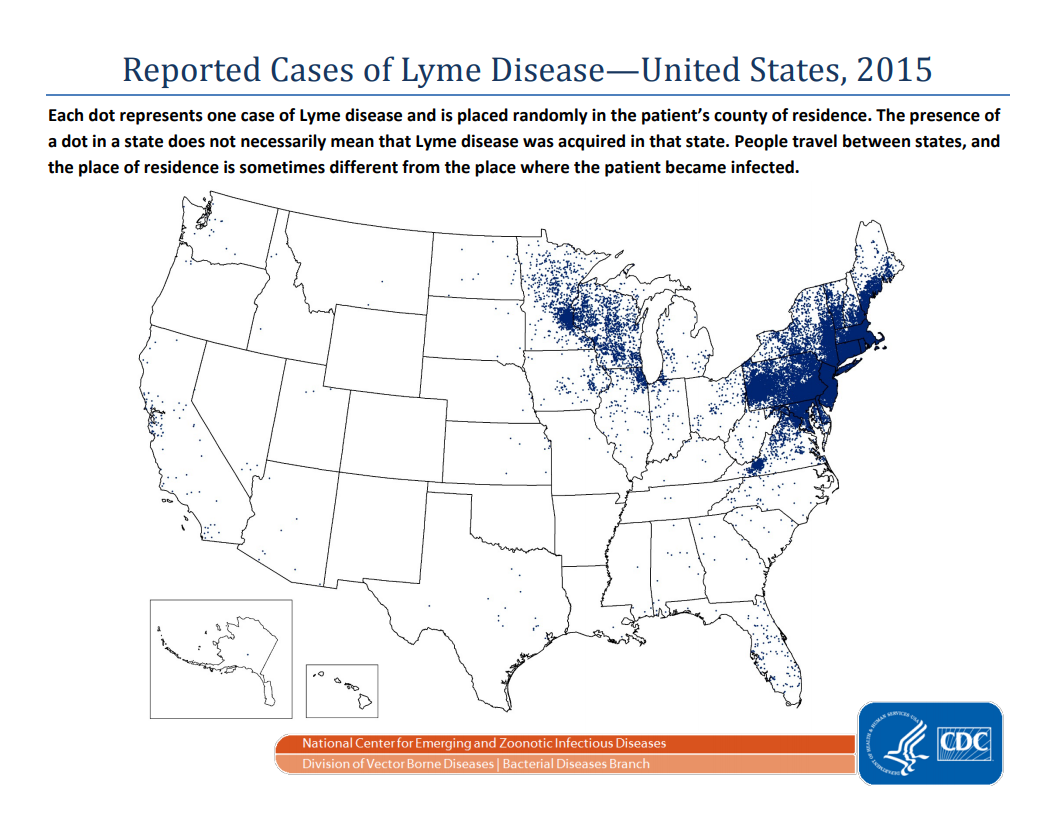
Notes:
(1) The 14 states are Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, Wisconsin.
References:
C. Molins et al. Metabolic differentiation of early Lyme disease from southern tick‒associated rash illness (STARI). Science Translational Medicine. doi:10.1126/scitranslmed.aal2717



