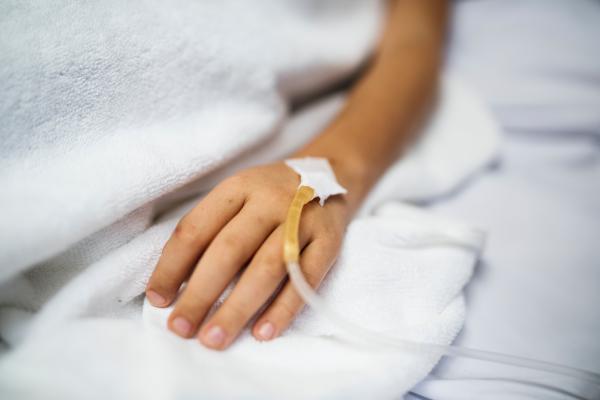
Making the rounds in the news media is a serious medical condition called acute flaccid myelitis (AFM). It predominantly occurs in children causing among other symptoms weakness in the extremities. In many reports, it is being likened to polio due to its potential to lead to paralysis. Given the disease impairs a person’s neurological system, in particular affecting certain areas of the spinal cord, its impact on a patient varies in the extent of diminished strength of one’s muscles and reflexes as well as in their long-term recovery.
This all sounds very scary, but let’s put the disorder into context so as to assuage some fears.
For instance, the Centers for Disease Control and Prevention (CDC) estimates less than 1 in a million people in the U.S. will annually develop AFM. And though the condition is not new, we are learning more and more about it and the CDC is monitoring these patterns closely, especially since spikes in cases began around 2014. Doing so will ultimately narrow the knowledge gap.
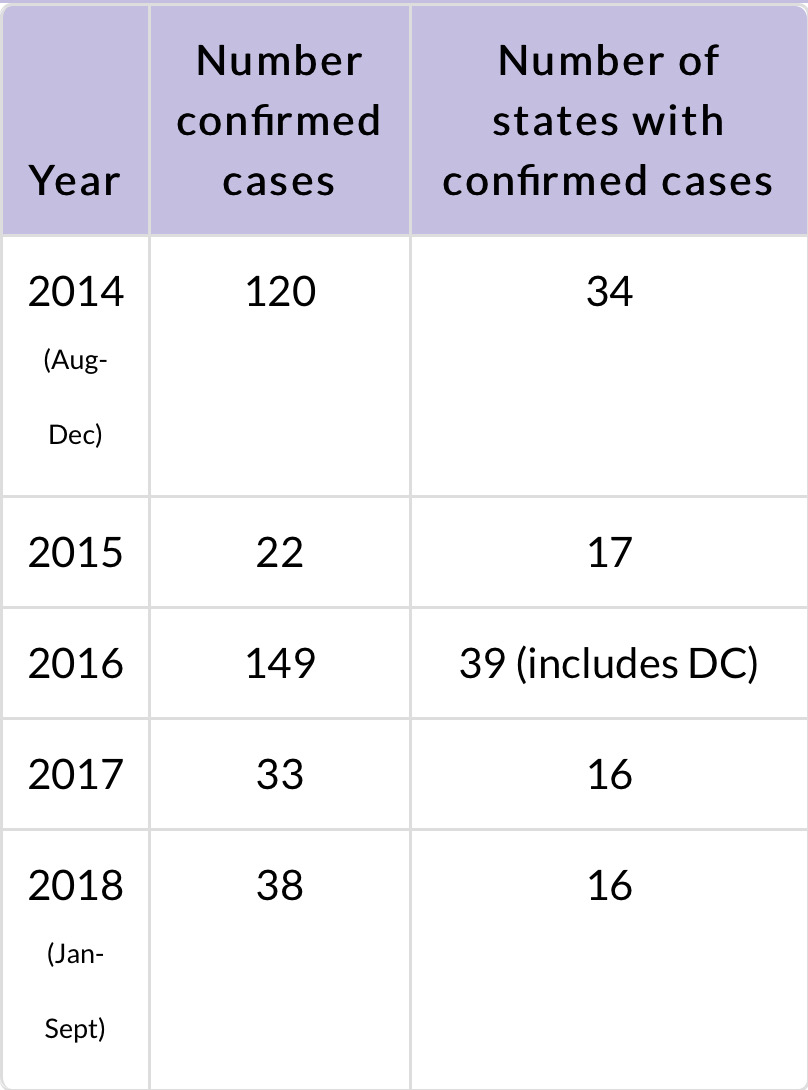
To put your concerns into perspective, here is a chart from the CDC documenting the trends in cases from 2014 until the present 38 in 2018 so far. As you can see, 2016 reflects a peak of 149 cases extending into many more states than other years, including the present one.
How to make sense of AFM
As much as we all would like, it is impossible to eliminate all risks of all things especially when unknowns enter the mix in a condition like this. And it is human nature for calm around relative risk to go out the window when we find ourselves personally influenced by falling into the wrong side of the ratio. That said, awareness is very important for a host of obvious reasons, including but not limited to understanding what to look for thereby being able to benefit from early medical intervention and the scientific community’s gathering of knowledge about AFM’s behavior so as to guide even more effective prevention efforts.
AFM and similar neurological conditions can be caused by a variety of factors: viruses, genetic disorders or exposures to toxins. Because its symptoms can mimic other maladies (e.g. Guillain–Barré Syndrome, transverse myelitis), diagnosis can be challenging. But, with the help of proper physical examination, imaging studies and testing, a doctor can readily discern the diagnosis. The good news is with the current media attention shining a light on this issue, AFM will be put into the forefront of a doctor’s mind. As a result, AFM will be readily considered in scenarios where sudden onset of arm or leg weakness is involved.
Like many other conditions, the individual is the variable. Some will have swallowing difficulties, others facial droops and in the extreme breathing issues that require more aggressive intervention. However, many do recover quickly. Thankfully, AFM is not very common and though we don't know yet why some people progress to require protracted care, the situation is being closely studied and tracked by scientists. Our understanding is expanding as a result.
What are some active steps to take
Because the cause of a person’s AFM is not always known, we do know that polio and West Nile Virus have been culprits for some cases. Staying current with vaccines, albeit polio or the flu, is a proactive measure in general to remain healthy. Following infection control measures during this cold and flu season especially is always of benefit – e.g. frequent hand-washing, keeping hands out of your mouth and not rubbing your eyes. Implementing precautions (see here) to avoid mosquito bites that transmit disease are worthwhile.
Preventing everything untoward is unfortunately unrealistic, but preoccupying ourselves with "what ifs" and worry about each and every disease that manifests is also not a productive step in living a full, meaningful life. Keeping yourself informed and current about risks is important, as is finding ways to minimize stress. Focusing on balancing those worthy goals is the most ideal while science, as it advances, bridges the gap.