The United States has failed on so many fronts. There was a lack of intelligence during the early days of the epidemic in China. A lack of preparedness for testing that directly led to our current situation. A national stockpile of supplies exists just for events like COVID-19, but it is woefully undersupplied and, clearly, our plans for re-supply are completely inadequate. Let's review the history of our approach to pandemic preparedness and the current testing debacle.
We have now locked ourselves down for the last two weeks. Happily, we’re not in New York City. But we are unable to read the news every day and observe the lives of family and friends without anxiety bordering on depression. Personally, I am angry, and I want to share the source of my anger with you while emphasizing the things that we can do differently for the next emerging infection. None of what I will discuss has not been previously contemplated or foreseen. None of what is happening is a surprise, but it is so unnecessary.
The US has failed on so many fronts.
There was the lack of US intelligence during the early days of the epidemic in China and the lack of attention to the intelligence on the seriousness of the infection during January.
There was a lack of preparedness for testing that directly led to our current situation of sheltering in place.
We have a national stockpile that exists just for events like covid-19. But it is woefully undersupplied and, clearly, our plans for re-supply are completely inadequate.
We continue to underfund state and local public health facilities and workers.
Today, though, I want to briefly review the history of our approach to pandemic preparedness and the current testing debacle.
Inspired, mainly I think, by Josh Lederberg’s report from the American Academy of Medicine in 1992 on the threat of emerging infections, experts began to seriously consider the possibility of a worldwide health crisis caused by a new (or even old) infectious agent. I was fortunate to have been asked to join Dr. Lederberg’s Forum on Emerging Infections of the National Academy in the late 1990s. We reviewed public health capabilities in the US, in other developed countries and in the developing world. We found that all were seriously underprepared to deal with anything like the kind of infectious disease we were considering. In all cases, including that of the US, we identified gaps in current infrastructure making observations on how these could be addressed. (As a “Forum” we could not write reports or make specific “recommendations.”) After 9/11/2001 and the following anthrax attacks we reviewed preparedness for biological and chemical attacks against the US on a larger scale. These deliberations shared considerable overlap with our previous reviews of public health capacity. We constructed models and projections of the effects of such attacks. Later, after having dealt with SARS, MERS, Ebola and Zika, the Academy released a report on pandemic planning in 2016 where improvements in global public health infrastructure and preparedness were emphasized. All this as well as experience with an H1N1 pandemic and the emergence of avian flu led to the development of a pandemic playbook during the Obama administration. Please note that this history spanned the administrations of Clinton, Bush, Obama and now Trump – republican and democratic.
One of the key components of preparedness is the availability of detection systems that provide early information on emerging infections that might become pandemic. In 2010 and again in 2016, reports examined progress in timeliness of identifying outbreaks and in communicating their existence. The authors found that, overall, the world community had improved from 2000-2010 but very little since then. Lagging regions included the Americas, Europe and South-East Asia. (Hmmmmm). In the 2016 Academy of Medicine report, it was recommended that the WHO take responsibility for detection and coordination of a global response.
This brings us to covid-19 and its beginnings in China. We now know that the outbreak began in November 2019 in the Hubei region of China among customers of wild animal markets. Local authorities were aware of clusters of pneumonia in the region but apparently were reluctant to report this. China did not acknowledge the outbreak until late December. The WHO announced the outbreak on January 5. According to the Washington Post, US intelligence agencies had been warning about the potential of this infection since early January. (One might ask where US intelligence was during December). On January 18, Secretary Azar (of HHS) was trying to convince President Trump about the potential seriousness of this outbreak. By the third week in January, we were repatriating diplomats and others from Wuhan and the Hubei Province. On January 31 travel from China to the US was restricted to US citizens and permanent residents and their families. Somebody in the administration recognized the danger posed by this virus.
Business Insider has published an informative timeline on testing. By January 10, the sequence of the virus was published. With the nucleic acid sequence in hand, diagnostic testing became possible. One week later, the first diagnostic testing kits were available. By February 6, the WHO had shipped 250,000 test kits to 159 countries. South Korea, as soon as the news of the virus from China was available, invested heavily in the manufacture of kits so that when the sequence was available, they could deploy testing to the population on a large scale. As used in South Korea, the test took about 10 minutes to complete and individuals had their results within one day. The US, for reasons that escape me, decided they would develop their own test and that it would be run at first at the CDC and later at state public health labs.
 Once the CDC had their test approved by the FDA, they shipped it out to the state labs – but it was faulty in spite of having passed an FDA approval process. Then, instead of immediately approving other tests for use in this emergency situation, the FDA continued to rely on its usual stodgy protocols for approving diagnostic tests. While I agree that we need the FDA to assure us that the tests are going to be accurate and useful, we also need them to have a way of accelerating their process in response to a public health emergency. They can do this but chose not to for another month. Then again, their initial approval of the CDC test was not such a good precedent either.
Once the CDC had their test approved by the FDA, they shipped it out to the state labs – but it was faulty in spite of having passed an FDA approval process. Then, instead of immediately approving other tests for use in this emergency situation, the FDA continued to rely on its usual stodgy protocols for approving diagnostic tests. While I agree that we need the FDA to assure us that the tests are going to be accurate and useful, we also need them to have a way of accelerating their process in response to a public health emergency. They can do this but chose not to for another month. Then again, their initial approval of the CDC test was not such a good precedent either. The problem with this US response is that it flies in the face of basic epidemiologic principles (unless things have changed in the last 25-30 years). The ideal way to deal with an outbreak is to identify cases and then their contacts and quarantine them for the incubation period. The first US case was reported January 22. Without widespread testing, we were unable to identify cases and therefore unable to quarantine contacts. This allowed the disease to spread throughout the US.
South Korea instituted very wide testing of the population testing 3500 people per million population. Even today, we are testing a measly 240 or so per million. South Korea’s test results were available within minutes to 24 hours. Our test results still come in about 5 days later. South Korea also used cell phone localization data to track movement of identified cases and to warn those whose phones had been in the vicinity of the confirmed case. They used police to supplement health care workers in testing and searching for contacts. They were able shut down the epidemic without having to shut down the country. Of course, their epidemic started and was centered around specific church in a specific geographic area of the country so perhaps their task was a little easier than it is in our vast country.
Like South Korea, Hong Kong, Taiwan and Singapore were all able to test widely and keep the epidemic controlled without shutting down their economies.
One of the major problems with the covid-19 virus is that about 30% of all transmissions are from asymptomatic or minimally symptomatic people. This means that very widespread testing would be required to identify all the cases. But other countries have succeeded anyway.
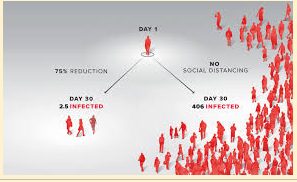
This delay in widespread testing, case -finding and contact isolation has left us with only one solution – social distancing. Our only way out of this current state of affairs involves widespread testing, case identification and contact isolation. We are nowhere near where we need to be.
In my next blog – to follow soon – I want to discuss the role that the strategic national stockpile could have played in helping to control the outbreak in the US. And I want to explore our support for the local public health facilities and workers on the frontlines in the US and how that could have been so much better than it has been.



