There may be around 200 different viruses that cause the common cold.
One of the major kinds, known as rhinoviruses, causes roughly one-third of all common colds in adults. Four different strains of coronavirus cause about 20% of common colds. Exact numbers are difficult to come by because, quite frankly, scientists didn't really care about the common cold until COVID-19 came around.
The four coronaviruses that cause the common cold are called 229E, NL63, OC43, and HKU1. The coronavirus that causes COVID, now known as SARS-CoV-2, is something else. But it's not entirely different. After all, it's still a coronavirus, so the genetic sequences are pretty similar. That begs the question, "Can infection with a common cold coronavirus help prevent COVID?" The answer might be yes, at least for severe cases.
A team of researchers led by Manish Sagar at Boston University performed a retrospective cohort study using medical records from 15,928 patients who had undergone a comprehensive respiratory exam at some point between May 2015 and March 2020. This exam determined if patients had been infected with many different pathogens, including the coronaviruses that cause the common cold (referred to as endemic coronavirus or eCoV). Patients were then split into two groups based on whether they had (n = 875) or had not (n = 15,053) been infected with eCoV at some point in the previous five years.
Before they began their analysis, the authors first needed to determine if there were any significant differences between the two groups, for example, if the eCoV+ group (i.e., people who had an endemic coronavirus infection) were sicker than the control group (eCoV-). Overall, they were just as healthy as the control group, with the exception that the eCoV+ group was slightly likelier to have HIV.
Since there were essentially no major differences between the two groups, the authors could then ask the big questions: What happened to the patients in the eCoV+ group? Were they likelier or less likely to get COVID? If they got COVID, how bad was it? The table below shows their results:
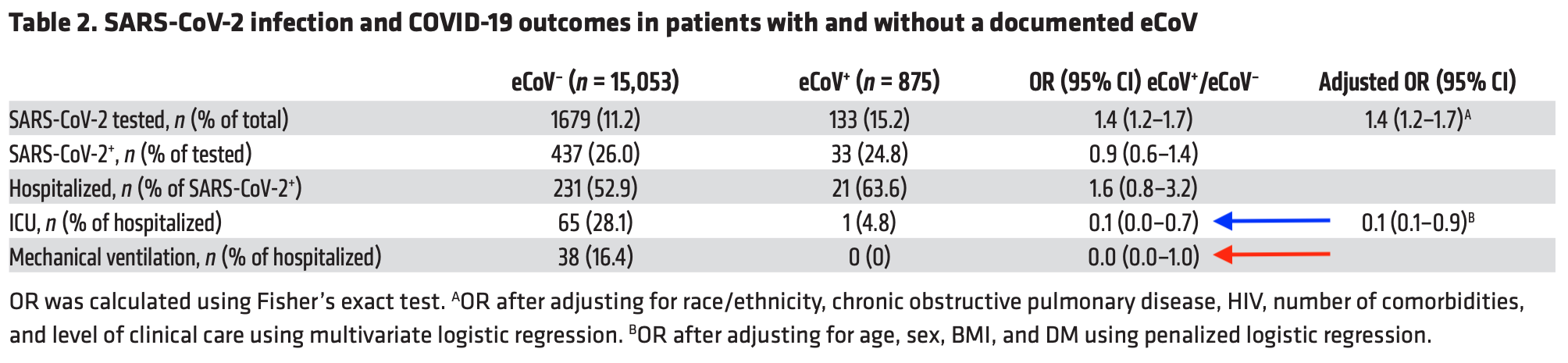
The second and third rows show no statistical difference between the groups when it came to testing positive for COVID or being hospitalized for COVID. In other words, patients who had a previous common cold coronavirus infection (eCoV+) and patients who had not (eCoV-) were both equally likely to test positive for COVID and/or be hospitalized.
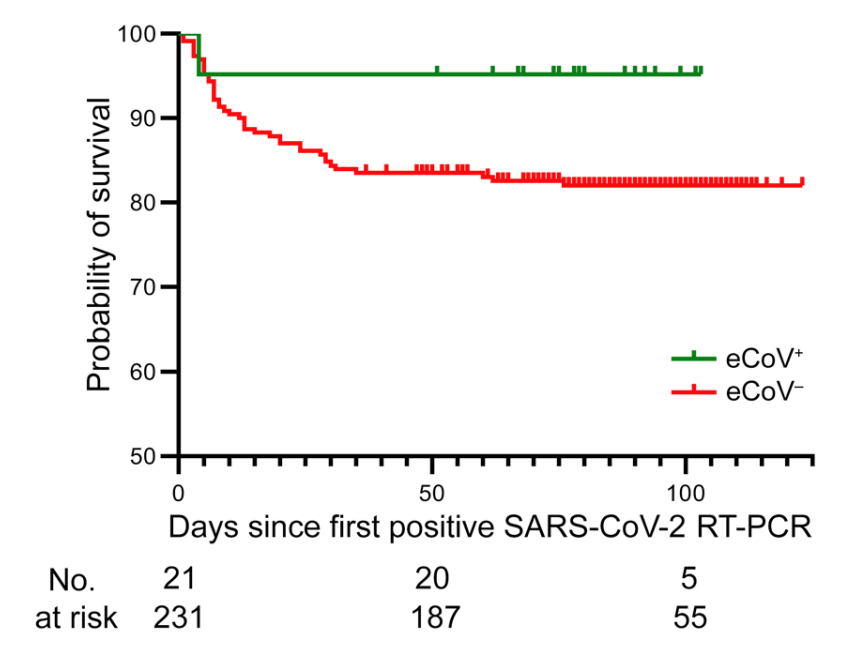 However, the eCoV+ group did far better when it came to their experience in the hospital. Those with a previous common cold coronavirus infection were far less likely to be put in the intensive care unit (ICU) or to require a ventilator (the former was statistically significant but not the latter). The authors also found that previous infection decreased the likelihood of death among hospitalized patients, but this result was also not statistically significant after being adjusted for various factors. (See figure.)
However, the eCoV+ group did far better when it came to their experience in the hospital. Those with a previous common cold coronavirus infection were far less likely to be put in the intensive care unit (ICU) or to require a ventilator (the former was statistically significant but not the latter). The authors also found that previous infection decreased the likelihood of death among hospitalized patients, but this result was also not statistically significant after being adjusted for various factors. (See figure.)
Combined with what other researchers have found, it is safe to conclude that the more mild coronavirus strains that cause the common cold confer some protection against severe COVID. That might make the sniffles a little more tolerable.
Source: Manish Sagar, et al. "Recent endemic coronavirus infection is associated with less-severe COVID-19." J Clin Invest 131(1):e143380. (2021) DOI: 10.1172/JCI143380



