For decades, HIV sufferers were bereft of effective treatment. In 2001, five years after their tenofovir disoproxil fumarate (TDF) drugs were patented, Gilead Pharmaceuticals received FDA approval, and the drugs became prescribable.
Gilead
If you grew up in the middle of the early AIDS epidemic as I did, something I've written about firsthand, the results of a study on a tw
The case in question concerned Gilead’s drug Tenofovir, widely prescribed for the treatment of HIV and Hepatitis B.
“Whether a duty exists is a question of law to be resolved by the court.”
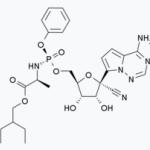
On Wednesday April 29th the Dow Jones Industrial Average rose 532 points on news that Gilead's remdesivir demonstrated a “clear-cut positive effect" in treating COVID.
Pricing a new drug is not an easy task, Gilead who is producing remdesivir is no stranger to pricing controversy, the release of Solvaldi, their drug to cure Hepatitis C, had a list price of $84,000 for a full treatment course.
Six weeks of endless speculation, guessing, second-guessing, ups, and downs about whether the world would have its first effective coronavirus drug has been exhausting. I see the damn molecule in my sleep.
If there is a single company that tops the "no good deed goes unpunished" contest I would pick Gilead Sciences. By a mile.
Having spent a decade (of pure futility) in hepatitis C (HCV) research in my former career, I have spent a fair amount of time since then writing about the astounding progress made over a 25-year period.