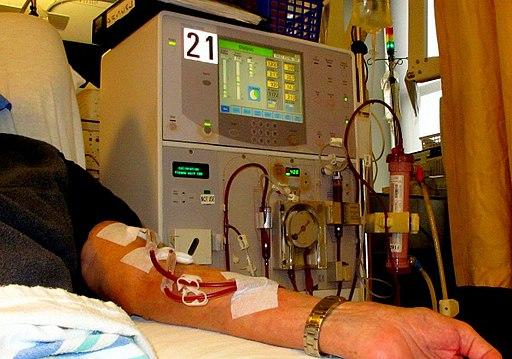
California has a proposition on the state-wide ballot that will limit the revenues of dialysis centers to 115% of the cost for “direct patient care services” and “health care quality improvement costs.” [1] It has attracted national attention given more than $110 million in lobbying expenditures by the two largest dialysis businesses in the state. Will this attempt to get the public behind price, or in this case, revenue fixing work?
Background
Patients who develop chronic renal failure are unable to detoxify waste and fluids, without dialysis, a three to four hour, three times a week, cleaning of their bloodstream they die. Some can get a kidney transplant and get off this endless cycle but for 80,000 Californians that has not happened and they receive most of their dialysis at freestanding chronic dialysis clinics (CDC). California estimates that revenues from these services amount to $3 billion annually.
Medicare is the primary payer, covering its normal 65 and over beneficiaries and through the End Stage Renal Disease program [2] provides the same care and coverage for those under 65 after they have received dialysis for more than 30 months. In that “coordination period,” dialysis costs are borne by Medicaid, in the state of California called Medi-Cal, and by health coverage through work or other organizations, e.g., commercial insurance. While the payments to dialysis centers from Medicare and Medi-Cal are “relatively close to the average costs” for providing dialysis; the payment from commercial insurance is negotiated and are often multiples of Medicare payments. This proposal seeks to bring commercial insurance payments down and thereby reduce health care costs and premiums.
Proposal
Any revenue great than 115% of payments for direct patient and quality improvement would have to be rebated to the insurance companies, along with accrued interest; and the dialysis clinics penalized an additional 5% of those rebates payable to the state. As with all ballot propositions, there is a small print explanation of economic effects - something that is rarely read by voters.
Fiscal Analysis
“Paying rebates in the amount of the excess would significantly reduce the revenues of CDC (chronic dialysis clinics) owner/operators… this means the CDCs would be less profitable or could even be unprofitable. … These future actions [CDCs’ response to passage of the proposition and the subsequent actions of the state regulators and Courts] are difficult to predict.”
That’s reassuring.
Among the uncertainties making a fiscal windfall or clinical disaster are:
- What is direct patient care costs? For every additional dollar spent on patient care, there is a $1.15 reduction closing the gap between revenue and the revenue cap. For example, if the wages for patient-care staff was increased. This explains why the Service Employees International Union, the SEIU, has put $17 million into lobbying for the proposition and was the proposition’s authors.
- Centers might reduce their non-direct costs, like administrative overhead or scale back operations by reducing hours of operation, or reducing the number of centers. That would make them more productive. Scaling back operations will also result in less convenience and more travel for patients, a particularly odious form of rationing – “rationing by hassling.” Or they merely could stop offering services; no business can run at a loss forever.
The bill only applies to commercial insurance, but the state and many local municipalities often outsource their healthcare coverage to private carriers and might qualify for rebates. There is no regulation regarding what the insurance companies do with their refunds; so they might pass those savings along to the employees who actually pay the premiums, or not. So the effect on tax-payer supported healthcare for state employees is unknown. The impact on Medi-Cal is also uncertain.
The report concludes that the fiscal impact on state and local government finances will either be “net positive” or “net negative.” There will be a sure loser, a new Big, Big Dialysis.
I understand the massive lobbying efforts by both the two largest dialysis companies (DaVita and Fresenius) a $100 million is a small amount if it prevents a billion dollar loss. I understand why the SEIU has put $17 million into the effort. But who is speaking for the patients? So far only the California Medical Association and the American Nurses Association. How will this improve the quality of care for patients on dialysis? Will paying SEIU workers more, result in them being more caring or empathetic? Will paying higher wages result in more SEIU personnel hired to care for these patients? What possible efficiencies will dialysis companies introduce? Do you believe they will increase the workload or reduce the number of administrators, or will consolidation of facilities and running them 24/7 be their favored approach?
Do we need to control health care cost? Yes. Has price regulation ever resulted in saving over shortages? I am not aware of any example. One last question, both of these dialysis companies are global in scope, do you think they might raise their charges in other states to compensate for any losses in California, robbing Peter to pay Paul?
[1] Another way of phrasing this is a cap on profits at 15% of costs.
[2] The End Stage Renal Disease (ESRD) Program was authored by Senator Ted Kennedy and covers about 90% of patients with ESRD requiring dialysis. It is the only disease-specific benefit available through Medicare irrespective of age; in some ways, you might think of it as Medicare for All for just one disease. 1% of Medicare patients have ESRD, and they utilize 7% of Medicare’s budget.
Source: Proposition 8 Authorizes State Regulation of Kidney Dialysis Clinics. Limits Charges for Patient Care. Initiative Statute.