To ACSH advisor Dr. David Shlaes, the outbreak of the Wuhan coronavirus in a nursing facility is scary but not surprising. He's appalled by the poor care of the elderly in our long-term care facilities, most of which are for-profit organizations.

The Achilles Heel of our healthcare system is our long-term care facilities. I don’t care if we’re talking about flu, coronavirus or resistant bacterial or fungal infections. We take our most vulnerable citizens and place them in understaffed facilities with under-trained staff and where conditions may be crowded. What are we thinking?
The recent outbreak of coronavirus infection in a nursing home in Washington is not surprising – but it is scary.
Is this news? Of course not. The CDC has examined this question previously and provides a great deal of astounding data that you can find here. The figures below all come from the US CDC.
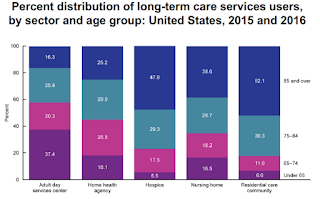
Most residents of nursing homes and residential communities are over 75 years of age with a large number being over age 80.
Almost 70% of nursing homes and over 80% of residential care communities are for-profit organizations often part of national chains.
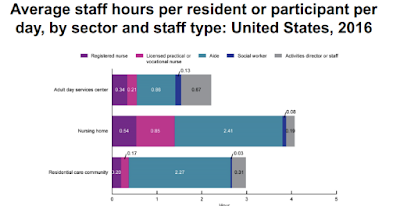
The vast majority of healthcare workers in these facilities are Aides. Each resident can expect to have 3-4 hours of care per day – mostly from Aides. Aides, mostly, are required to have a minimum of 75 hours of classroom and practical training – not much. (By contrast, a registered nurse must have either an associate degree or a bachelor degree). Of course, during off-hours like evenings, nights and weekends, staffing is often minimal.
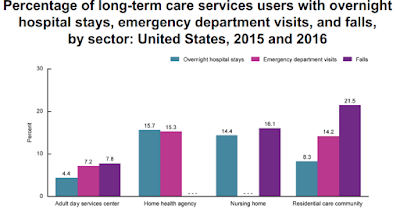
Falls and hospital admissions are frequent.
Outbreaks of resistant infections have been documented frequently in our long term care facilities.
My mother spent the last ten years of her life (she lived to age 97) in several assisted living facilities. They were all privately owned and one was non-profit. But the non-profit facility distributed the wrong flu vaccine one year (not the high dose recommended for those over age 65).
Is this something we should let the markets handle (as we mainly do now) or should we regulate these facilities more stringently?
# Reprinted with permission from Dr. Shlaes' blog Antibiotics - The Perfect Storm. The original posting can be found here.
Category