To everything, there is a season
A time to be born, a time to die
A time to plant, a time to reap
A time to kill, a time to heal
A time to laugh, a time to weep
elderly
DAY 1 Was it just last winter when we left the New Year's Eve party in a snit because we couldn't dance to the music selected by the "younger group" living in our retirement community?
My generation, the Boomers, are not shy in expressing their opinions, but what about those of us, slightly older, the generation of the Korean war, so “inconsequential” that their name is “The Silent Generation,” lost between the Greatest Gene
I've been in science communication for over 8 years. If there's only one thing I learned, it's this: People don't respond to facts.
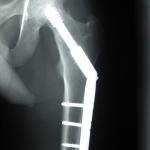
Fractures in the elderly result in significant dysfunction, with many not recovering their full function, with up to 25% requiring permanent institutional care and an eightfold increase in mortality within three months of a hip fracture.
The most common form of dementia, Alzheimer’s Disease (AD), currently afflicts 5.5 million adults in the United States and is estimated by 2050 to impact 13.8 million (age 65 or older).
Why is this happening?
China, with one of the largest – if not the largest – elderly population on Earth, has a strong incentive to learn how to support or improve cognitive function for its older citizens.