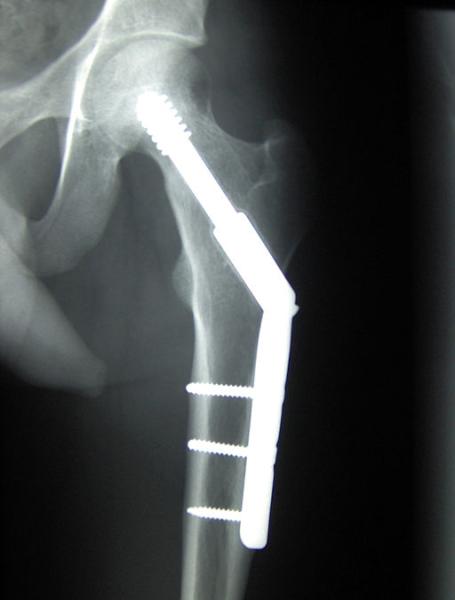
Fractures in the elderly result in significant dysfunction, with many not recovering their full function, with up to 25% requiring permanent institutional care and an eightfold increase in mortality within three months of a hip fracture. Treatment has been directed at strengthening bone with Vitamin D and calcium as well as assistance in ambulation and balance. A new paper brings an engineering perspective to the issue comparing structure fatigue to bone “fatigue;” suggesting that upwards to 25% of these fractures represent bone fragility or what I term orthopedic frailty.
Besides providing an interior structure for our bodies, so that we are not amorphous masses, bone serves to anchor our muscles and form levers with our joints, that help us stand and walk. Beneath the surface, bone remains an active tissue, responding to the physical stresses our upright posture and ambulation create, remodeling to strengthen areas of stress with more bone.
Osteocytes, comprising 90% of our bone’s cells, translate those mechanical stresses, communicating with osteoclasts, which reabsorbs bone and osteoblasts that create bone to create an orchestrated response. Specialized passageways, called canaliculi, tunnel through the bone to allow the osteocytes to communicate and provide oxygen and nutrition to all the bone’s cells. Bone’s remodeling has three phases; bone is initially reabsorbed before a final stage when new bone creation is complete. The time between full reabsorption and bone creation, the second phase, is a time when the bone in that small area is considerably weakened. Bone remodeling is known to slow with aging, and there can be increasing asynchrony between the forces removing and building bone so that over time there is less bone, decreased bone density.
Fractures
Traditional thinking about traumatic fractures suggests that a sudden force impacts the bone exceeding its strength resulting in a fracture; for the elderly that frequently is the impact of falling. The decreasing bone density of aging is thought to reduce the force necessary to cause the fracture so all of our efforts at diagnosis have been directed at determining bone density and treating patients with Vitamin D, calcium and in some cases a medication (Biphosphonates). But up to 50% of fractures in the elderly occur in the presence of normal bone density prompting a rethinking of the mechanism of fracture.
Bone derives its strength through a binding together of the small-scale strengths of collagen, our primary structural protein, into larger and more significant structural components. Perhaps the easiest way to visualize what is happening is to consider the bridge cables. Those cables consist of a single wire entwined with other wires creating a small cable, in turn, wrapped with other small cables forming larger cables. A “chain is as strong as its weakest link” applies to the bone and tiny weakness in collagen results in overall loss of bone’s strength.
The stress on bones comes and goes, think of the forces acting on your legs as your weight moves from left to right as we walk. Those stresses deform the bone, ever so slightly; the bone's collagen is ground zero for those changes and accommodates by sliding over one another dispelling the force over a larger area. Collagen is also cross-linked, tethered to one another resisting and limiting that sliding. As we age, we form more and more crosslinks, reducing collagen’s movement in general, making our bones more brittle. The cross-linking can be measured with a metabolic marker, advanced glycation end products or AGE.
Bone Fatigue
Since we walk and stand upright most of the time, the same areas are repeatedly stressed. Drawing from the world of mechanical engineering, repetitive, cyclic stress results in a decrease in the material's resistance to changing shape, called fatigue. Anyone who has bent a piece of metal or plastic back and forth to break it is familiar with “cyclic loading” and mechanical failure due to “fatigue” – the cause of 80% of catastrophic failures of bridges, axles, airframes. The paper's contribution is to introduce the biomechanical concept of bone fatigue as a source of fractures. In fact, they suggest that upwards to 25% of fractures in the elderly are not due to falls, but cause the fall as the fatigued bone “snaps.”
Microdamage, small nanometer size cracks, develop in areas of repetitive stress, osteocytes signal to initiate repair, through reabsorption and replacement. In healthy, younger bone, damage occurs more slowly and the phase when the bone is weakest, after reabsorption and before the new bone is wholly laid down is short. In aging, cellular repair slows prolonging that period of greatest weakness. When coupled with age-related increased bone stress from changes in our muscles and joints those tiny cracks get larger. The breaks disrupt the canaliculi, the passageways for oxygen, nutrition and signaling the need to begin repair to the cells resulting in more cells dying and prolonged loss of bone strength. We measure this increasing dysfunction of cellular activity as loss of cells, declining bone density, but the real problem may be the loss of bone quality. Quality in this case meaning the ability to gently yield in the face of stress and resist fracture. Bone quality may account for part of the ten-fold increase in fractures in the elderly that is independent of bone density. Orthopedic fragility, frailty, is a high rate of fatigue-damage formation exceeding the rate of bone remodeling and repair.
Diagnostic and therapeutic challenges.
These fatigue induced fractures are frequently termed “stress fractures.” There is swelling of the bone’s surface and marrow, and subtle and tiny linear fractures; findings that normal X-rays studies are too insensitive to detect. The expense and radiation associated with MRI and CT imaging to screen for fractures are too great. More importantly, the patient’s complaints of increasing aches and pains in these bones that would prompt such studies are masked by other problems of aging, attributed to “arthritis” or getting old rather than formation of stress fractures. Measurement of collagen crosslinking, by those advanced glycation end products, is a future consideration.
Vitamin D has been shown to have a role in osteocyte survival, so recommendations for adequate intake of both Vitamin D and calcium seem prudent. We also know that the more active elderly experience less of these fractures; although too much of a good thing and exercise may increase the cyclic loading and enhance damage. So it may be useful to cushion ourselves when engaging in these activities, for example, wearing appropriate footwear that cushions the stress of walking and running. It might also be helpful if we can get help in identifying exercise that optimizes activity and reduces load, for example, swimming or other form of water aerobics.
Source: Fatigue as the missing link between bone fragility and fracture Nature Biomedical Engineering DOI 10.10138/s41551-017-0183-9