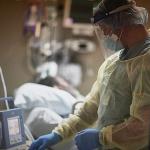
End-of-life care is an uncomfortable topic for many if not all of us. Many individuals express a preference for dying in their own homes, providing a sense of control, privacy, and the ability to be surrounded by family and friends.
end-of-life care
During the years of my medical career, when I treated patients (always in hospitals), I was one of those rushed doctors who focused on efficiently formulating and implementing diagnostic and treatment plans rather than on the patient’s emotional n
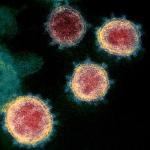
Perhaps other than virologists, few people would have predicted that a tiny microbe would dominate global headlines for several months in 2020. It goes without saying that the coronavirus has kept us quite busy.
End-of-life hospitalizations can, for obvious reasons, be brutal for the individual and his or her loved ones.
Have you started your Christmas and/or Holiday shopping? If you're like us, you're putting it off to the last minute because you're too busy with other things. Here at ACSH, we've been busy telling the world about science.
With right-to-die legislation in its fledgling stages in the United States, the bioethics surrounding assisted suicide are in play as they haven’t been in the past.
Early on January 27, 2018, The Most Interesting Man in the World passed away at the age of 91.
Unlike our ancestors, who encountered it often, members of our modern society seem strangely detached from death. Many people have never even seen a dead body.
A recent report in JAMA by a large study group shows mixed results when it comes to end-of-life care