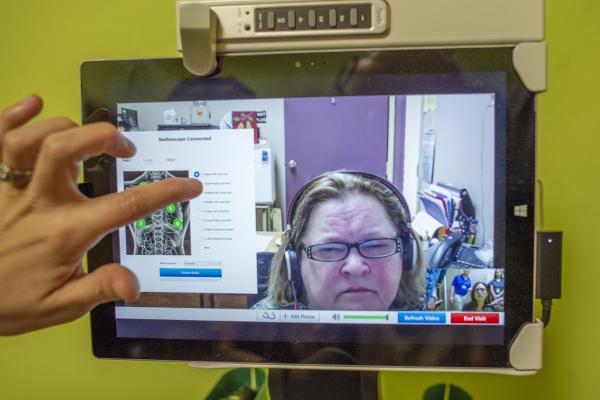
End-of-life hospitalizations can, for obvious reasons, be brutal for the individual and his or her loved ones. By nature of the ominous diagnosis itself and the highly variable set of circumstances unexpected or otherwise that set the stage for the ensuing death, the chain reaction of events by definition test all aspects of our humanity. Now, imagine a man who is challenged to breathe and has difficulty hearing learning the news things have gotten quite grim by a doctor via a wheeled in video-link screen device fashioned atop a robot-like mobile kiosk placed at the foot of his bed. Picture his granddaughter alone at his bedside who is constantly repeating the doctor’s words because the patient cannot accurately understand them due to the loudness of the machines and his various impairments. And, the suffering is unnecessarily compounded.
Such is the story of a man who passed away last week after an intensive care admission to a Kaiser Permanente medical facility in California. His family is alerting media outlets of their experience so no one else should ever have to endure what they did (see BBC News, Fox News for full video of exchange). As per the granddaughter, “the medical staff told her the robot is "policy" and "what we do now."”
The family doesn't deny that they were aware of how sick their loved one was, the granddaughter said,
"Devastated. I was going to lose my grandfather," said Wilharm. "We knew that this was coming and that he was very sick. But I don't think somebody should get the news delivered that way. It should have been a human being come in."
Her mother conveyed
"If you're coming to tell us normal news, that's fine, but if you're coming to tell us there's no lung left and we want to put you on a morphine drip until you die, it should be done by a human being and not a machine," Catherine Quintana told USA Today."
"We offer our sincere condolences," said Kaiser Permanente Senior Vice-President Michelle Gaskill-Hames. "We use video technology as an appropriate enhancement to the care team, and a way to bring additional consultative expertise to the bedside. Gaskill-Hames added the machine visit was a follow-up to earlier physician visits. She says it did not replace previous conversations with patients and family members. “The use of the term ‘robot’ is inaccurate and inappropriate,” she exclaimed. “This secure video technology is a live conversation with a physician using tele-video technology, and always with a nurse or other physician in the room to explain the purpose and function of the technology. It does not, and did not, replace ongoing in-person evaluations and conversations with a patient and family members.”
They go on to say
"The evening video tele-visit was a follow-up to earlier physician visits," she added. "It did not replace previous conversations with patient and family members and was not used in the delivery of the initial diagnosis.... "That said, we don't support or encourage the use of technology to replace the personal interactions between our patients and their care teams - we understand how important this is for all concerned, and regret that we fell short of the family's expectations.”
If you watch the video of the exchange, then you will discover there is discussion about emphasizing comfort care and the use of morphine, its benefits and risks. Morphine at this stage in particular with someone with such respiratory compromise can among other things slow breathing further - so it is a delicate dance to control pain while not imperiling a patient. The man on the video screen conveys he doesn’t anticipate the patient will be going home. As you watch, you hear the granddaughter while tearful with apparent anguish reiterate what he says, abbreviate his words and express the need for her mother and grandmother to participate in this conversation.
It is heartbreaking.
Such dialogues are occurring daily in this country under similar circumstances, so they are not unique. But, the fact this video element was added to this one will forever haunt this family. Had the identical scenario occurred in person, the doctor could get closer to the patient to adapt and meet him where he was clinically. His physical presence alone would have added peace.
There are a lot of situations where such technology has enhanced care. Consider when someone is in a remote area or one with a lack of desired specialists. When the option is no medical personnel or this, then the stakes change. If the option is a video-link call versus an audio only one for a routine illness, then there can be merit to that under the appropriate setting. The technology can be used to allow family members from elsewhere in the country to call in by live video so they can be "present" when a physician rounds on their loved one.
But, the informed consent of the patient and his family should always be taken into account especially at the end of life. These discussions are precious and significantly factor into everyone's well-being. Tech use should be tailored accordingly with well-defined parameters that are not one-size-fits-all. It is apparent from this instance that whatever policy (or lack of effective communication of video use in hospitalized patients) was in place did fall demonstrably short for this family and warrants immediate revisiting. Despite the many wondrous advances happening in the digital medical realm, we must always ask ourselves how we can preserve and protect “care” in healthcare.
Technology in medicine should serve to facilitate humanity, not replace or undermine it.