Let's call progress against cancer a mixed bag. Until 20 years ago, chemotherapy drugs — poisons that kill or stop the division of cells— have been the mainstay of cancer treatment. These cytotoxic drugs, many of which are more than 50 years old, work on the principal that cancer cells divide more rapidly (1). So that anything that poisoned all cells would disproportionately affect cancer cells. It works-- sort of.
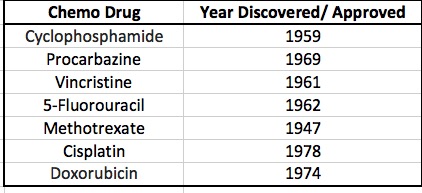
Some commonly used cytotoxic chemotherapy drugs and the year they were discovered or approved. Progress?
Two of the many flaws in the use of cytotoxic drugs are systemic toxicity (often brutal side effects), and resistance (mutation of some of the cancerous cells, which withstand chemotherapy and continue to grow). The advent of targeted therapies, ushered in by Rituxin in 1997 and Gleevec in 2001, was seen as the holy grail of cancer: drugs that would specifically interrupt pathways that are unique to cancer cells while sparing others. While there have been some groundbreaking successes with targeted therapy, it has not lived up to all the hype:
- The targeted therapies have their own set of side effects.
- They are often combined with cytotoxic drugs, rather than replacing them. This can make the side effects worse.
- When a target of cell division is blocked, cancer cells have multiple redundant pathways, which can take over, thus short-circuiting the targeted therapy.
- Efficacy against cancers that are difficult to treat is often modest. Some newly approved cancer drugs extend life by months, not years.
But, a novel mechanism for specifically targeting cancer cells has been reported in the January 24th issue of Cell Reports. Scientists at the Washington University School of Medicine in St. Louis have uncovered a weak spot in cancer cells that is not present in normal cells—the need for arginine, one of the 20 amino acids that make up human proteins.
Brian A. Van Tine, MD, PhD, an associate professor of medicine and colleagues found that cancer cells, especially those from sarcomas (2), have a critical defect—they rely on arginine in the blood for fuel. Normal cells make their own arginine, but 90 percent of sarcoma cancer cells cannot (3). When deprived of arginine, these cells starve, and begin a process called autophagy (self-eating). This defect in cancer cell metabolism raises the possibility of a drug that would kill only cancer cells by selectively depleting the supply of arginine in the blood. But, this is not enough.
An experimental drug called ADI-PEG20, which depletes arginine in the blood has failed in several clinical trials. This is because cancer cells are rather fond of living, and have developed a way to survive in the absence of arginine. When its supply is shut off, the cells slow down for a while, but then turn on a salvage pathway, which instead uses glutamine, another amino acid. In fact, when sarcoma cells were exposed to ADI-PEG20, they actually began to make more glutamine (upregulation).
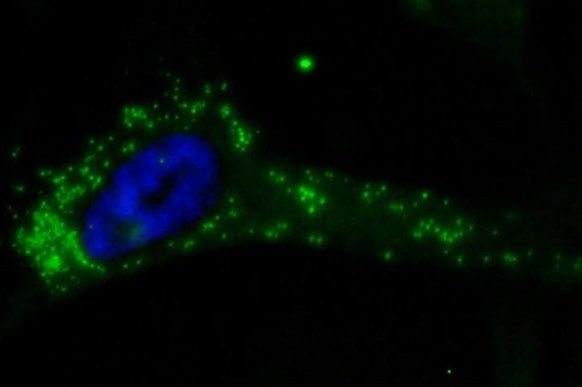
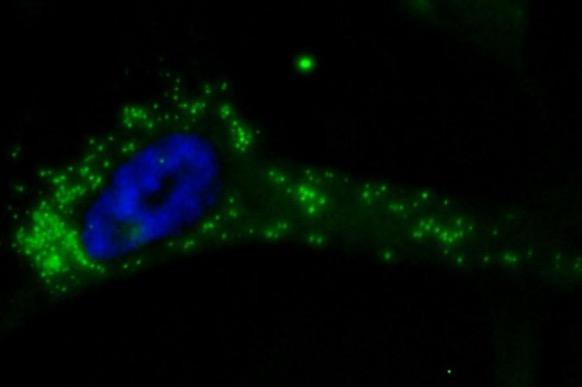
A sarcoma cell in the starved of arginine. The blue is the nucleus of the cell. The green indicates areas where the cell has started to feed on itself. Image: Jeff Kremer, Washington University Medical School.
Van Tine's group decided that a double whammy was necessary—shutting off the supply of both amino acids (4). When a drug that inhibits glutamine biosynthesis was added, the cells couldn't handle both and began feeding on themselves.
One of the primary challenges in cancer treatment has always been selectivity. It is "easy" to kill bacteria or viruses because they replicate by very different mechanisms than normal human cells. Cancer cells, for the most part, do not. A strategy that effectively distinguishes between cancerous and non-cancerous cells would represent an enormous advance in the treatment of cancer. Clinical trials are being planned for patients with sarcomas.
We should keep our fingers crossed. A drug combination that kills cancer cells while sparing healthy cells is just what the doctor ordered.
Notes:
(1) Cells in the stomach and scalp divide especially quickly, which is why vomiting and baldness are common side effects of cytotoxic agents.
(2) Sarcomas, which are cancers of fat, muscle, and connective tissues do not respond well to chemotherapy.
(3) Sarcoma cells lack the enzyme argininosuccinate synthetase, which is responsible for the biosynthesis of arginine. This is why they depend on arginine in the blood to replicate.
(4) The amino acid serine can also act as a backup. Blocking the production of serine also resulted in cell death.
Original source: Van Tine, A., Cell Reports 18, 991–1004, January 24, 2017
SaveSave



