The U.S. Preventive Services Task Force (USPSTF) recently released a 2017 draft recommendation statement on screening for prostate cancer which is based on systematic evidence review and assessment— updated from their prior 2012 version. As indicated by the authors’ viewpoint published in JAMA, the goal of this release is to raise awareness of newly acquired data on the topic while inviting review and commentary before the report is officially finalized. (1)
Because there was concern that universal PSA (aka prostate-specific antigen, a blood test) population screening often times leads to unnecessary treatment which in itself carries risks, determining criteria for those at higher likelihood of developing disease and how to stratify or prioritize testing is at the forefront of decision-making for prostate cancer screening, prevention, disease monitoring and cure.
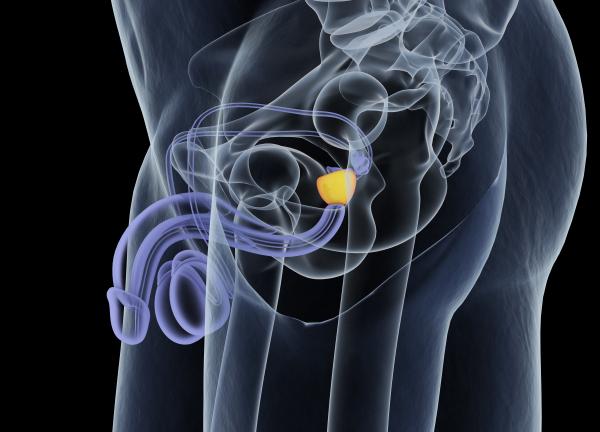
First, let’s discuss some basics before delving further into the latest revelations in prostate cancer screening, diagnosis and the therapies available. What is your prostate and what is its purpose? It is a tiny gland that rests in-between the bladder and rectum of men. It encompasses a portion of the tube (aka urethra) that transmits urine from its reservoir of the bladder down through the penis. Additionally, it plays a role in secreting some components of semen. This sperm-filled fluid makes up your ejaculate.
As a typical part of aging, the size of the prostate tends to grow. It is always useful to think of real estate when considering the impact of this often natural process, especially when extreme examples take place. Because the area is replete with nerves and anatomy essential to normal urination and sexual function, damage to it by treatment radiation, trauma, surgery or mass effect from excessive enlargement of the gland or malignant spread can dramatically impair a man’s quality of life.
It is not rare for a man with prostate cancer to be entirely asymptomatic. Hence, why it is often considered a silent disease and rampant PSA testing in conjunction with digital rectal examination (DRE) was once deemed standard protocol for all men. DRE requires a physician to place his gloved finger entering the anus inside the rectum to feel for any ridges or nodules of the gland. Because accessing the entire prostate is not possible by this method, the blood test described and other imaging studies complement the process so as not to miss a cancer diagnosis.
Some men will have symptoms of urinary dribbling, for example, that necessitates exploration and intervention. Just because you have them does not mean that you have prostate cancer, but it is certainly important for you to be properly evaluated to be sure. Like with all cancers, the earlier it is detected the greater your chance of less invasive treatment and improved survival. The gland itself can get infected, so antibiotics do the trick in that scenario. Or, benign enlargement can be another culprit which can be successfully managed and monitored.
The American Cancer Society declares besides skin cancer, prostate cancer reflects the most common cancer in American men. They estimate 2017 will bring roughly 161,360 new cases and 26,730 deaths. Behind colorectal and lung cancer, it is listed as the third leading cause of cancer death in men. About 1 in 7 will receive the diagnosis in his lifetime, but being older is when it usually appears with the average age of diagnosis being 66 occurring in men 65 or older in 6 out of 10 cases. Appearing before age 40 is rare. (2)
There is significant variability in the aggressiveness of the illness. Those with the low-risk type—who are traditionally older— now appear to fare quite well with reduced harm from immediate surgery or radiation by following the latest trend of “active surveillance.” This watchful waiting approach involves close monitoring with frequent PSA testing and biopsy before proceeding to invasive treatments. This would be for selected men excluding those with more aggressive forms and at higher risk.
Some conclusions of the USPSTF 2017 recommendations include there may be a small net benefit to screening in men ages 55 to 69 years where the risk to benefit ratio is pretty close suggesting the decision to initiate screening be an individual one. Also among this new research is the finding that 3 men per 1000 offered screening may avoid metastatic disease. (3)
Q&A
To tease out the state of prostate cancer from screening to cure along with last week’s USPSTF draft publication, I have enlisted the help of the Chairman of Urology, Chief of Robotic Surgery at Lenox Hill Hospital, Dr. David Samadi. Dr. Samadi is a board-certified urologic oncologist trained in open traditional and laparoscopic surgery, world-renowned for his expertise in robotic prostate surgery:
How would you summarize the latest prostate cancer screening draft recommendations by the USPSTF compared to their prior effort in 2012? Agree or disagree?
The most significant change from the 2012 USPSTF recommendations is their upgrading prostate cancer screening from a Grade D (more harm to screen than treat) to a Grade C classification. Over the past 5 years, the data showed greater tumor migration in younger men with more aggressive cancer. In those scenarios especially, not screening would do men a tremendous disservice as they would present with metastatic disease. When a cancer is contained, we can not only prolong life but preserve its quality. Once it spreads, it is much more challenging.
Also, they realize care needs to be individualized as conversations must be meaningfully had with those with a strong family history and African-American males in particular. These groups have a higher likelihood of developing prostate cancer. In general, the risks can outperform the benefits of routinely screening with the PSA test between ages 55-69 as the number of biopsies increases, anxiety and so forth. About 70% of those with low risk cancer will die from something else.
The American Urological Association (AUA) and ACS (American Cancer Society) have been working together to bring sense to this since the idea of no screening till age 55 was not a good one. Prostate cancer of low, moderate and aggressive risk in young men could be missed and if not screened then they will have metastases and die from it. In all guidelines, they talk of death and no one was talking about rate of metastases or quality of life.
Because of the prior recommendations, we are seeing a higher rate of metastases which is not what we were seeing. PSA though nonspecific has reduced number of metastases and number of deaths about 30-40%. There is an art to dealing with the PSA and not every elevated PSA warrants biopsy. The physician looks at the trend, does it double in time, family history and is there a nodule or not on physical exam etc. The information is put together like detective work. What is rate at 40-55, 50-55? What is the health and degree of activity of the man over 70 or any age? People are living longer with stents and other issues, so we need to adjust and look at many different factors. So the Grade D to C is a big step forward. Patients can ask doctors and bring it to doctors.
We have a long way to go before PSA and mammogram are on par. Men need to wake up and be more aware for until we come up with a specific test, PSA is the best we have. We are getting better in diagnostic tools, better genetic tools and getting better overall. Ultrasound was more crude with high false negatives, and now we have better imaging to discern who is more in need of intervention. We use 3Tesla MRI or MRI where the ultrasound pictures fuse with MRI images for more targeted biopsies almost like GPS for biopsy as opposed to randomly shooting in the dark and missing the cancer.
What causes prostate cancer? Please identify modifiable risks.
Age is a main risk factor. The older you get, the higher the risk. Over age 70, the risk drastically increases. So, why are we not being aggressive with those guys? Because cardiovascular diseases are going to get them more than prostate cancer, the guidelines are set for the public and not for a specific person. That’s why care needs to be individualized. The plan might be more aggressive if a 70 year old man is overall healthy, his father lived to 95 and he takes care of himself as opposed to one who is 55 with high blood pressure, morbid obesity, smokes and due to the co-morbidities would not fare as well from surgery.
Race carries much risk. The incidence of prostate cancer is 3:1 for African Americans over Caucasians. Environment is also a factor with a diet rich in high fatty foods and low fiber being culprits. Genetics plays a role, so positive family history is influential.
Who is at greatest risk of aggressive or metastatic prostate cancer?
The message should be there are people behind guidelines and it is the art of medicine to personalize. Young men with a prostate cancer diagnosis tend to have it be more aggressive in nature. Your Gleason score determines your risk. It is on a 2-10 scale with 2-6 being low, 7 moderate, and the 8-10 range being an aggressive prostate cancer. Everything is looked at to make a pathologic classification to tell a patient how aggressive and then it is delineated even beyond that using the percentage of core, number of core, what score, volume of cancer, age, ethnicity, family history etc. to make a decision on how to proceed.
When caught early and contained, men do very well and lives are saved. Despite the guidelines, I recommend a baseline PSA at age 40. If your PSA is over 1.5, then see urology immediately because your risk of prostate cancer is high (see this study). If wait until age 55, some of these men will go without being noticed and wake up being among the near 27,000 men who die per year like breast cancer.
Prostate cancer screening has been wishy washy because our test, the PSA, hasn’t been specific. We should look at the trend and keep under surveillance as some men do have very aggressive cancers.
How is a man diagnosed with prostate cancer? Since it is often considered a silent disease in that symptoms can be absent, please walk through the steps a man endures to arrive at diagnosis— including the risks and limitations of biopsies, for example.
He should have a baseline PSA at age 40. If okay, then again at 45 or 50 when he starts to take annually. If there is a strong family history and/or he is African-American, he should talk to his doctor. Any time a PSA is done he should have a DRE. In 15% of the time, the doctor will feel firmness or a nodule that would be missed if didn’t do the DRE and the patient will see urology.
If the PSA is elevated, the first step might be to treat with antibiotics for 7-10 days to deal with any possible infection and inflammation instead of an immediate biopsy. Then, repeat the PSA and do an MRI. If the MRI shows no lesions and the PSA goes down, then the patient may not need a biopsy. Prostatitis and the easy things should be first ruled out before jumping to a biopsy.
Much conflicting information has surrounded the PSA blood test as the paradigm shifting of USPSTF recommendations has led to some confusion. Please clarify its role. How do we balance the hazards of over treatment with prevention of metastatic disease?
No matter what you do with any kind of screening you tend to over treat to some extent. The danger of over treatment is the change of the man’s quality of life. The way to fight that is to have their care managed and taken over by experts which improves their quality of life. Clearly, a surgeon who performs 30 vs 400 cases will not have the best outcomes. So, getting 2 and 3 opinions with ever improving technology is a way to go where even if over treated, the quality of life isn’t affected—so not much harm is done.
For certain patients, aggressive treatment and diagnosis can save a life. Prostate cancer is known as a silent killer that by the time you have symptoms of back pain or obstructed urination it is too late. If was screened years ago, then would not have required radiation and chemotherapy.
Sometimes it comes across that all surgeons want to do surgery. But, surgery is a good first modality. It will give you certain things that other things won’t, like accurate staging. You might find 30-40% more cancer and a more aggressive cancer than previously thought from imaging or biopsy alone. PSA after surgery goes to undetectable levels and should remain there. So it is very easy to follow a patient because the PSA has to be and stay zero.
In radiation, you are only treating what a random biopsy showed and the PSA fluctuates making it difficult to interpret in the long-term. If there is cancer after initial surgery, you still can get radiation or chemotherapy if it comes back. Surgery is still a viable option and low dose radiation has fewer side effects. But, the other way around, surgery after radiation is practically impossible since the tissue adheres to the rectum and the prostate becomes like cement. Radiation carries the risk of secondary cancers (e.g. bladder, rectal).
Though all interventions have incontinence and impotence risks, in the hands of expert surgeons better outcomes result. There are many throughout the country.
How would you define “active surveillance” and the patient who qualifies for it?
Those who have a lower risk cancer might be eligible for active surveillance. And, it is just that—emphasis on “active.” They might have had a couple biopsies, and with their co-morbidities not be good candidates for surgery. Regardless of the circumstance, it requires a very compliant patent with follow-ups every 3 months that includes an exam, frequent PSAs and biopsy once a year or every other year.
It is a real active surveillance which at times can be very anxiety-inducing as they worry about walking around with cancer. They are being monitored to see if the biopsy changes and there is more cancer. Rarely at age 40 is this a long-term plan for them, given lifestyle considerations among others. At this age, when the surgical case is easy and curable it can make more sense to do it since it becomes much harder 3-4 years down the line when you might have to jeopardize nerves and continence.
Please discuss the prostate cancer surgical treatment options and risks of incontinence, impotence and complications.
The risks are rare with biopsy which is often the first step (takes about 15 minutes). This should be performed by a urologist. There can be bleeding in the semen or blood in the urine which is typically transient with a small percentage (about 2%) getting an infection.
Open surgery is the more conventional, traditional approach that requires a large incision from the belly button down to the pubic region. It often requires transfusions due to lots of bleeding and protracted recoveries for patients. The number of these surgeries have gone down drastically for these and other reasons. Those who advocated for open surgery over newer robotic-type surgery kept talking about the ability to retain tactile feedback when there was no visualization due to bleeding into the operative field. When this occurs it makes the surgeon almost blind and you need to use fingers to find any extension of cancer or problems. Those proponents would argue you can’t feel with robotic techniques, but that argument doesn't cut it anymore.
With robotic surgery, there is no blood in the field as CO2 gas tamponades. Eyes are more accurate than tips of fingers. There is no tremor. Operative time and recovery are much quicker increasing safety and benefit for the patient. With volume expertise comes better outcomes. So, in the hands of an expert surgeon, issues with continence are less and sexual function can raise to 78% at one year post-surgery. Depending on a surgeon’s series, range of sexual function can raise between 40% to 80% with rate of continence 85-95%. Oral medicines, vacuum devices and other options can be used to achieve more quality erections with every 3 months that passes showing better and and better improvement.
Younger guys tend to bounce back more effectively with urination and erectile function if the nerves were saved and there was no cancer invasion (see this study). Life comes first, so with surgery it is cancer sparing first and nerve sparing second with every effort made to contain nerves.
Obviously you prefer robotic, but why? Are you biased?
No, I am not biased and I will tell you why. I was an open surgeon first from my training at Memorial Sloan Kettering. Then, I was among the first surgeons to go for training in France and went on to do laparoscopic and robotic surgery. Laparoscopic surgery is ideal for kidney cancer, but there is no real role any more for prostate cancer due to tremor at the probe tip and so on… Robotic provides a 3D view without tremor.
I do a little more advanced robotic surgery whereas most surgeons try to come from the outside in, I go from the inside out. Imagine peeling an orange with the skin being the nerves and the orange itself being the prostate. Most attempt first to mobilize and peel the nerves to the side. By touching them, you are at higher risk of damaging them. I come in from the top and go around the prostate leaving the nerves where they are. So, it is more moving the prostate away from the nerves instead of the nerves from the prostate.
The bottom line is if the choice is between an experienced open surgeon with a rookie robotic one, then go with the open. An excellent open can do a great job. But, if the choice is between both super experienced open or robotic, then the robotic technique involves less blood loss, less incision and other pain and is better for the patient.
What are the right answers to questions patients should ask before picking a urologic oncologist surgeon. For example, how many cases performed per year is considered highly experienced?
How many cases do they perform per year? Over 100 prostate surgeries per year is good with the more being the merrier. The more you practice your tennis serve, the better you will be. The more robotic surgeries you do, the more qualified you become. What kind of continence and sexual function do you see after surgery? Who performs the operation? Is the surgeon involved in the case or not? Is he involved in further treatment and follow-up? You want a surgeon who will spend the entire journey with you. A urologic oncologist surgeon who follows you for life— that demonstrates a person who takes pride in what they do. This is the optimal person to follow you since they have examined you, understand the nuances of the changes in your physical exam and will treat you as their own patient. A multidisciplinary team with a medical oncologist can be invaluable.
You want a surgeon who reviews his cases by video and medical record, much like a football player who watches his plays so as to perfect and modify his technique. It is so crucial to warn the public that just because someone says they are an expert in robotic surgery, doesn’t mean that they are. You need to find out about the extent of their robotic training. These procedures often take about 1.5 hrs sometimes more, but if they are taking 6-8 hours then they are not a safe surgery.
I have a back up robot in case the robot breaks and have been doing this close to two decades so my team is one of the best in the world and are capable of fixing any issues. Since I am trained in laparoscopy and open, I can get the patient through without any problem. In over 6000 surgeries, I never had to convert to an open operation so that is the record. I perform all robotic surgeries from beginning to end and that is my commitment to my patients.
Just because someone can drive a Lamborghini does not make them a NASCAR champion!
It is a popular belief that if a man lives long enough he will develop prostate cancer, but it won’t be what kills him. The pendulum has shifted regarding this notion given the more aggressive nature of the disease when it presents in the younger adult male. Where do you weigh in on this and its relative risk throughout the various stages of the adult male?
About 30-35% of prostate cancer is aggressive or moderately aggressive and needs to be treated. There are roughly 160,000 new cases annually and it causes 27,000 deaths every year with a couple million men walking around with it. There are centers of excellence committed to this disease where the surgeon, team and whole program are dedicated to this which can make all the difference in not only survival, but quality of life. Once there, it is crucial to observe closely how the surgeon behaves and whether he examines you himself and so forth. The way they are in the office can reflect how they are in the operating room.
From your perspective should every man of a certain age be followed by a urologist, in general? When is it ok in terms of prostate cancer risk or disease to be only seeing your internist or family doctor?
Seeing a family doctor or internist is great until age 40 which is when I recommend a baseline PSA be done for the record. If this is okay and the patient has no symptoms or any significant risk factors, then 45-50 is when a urologist should come into the mix. There is no age limit if a man has symptoms, is high risk or has significant family history. In these situations, urology should be immediately involved.
When do radiation or chemotherapy come into play with prostate cancer?
These are good treatment modalities as a plan B. As adjuvant therapies. Too many patients are being radiated upon initial diagnosis with some of this financially driven. Additionally, hormone medications can accompany radiation thereby contributing to patients having problems with sexual function. Lupron is an example. Using radiation for primary treatment means should there be a recurrence of disease, the patient can’t be operated on in the future. With radiation, as time goes on more side effects like rectal bleeding come into the picture. This is why it is so important to talk to a radiation oncologist and a urologic oncology surgeon to make the decision that is right for you. The approach to prostate cancer is not a one-treatment-fits-all. You need individualized care and personalized treatment. What works for you, might not for someone else.
Where do you see disease incidence and treatment going for prostate cancer in the next 10 years?
As we become more and more sophisticated and smarter on who to treat and who not to treat, we will prolong life and enhance its quality. I believe the data and technology will come where we can look at two comparable 55 year old patients with cancer—where on the surface they appear the same—and know who needs to be operated on and who can be closely monitored. Hopefully, this is in our near future.
The take home message... To those diagnosed with prostate cancer, there is life after this silent killer. Experience matters and you should choose wisely. In the hands of committed surgeons, you will do well and, hopefully, have the trifecta.
SOURCES:
(1) (3) Bibbins-Domingo K, Grossman DC, Curry SJ. The US Preventive Services Task Force 2017 Draft Recommendation Statement on Screening for Prostate Cancer: An Invitation to Review and Comment. JAMA. Published online April 11, 2017. doi:10.1001/jama.2017.4413
(2) American Cancer Society, link here.
For more information, from the National Institutes of Health's (NIH) National Cancer Institute, click here.
NOTE(S):
To view ACSH's Director of Medicine Dr. Jamie Wells and Dr. David Samadi's recent television appearance answering the public's health questions, click here.

Dr. David Samadi (left), Dr. Jamie Wells (center), Host Ernie Anastos (right)