The desire to detect cancer before it spreads to other areas of the body remains one of the priorities of the cancer research field. Why? Because, early detection of tumorous cancers could potentially be cured by surveillance and surgery alone, before metastasis occurs.
Although this year was a banner year for new cancer treatments, seeing Food and Drug Administration (FDA) approval of two separate novel cancer therapies (leukemia, lymphoma), progress remains slow.
So, while we wait for new cancer treatments to come to fruition, some groups think that early detection is the new horizon of cancer treatment and a new paper in Science present an improved blood test for cancer detection called CancerSEEK.
CancerSEEK looks for two separate markers for cancer - genetic mutations and protein biomarkers. It can not only detect eight common cancers (ovary, liver, stomach, pancreas, esophagus, colorectum, lung, or breast) but, also to identify the organ with the tumors.
They designed a polymerase chain reaction (PCR)-based assay to identify the presence of mutations in 16 genes that are frequently involved in cancer when mutated.
They focused on four challenges.
- The test must query a sufficient number of bases to allow detection of a large number of cancers.
- Each base queried in the test must be sequenced thousands of times to detect low prevalence mutations.
- There must be a limit on the number of bases queried in the test because the more bases queried, the more likely that artifactual mutations would be identified, reducing the signal-to-noise ratio.
- The test must be cost effective and amenable to high throughput, factors that limit the amount of sequencing that can be performed.
They also had to make sure that the blood test had a hight level of specificity, to avoid false positives. In order to ensure confidence, they folded the identification of specific biomarkers into the DNA assay.
Many proteins potentially useful for early detection and diagnosis of cancer have been described. The group found 41 proteins that had been shown to detect at least one of the eight cancers of study with high specificity. Out of those, eight were shown to be able to discern between a cancer patient and non-cancer patient.
Built on the protein and DNA information, CancerSEEK was used to study 1,005 patients who had been diagnosed with Stage I to III non-metastatic cancers of the ovary, liver, stomach, pancreas, esophagus, colorectum, lung, or breast.
The results were very promising, as can be seen in the figure below.
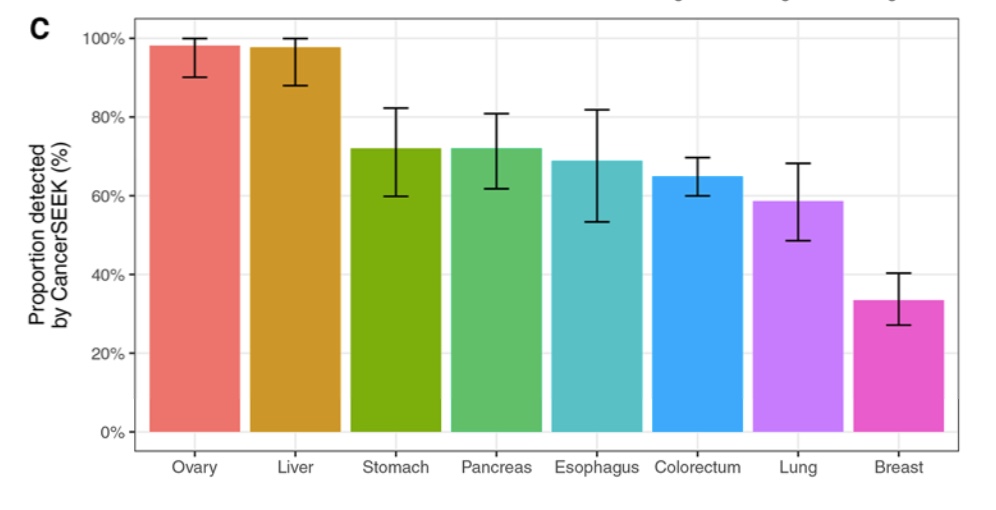
The test was able to detect disease in about 70% of the people tested, on average. Importantly, CancerSEEK is very good at being specific. Only 7 out of the 812 healthy controls tested scored positive for cancer. That's less than 1% error.
The effectiveness of CancerSEEK varied widely. It could detect almost all (98%) ovarian cancer, but it was not the same story for breast cancer at only 33% detected.
On a sidenote, ovarian cancer happens to be one of the cancers that, in particular, has almost no mechanisms of early detection. Therefore, rising to the top of a technique like this is perhaps a stroke of good luck for that particular cancer patient community.
Both CancerSEEK's ability to detect cancer and identify the cancer tumors' origin increased in the later stages of the cancer.
So, although CancerSEEK will not be available in your physician's office just yet, it is being used in a study that will test CancerSEEK in some 10,000 healthy individuals who will be followed for five years. And, who knows? Maybe a blood test to detect cancer will be in our future. What we will do with that information is another question entirely.
Source: Joshua Cohen at al. Detection and localization of surgically resectable cancers with a multi-analyte blood test Science 18 Jan 2018: DOI: 10.1126/science.aar3247