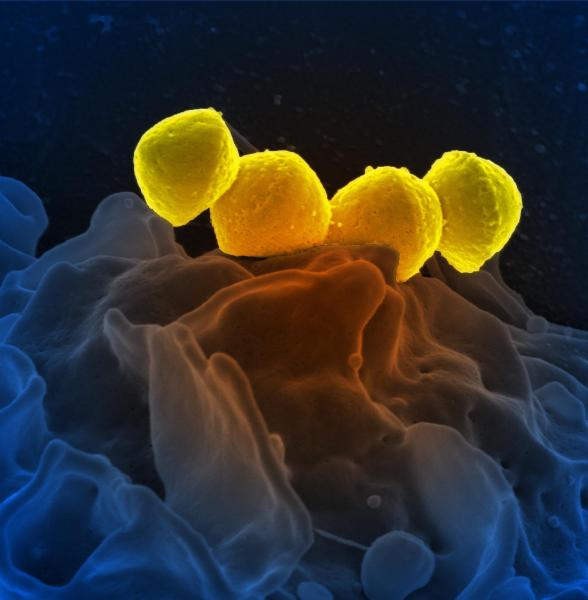
It's the stuff of nightmares — a small injury that turns deadly as a result of the unbridled proliferation of a common bacterium, such as Streptococcus sp. Known as necrotizing fasciitis, necrotizing soft tissue infection (NSTI) or in headlines flesh-eating bacterial infection, the condition can result in amputation of an affected limb, toxic shock, and loss of life. But what allows the bacteria to run amok in some people, while others have a small wound that heals easily? Recent research supplies one clue — a lack of antibodies against the causative bugs.
Dr. Anshu Babbar from the Helmholz Centre for Infection Research, Braunschweig, Germany, and colleagues investigated the role of pre-existing antibodies to Streptococcus pyogenes in patients who harbored that bacterium. They sampled blood from people with (14) and without (2) NSTI.
At the beginning of the study they found that the plasma from NSTI patients did not contain antibodies to S. pyogenes or to any of the toxins that bacterium produced. In contrast, the patients who had soft tissue infections caused by S. pyogenes (but not NSTI) did present with antibodies to both the bacteria and to many of its toxins.
Half of the NSTI patients were treated with intravenous infusions of IgG antibodies (IVIG), and three days later their plasma was again tested for the presence of antibodies against the bacterial toxins. The investigators found that the untreated patients did develop antibodies against some, but not all, of the S. pygenes toxins. In contrast, those who had been treated with IVIG at day 0 of the study developed antibodies against most of the toxins. They noted
“These results indicate that IVIG treatment provides the NSTI patients with a pool of antibodies against a wide array of exotoxins that complement those that may not be induced by the natural infection."
and
“[P]re-existing antibodies against the whole repertoire of exotoxins…may prevent the progression of soft tissue infection into severe NSTI. The opposite could also be the case and patients lacking antibodies against specifc S. pyogenes exotoxins may be at risk for developing NSTI.”
Importantly, they noted that IVIG treatment must be initiated very early in the development of NSTI — once the condition is established the treatment will not be effective.
These results suggest a means of detecting which soft tissue infections are likely to progress to NSTI. If an antibody test demonstrates that antibodies to the infecting bacteria aren’t present, then early treatment with IVIG could prevent the progression to NSTI. Of course, this research used only one type of bacteria, and it’s not clear that other types that could cause NSTI could also effectively be treated with IgG, but it presents a framework to discover if these results could be generalizable to other infective organisms.