Before we jump in, there is one caveat, the medical data surrounding Covid-19, is in flux because we lack standardization of information globally. After all, our data sources are still busy treating patients and not cleaning up messy data, and because there are variables that we need even to identify.
Transmission
We do know that Covid-19 is transferred from an infected individual to a susceptible one by direct person-to-person contact or indirectly through viral particles shed by the infected into the intimate environment. Those transmissions can occur in “the household, workplace, school or randomly in the community,” and that is part of the rationale behind social distancing. The halo of transmission extends, we believe, for about six feet around an individual. But there is a more crucial preliminary finding; the current data suggests that “approximately one-third of transmission occurs in the household, one third in schools and workplaces and the remaining third in the community.”
Incubation
Once the virus enters your body, unless it is immediately killed, it sets up shop and begins to replicate. It requires a critical mass to start overwhelming your body’s defenses – the incubation period. The estimates of the incubation period vary, with the average being roughly 5.1 days based on reports from China’s Wuhan province. [1] But the incubation time increases up to 11 days when accounting for 97% of patients, not just the middle. Out of an abundance of caution, you might add a day or so to capture everyone in the range. Let’s call it 2 weeks. This is the point when you will become symptomatic or not. We will return to the symptomatic in a moment.
Just as the virus must acquire a critical mass to challenge your defenses, it requires time to become so manifested that you can transmit the virus to others – it doesn’t happen right away. The assumption is that infectivity, the ability to infect others, begins about five days after the virus establishes itself. More importantly, infectivity is estimated to occur 12 hours before symptoms are present. And there is variance in how infective you are to susceptible individuals; it too follows a distribution. The current study assumes “that symptomatic individuals are 50% more infectious than asymptomatic individuals.” That infectivity plays out in how many individuals are subsequently infected, the R0, which seems to be in the 2.0 to 2.6 range. Seasonal flu has an R0 of about 1.3, so Covid-19 is more infectious.
Symptomatic patients
Everyone responds differently to Covid-19, and again, we are not sure of what those factors are or will be. But there is a range, from asymptomatic to critically ill. Each grouping within that range requires different care. Let’s take them in order of severity. For asymptomatic and those with mild manifestations (temperature and cough), the key is isolating them from others preventing infections; and symptomatic relief from over-the-counter medicines, antipyretics, and antitussives. The data from China suggests that 40 to 50% of Covid-19 infections fall into this category – truly a cup half empty vs. half full dilemma. That actual percentage will vary based on the resilience or frailty of the population being considered.
Frailty reflects how much of your physiology is out of balance. Diabetes might be thought of as frailty of glucose metabolism, asthma as the frailty of our respiratory tracts immune response. Frailty reflects our physiologic age, not our chronological years. It increases with age, and it is easier for scientists and public health officials to use age as a shorthand way to describe frailty.
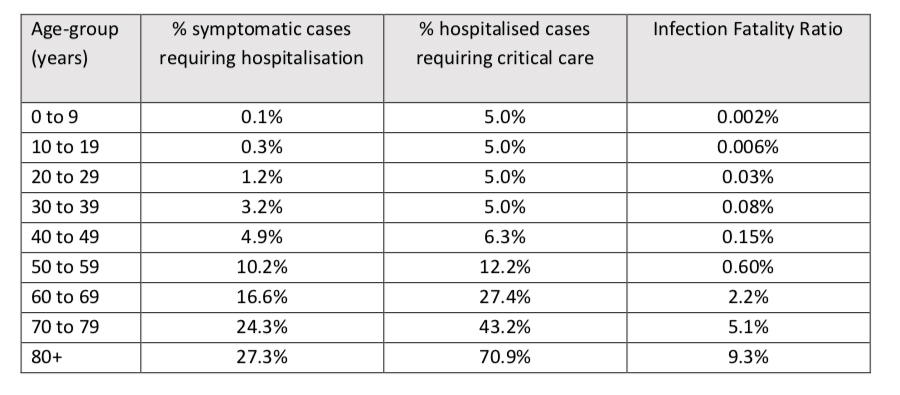
The 40-50% figure I just mentioned is based on the aggregate frailty of the Chinese people in Wuhan; their ages and specific frailties may well differ from our population. For example, smoking is far more prevalent in China than in the US. Our best current data, whether from China or Italy, is difficult to translate so public health officials will adjust estimates in directions to be safe. The modeling by the Imperial College’s Covid-19 response team, placed the mild cases, “sufficiently symptomatic to self-isolate,” at 66% in their models.
The remaining 33% require hospitalization for a variety of reasons. Some individuals are hospitalized because it is the safest option; after all, how do you effectively isolate passengers on a cruise ship, individuals in nursing homes or other institutions, including prisons, and the homeless. Many other hospitalized patients will be symptomatic and at a high enough risk to require more sophisticated monitoring than a thermometer. Given that Covid-19 initially attacks the respiratory system, individuals with respiratory diseases (asthma, COPD) or symptoms related to shortness of breath or diminishing ability to absorb oxygen into their bloodstream require close monitoring. The estimates place these moderately symptomatic patients at 70% of those hospitalized [2]. The best estimates are that these individuals will need 8 days of hospitalization. Those days can be reduced, in the aggregate, by deploying more home health services, especially telemedicine, and when necessary, home visits.
The remaining 30% require invasive mechanical ventilation in the setting of an ICU. For those following the math, that is roughly 10% of the entire population at risk. Their length of stay in the hospital is approximately doubled, with about 10 of those days spent in the ICU. The assessment by the Imperial College notes that the aggregate length of stay they have calculated at 10.4 days for everyone hospitalized is “in line with estimates for general pneumonia admissions.”
Fourteen days of bedrest takes a toil beyond whatever process put you in bed for that length of time. Your muscles weaken from disuse. Lying in bed on a ventilator fighting an infection often requires 5000 or more calories a day, and normal iv fluids provide only a small fraction of that amount. While we can supplement nutrition intravenously or by feeding tubes, it is fair to say that patients will be discharged relatively malnourished. Typically, after surgery, it takes about 4-6 weeks after discharge to “feel like yourself.” While I have seen no data on post-discharge care, it is a reasonable assumption that those receiving critical care in the hospital will need several weeks of post-discharge recovery. In the case of the elderly, and they are the ones most at risk, that care will be delivered through rehabilitation and skilled nursing facilities.
Covid-19’s Time Course
Here is Covid-19’s basic course, and again, these numbers are estimates based on the available data, and there are large confidence intervals, signifying significant uncertainty around all of them.
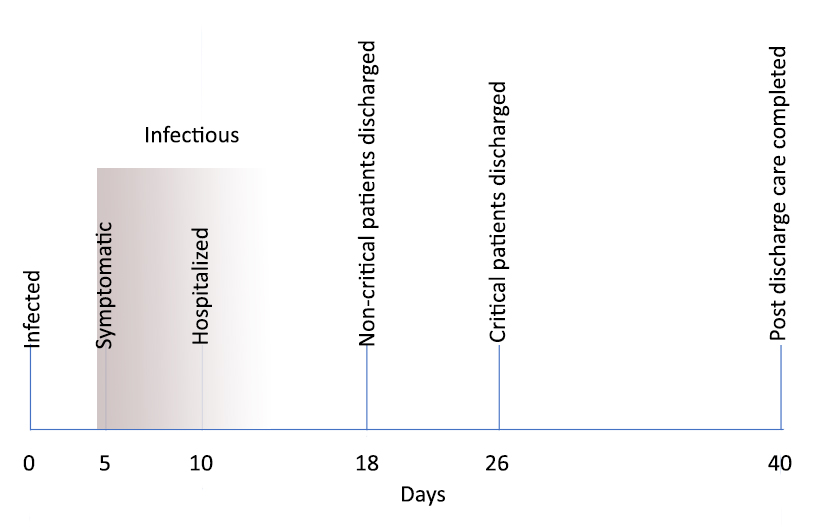
This disease timeline is the basis for estimating how long we must practice social distancing and shelter in place. When this data is aggregated to our population, it forms those peaked and flattened curves.
Frequently, as a physician, we are faced with delivering bad news. If you have the opportunity, it is often better to try and "prepare" the family by being increasingly pessimistic, so that hope, which is so vital in these situations, dissipates slowly rather than dramatically removed. We "hang crepe," referring to the bunting that surrounds a funeral. From my perspective, the steps we have taken are not going to be in place for just two weeks; they are going to be here for some time. If you follow the estimates of the Imperial College, and they are reasonable, we are looking at several months. Here is their graphic. I will give them the last word.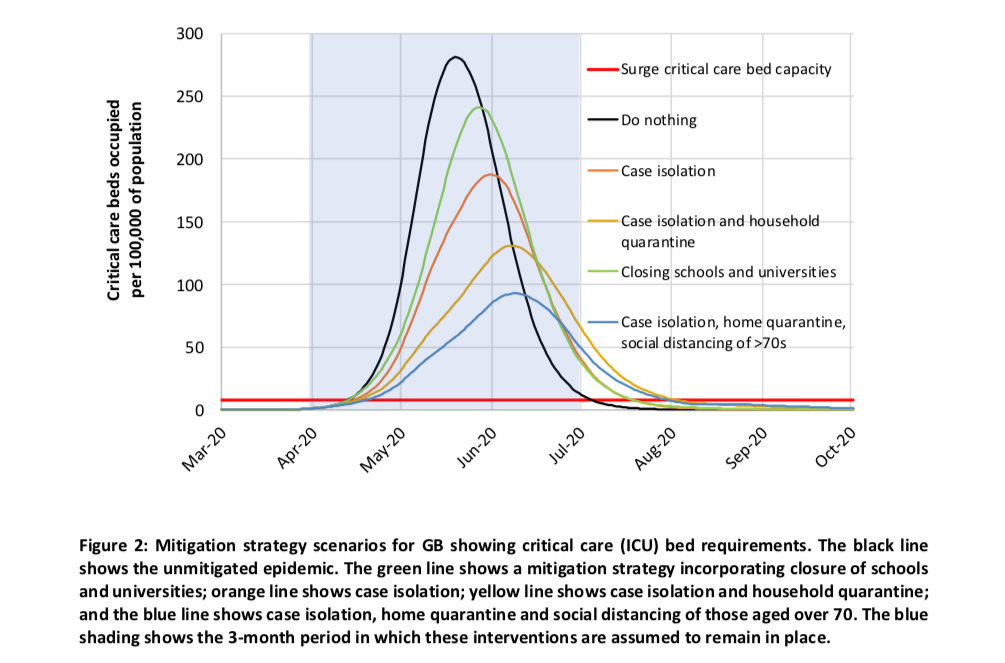
“However, there are very large uncertainties around the transmission of this virus, the likely effectiveness of different policies and the extent to which the population spontaneously adopts risk reducing behaviours. This means it is difficult to be definitive about the likely initial duration of measures which will be required, except that it will be several months. Future decisions on when and for how long to relax policies will need to be informed by ongoing surveillance.” Emphasis added
[1] The Incubation Period of Coronavirus Disease 2019 (COVID-19) From Publicly Reported Confirmed Cases: Estimation and Application Annals of Internal Medicine DOI: 1 0.7326/M20-0504
[2] That 70% translates into about 21% of the total population.
Source: Impact of non-pharmaceutical interventions (NPIs) to reduce COVID- 19 mortality and healthcare demandImperial College Covid-19 Response Team




