We may need to revise the lyrics from a classic musical:
"Just a spoonful of sugar makes the medicine go down... in the most delightful way."
Robert and Richard Sherman, Mary Poppins (1964)
"Just a spoonful of sugar and a gas mask makes the medicine go down... in the least repulsive way."
J. Bloom, ACSH (2020)
WHAT IS THE PREMISE?
A small, preliminary, but interesting study at the Kennedy Institute of Rheumatology at the University of Oxford (UK) asks the question "Is it possible to make vaccines work better in the elderly?" This question is now especially relevant since only yesterday, the first doses of Pfizer/BioNtech's COVID-19 vaccine were administered to healthcare workers in the US.
However, there are two difficult issues in the mix. First, older people are far more likely to become seriously ill or die of COVID. Second, vaccines are not as effective in the elderly. Will this lead to reduced coverage against COVID in older people?
“Older adults are at high risk of being severely affected by infectious diseases, but unfortunately most vaccines in this age group are less efficient than in younger adults.”
Ghada Alsaleh, Ph.D., Kennedy Institute of Rheumatology, University of Oxford, UK.
Alsaleh and colleagues are studying a process called autophagy ("cellular self-eating") in mice. Autophagy can be thought of as a "built-in recycling plant" in which damaged cells, for example, T-cells of the immune system, digest themselves and the cellular components are released and reused. Autophagy is one of the methods that keep the immune system healthy. The difference in autophagy was shown in mice; older mice were less able to perform this essential function than those in younger mice.
Autophagy plays a part in removing remove damaged proteins and other junk from cells. Source: Tanpaku
A similar effect was seen in two small clinical trials. Both older and younger volunteers were enrolled in clinical trials to evaluate potential vaccines for respiratory syncytial virus (RSV) and the hepatitis C virus (HCV). As was the case in mice, in younger people autophagy of T-cells (1) increased upon vaccination, but this effect was muted in older people.
What to do? It is known that a naturally occurring chemical (part of a class called low molecular weight polyamines) called spermidine can give the autophagy process a boost. (The way this works is complex and beyond the scope of this article. And my brain.) Could the addition of a simple chemical really make a difference in the response of the elderly to vaccines?
Laboratory analysis of T-cells from older people revealed that they had less spermidine in their cells than in younger people. But when spermidine was added to the blood cells of older people the level of autophagy in T-cells was restored to that in younger people.
“Our work suggests that boosting autophagy during vaccination may help make vaccines more effective for older people.”
Ghada Alsaleh, Ph.D
Although the evidence of restoration of autophagy is limited, this is an intriguing idea because it could be easily tested. Spermidine is found in a variety of foods so toxicity is unlikely to be a problem, and the impact of the spermidine on autophagy has been demonstrated. But it will take time from this point to prove whether the chemical will provide any real-life advantage to older people. It is a long trip from a Petri dish to the bloodstream.
AND JUST BECAUSE CHEMISTS CAN'T HELP THEMSELVES
Spermidine's "chemical cousins" are a bunch of doozies. You have smelled at least some of them. And as their names suggest, their odors are not exactly reminiscent of a bouquet of lilies. Here are four low molecular weight polyamines for you to sniff on (2). Just not at the dinner table.
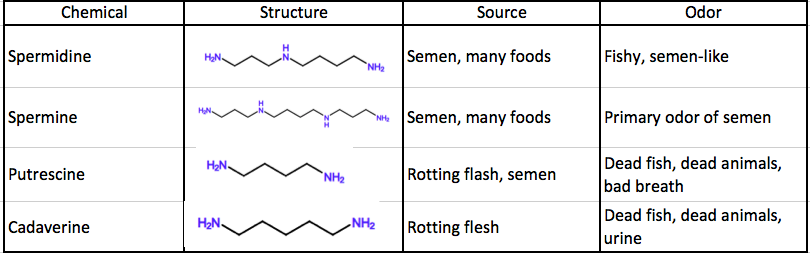
NOTES:
(1) T-cells are one type of leukocyte (white blood cell) that is an essential component of the immune system.
(2) I wrote about putrescine and cadaverine in 2018 (2).




