Why it may seem a bit like knowing the number of angels dancing on the head of a pin understanding the relative amounts of virions and viral particles responsible for COVID-19 will provide some insights into “pandemic dynamics” and our immune responses. The scientists used three studies of rhesus macaques infected by COVID-19; they were our closest relative, for which we had good data.
The rhesus monkeys were infected with the virus, sacrificed on day 3 or 4 of infection, and quantitative measures were made of the virions present. That information, coupled with our knowledge of coronaviruses in general and some mathematical manipulation, form the basis of their findings.
Counting COVID-19
A quick reminder. PCR tests for COVID-19 identify the presence of “naked” RNA, not the capsule necessary for delivering the virus, not the virion. It is a proxy for virions, and large amounts strongly suggest the presence of current infection. A more accurate way to determine the presence of virions is to measure the number of cells killed by their presence in cell culture the TCID50 [1]. This is a far more accurate proxy for those “infectious units,” the virion
Why values are unclear
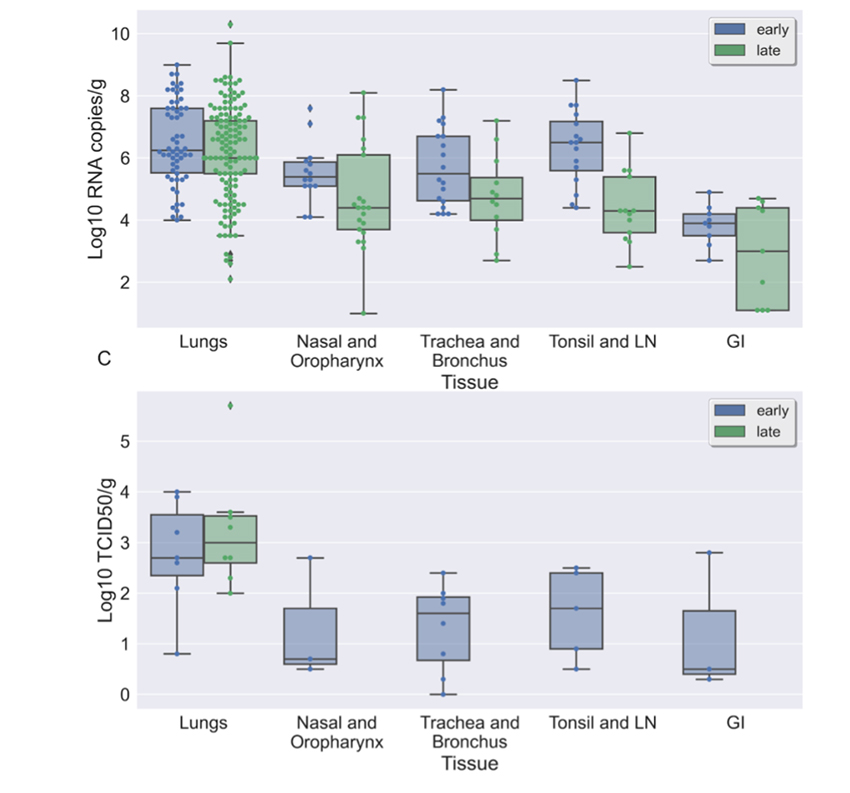 Let’s get started by considering this graph depicting PCR and TCID50 counts in the respiratory and GI tracts and the local lymph nodes and tonsils, the stand-in for our immune system. As we expect, the values differ early and late in the infection and within different tissues. In addition, there is a wide variation in viral load, six orders of magnitude reflecting susceptibility and timing of sampling.
Let’s get started by considering this graph depicting PCR and TCID50 counts in the respiratory and GI tracts and the local lymph nodes and tonsils, the stand-in for our immune system. As we expect, the values differ early and late in the infection and within different tissues. In addition, there is a wide variation in viral load, six orders of magnitude reflecting susceptibility and timing of sampling.
There is much more evidence of infection in the lungs than in our mouth and nose (nasal and oropharynx), so it is possible that our PCR testing is less sensitive to the presence of infection, creating undercounts.
The PCR counts are far higher than the TCID50 counts, so it is also possible that PCR counts are too sensitive, identifying infection that is resolving. Cell culture to “prove” infection takes too long clinically, PCR is a reasonable proxy, but it is far from precise.
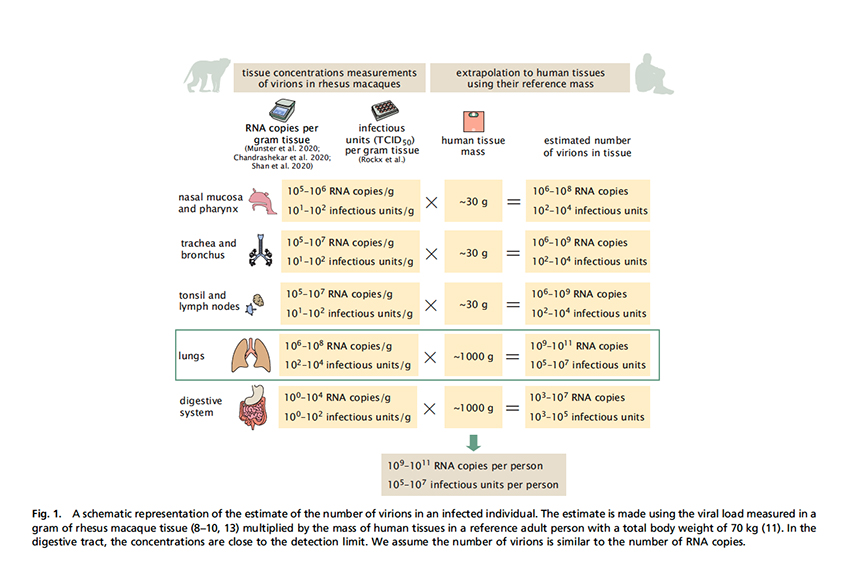
Number of virions in an infected individual
This second graph shows the number of RNA copies from PCR testing or infectious units from those TCID50 counts in the organs of the rhesus monkeys. Using the weight of the lungs, we can extrapolate to the number of virions in a human. There are 109 to 1011 RNA copies, but 4 fold fewer infectious ones. Thus, the number of virions is between 100,000 and 10,000,000. To simply extrapolate to women and children, based on size, would be inaccurate as both groups have different responses to COVID-19 than men. Some studies suggest that the viral load would be further reduced by another order of magnitude for children, but who really knows?
Number of cells infected
For this calculation, the researchers used data on other coronaviruses to estimate that every infected cell contains 10 to 100 infectious virions. Having estimated the total number of virions present, they can also estimate the number of cells infected. At the peak of infectivity, 104 – 106 cells are infected, about 0.001% to 0.00001% of our total.
Not all cells are susceptible to COVID-19. To infect a host cell, COVID-19 needs one of two receptors, angiotensin-converting enzyme (ACE) and transmembrane protease, serine 2 (TMPRSS2). They are found in about 1-10 % of our lung and airway cells, further reducing the choice of cellular hosts to the range of 100 to 10,000 cells.
A hundred virions in 10,000 cells, 0.0001% of our total cells, is all that is necessary to kill us. We may be more fragile than we would like to believe.
Our cellular defenses
IgG antibodies found in serum roughly three weeks after infection measure around 10 μg/mL, but only about 5% are directed at COVID-19’s spike and can neutralize it. Using the weight of the IgG, they estimated the number of antibodies present. The COVID-19 virion has about 30 to 40 spikes. Research in other viruses found that 3 to 4 sites need to be bound by the antibody to neutralize the virus.
Based upon that information and a little math, we mount a significant response, producing an estimated 100 to 10,000 antibodies against every spike. Similar calculations for T cells suggest that there are 100 to 1,000 T cells focused on COVID-19 for each infected cell.
Virions and severity of disease
We still do not know how the number of virions correlates with the severity of disease. Some studies suggest the viral load is similar among the asymptomatic and critically ill; others find significant differences. The researchers note that viral shedding continues for more extended periods in the severely ill. Their calculations suggest that viral load maybe “1-2 orders of magnitude higher” in the non-survivors.
Just for Fun
Can we answer the question of how many virions “dance on the head of a pin?” Here is the researcher’s calculation.
Assuming 1-10 million active infections at any given time, there are 1017 to 1019 RNA copies or 1013 to 1015 virions. A virion weighs about 1 fg, a femtogram, or 1 x 10-15 grams. I will spare both you and me the math. There are approximately 0.1kg to 10 kg virions out and about at a given moment in time. At the upper limit, 22 pounds of virus are responsible for the current global totals of 3.72 million deaths and 173 million infections.
[1] The TCID50, the amount needed to kill 50% of the cells, is used to calculate “infectious units
Source: The total number and mass of SARS-CoV-2 virions PNAS DOI: 10.1073/pnas.2024815118




