Aerosols or Droplets
“Aerosols are microscopic liquid, solid, or semisolid particles that are so small that they remain suspended in the air.”
- Aerosols are characteristically considered 5 microns or small; droplets are larger.
- Droplets are more frequently found in coughs and sneezes; we produce aerosols whenever we exhale
- Droplets are larger and heavier, and they travel shorter distances – roughly 2 feet; Aerosols are smaller, lighter, and travel further.
- The relative importance of each is subject to some debate, although both the WHO and CDC officially acknowledged aerosols are the prime mode of transmission this Spring.
- Observational data on superspreader events being indoors, with poor ventilation, crowded conditions, vocalization make a strong case for aerosols over droplets
“For airborne transmission to occur, aerosols must be generated, transported through air, inhaled by a susceptible host, and deposited in the respiratory tract to initiate infection. The virus must retain its infectivity throughout these processes.”
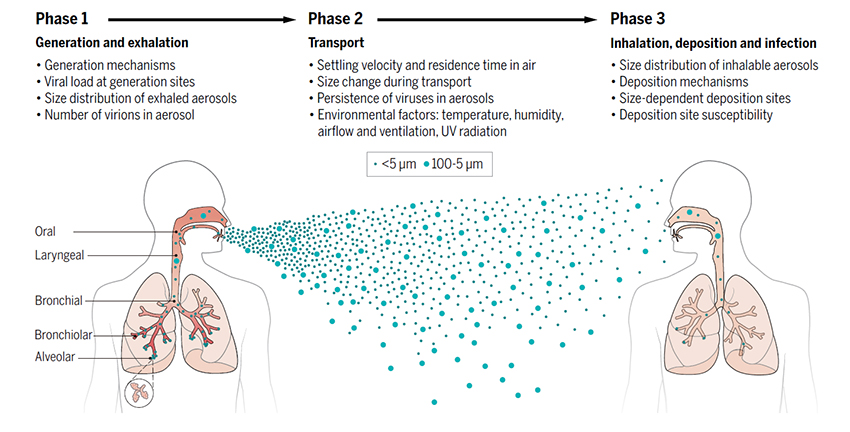
- Droplets are formed primarily by saliva in our mouths. Aerosols come from throughout the respiratory tree and are formed by shearing forces associated with air movement (exhalation) – more forceful air movement creates more aerosols
- The size of the aerosol particles is crucial; smaller particles are found deeper within the respiratory tract. But aerosols contain multiple sizes, roughly placed into four groups, each differing in their contribution based on their anatomic source, how they are produced, and the associated respiratory activity, i.e., breathing, singing, shouting, or trying to “catch our breath.”
- Children produce less aerosol volume than adults because of the size of their respiratory tracts.
- But breathing produces more aerosols because it is continuous than those created by episodic sneezes or coughs.
"The viral load of aerosols is a key factor in determining the relative contribution of airborne transmission."
- We still do not know the required viral load, and getting an answer is difficult for a variety of measurement problems
- Viral particles are more significant in smaller aerosols. Some studies have suggested that a patient with COVID-19 exhales 100,000 to 10,000,000 particles per hour; other studies show no detectable virions. Many factors mentioned in the creation of aerosols explain the resulting “interpersonal variability” to exhaling viral loads.
- A further uncertainty is a gap in our knowledge of the dose necessary to elicit infection. For influenza, we know that far less is required when an aerosol is inhaled deep into our lungs compared to the quantity necessary to inoculate an infection via a nasal swab – location matters, as does susceptibility
They fly through the air with the greatest of ease
- The force of exhalation begins their transport, but gravity, temperature, humidity, the presence of ultraviolet light, and the electrical charge in the atmosphere all alter their course.
- The aerosol size is also dynamic, influenced by evaporation, coagulation, and deposition, reducing how long and for what distance they remain airborne. We can calculate those distances but these computations involve so many variables and assumptions that the numbers we determine put us in the general area of the ballpark.
- That said, there are more virions closer to the source. The concentration decreases with distance and the mixing with the air and its flow around us.
- Transmission is favored at lower temperatures. The relative humidity also plays a role; drier air results in greater evaporation and diminished aerosol volume. UV light kills COVID-19; sunlight is a disinfectant. This helps to explain some of the seasonality of respiratory viruses.
- Of course, we spend 80% of our time indoors
"Airflow strongly influences the transport of virus-laden aerosols, in contrast to droplets, which are rapidly deposited because of gravity."
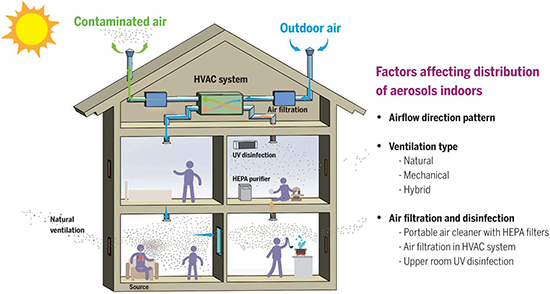
- The greater airflow outdoors increases dispersion; indoors, we rely on the ventilation provided by our windows or, more likely, our heating and cooling systems. These systems, in turn, are impacted by whether they involve forced air, conduction, the presence and absence of walls, doors, and other obstructions. Those Plexiglas barriers impede droplets, but they inhibit airflow
- HEPA filters will remove 99.97% of the aerosols of concern, but the airflow can alter their efficacy in the room – hotspots, with greater viral risk, have been demonstrated in elevators, classrooms, and supermarkets despite HEPA filtration
“Once inhaled, virus-laden aerosols may deposit in the respiratory tract of a potential host…Infection may be initiated at the deposition site if the virus remains infectious and appropriate receptors are present.”
- Large aerosols settle in the nose and upper respiratory tracts. The smaller, more viral-rich aerosols penetrate more deeply into our lungs.
- But their deposition onto the lining of the lung (alveoli) is due to Brownian motion (random motion) and the electrostatic charge present within the aerosols, which can cause viral particles to be attracted or repelled from the alveoli.
- Of course, the presence of underlying lung disease alters the situation with structural changes and mucus, which can act as a barrier to viral implantation.
- Once deposited, virions need a suitable cellular receptor, the sites where the spike attaches. At that point, the strength of the patient’s immune response comes into play.
Droplets contaminate surfaces, so hand washing and cleaning counter surfaces are helpful easily performed mitigation factors. Our experience in getting healthcare workers to wash their hands indicates that this is easier said than done. Even a cursory reading of this article suggests the overwhelming number of variables that can affect the airborne transmission of COVID-19.
“Physical distancing, a mitigation put in place to address droplet transmission, is also effective in reducing the chances of aerosol inhalation because aerosol concentrations are much higher in close proximity to an infected individual.”
Increasingly, the evidence is that respiratory virus transmission, including seasonal flu, and COVID-19 are due to aerosols we generate. And we have good evidence that from 20% to up to 50% of individuals infected with COVID-19 are asymptomatic and “generally continue to be involved in social activities, leading to airborne transmission.”
Masks are not entirely efficient, but they are the best and cheapest mitigation effort the science of airborne transmission supports - even ill-fitted cloth masks can reduce viral transmission by 50%. In the war against COVID-19, is wearing a mask too great a price to pay to save half of your fellow citizens from becoming ill? Will there be a day when we say to those who have worn a mask, “Thank you for your service?”
Source: Airborne Transmission of Respiratory Viruses Science DOI: 10.1126/science.abd9149




