The study itself was straightforward. How well did disclosure by physician authors in these journals match up with their disclosures in the physician Open Payment database? The dataset consisted of all articles published in 2017 in these journals where the first or last authors (traditionally the primary authors) were physicians and had Open Payment records. Of the close to 400 original research reports between the two journals, 31 articles from each meet these criteria and were analyzed.
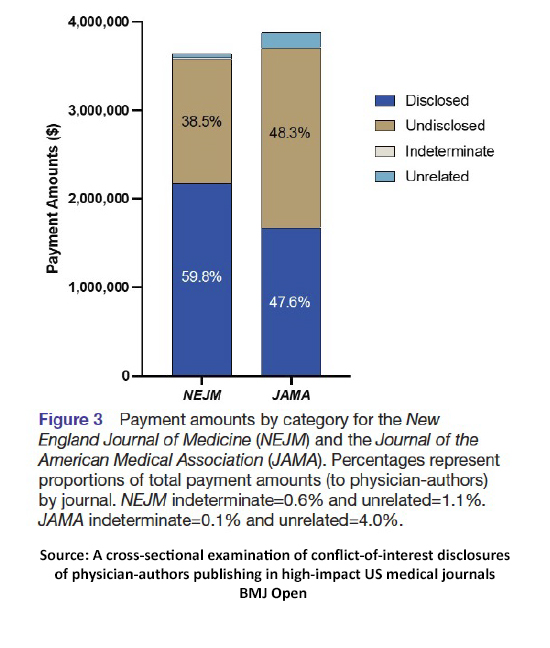 Total payments to all 118 authors $7,476,049 in general payments – roughly evenly split between those writing in the NEJM or JAMA
Total payments to all 118 authors $7,476,049 in general payments – roughly evenly split between those writing in the NEJM or JAMA- One hundred six authors received payments ranging from $6.36 to $1,486,929; the mean was in the $60,000 area. It is again important to point out that payments reflect a range of activities, from research funding to speaking or consulting, royalties, and the occasional lunch or dinner.
- 86 of those 106 authors, 81%, received undisclosed payments. [1]
- The 23 most remunerated physicians were all among those with undisclosed payments. They received 84.5% of all compensation, roughly $6.3 million
Could these thought leaders’ disclosure practices be more “do as I say, not as I do?” The evidence would certainly suggest that possibility. The researchers are quick to take no position on the intent of these individuals.
“…the authors of this study take no position on the physician authors' intentions in non-disclosure of their COIs; we characterize the issue as a ‘process problem’ rather than a ‘people problem,’ especially in light of the patterns observed in COI disclosure rates regardless of the journal’s disclosure process and regardless of payment amount.”
That may well be the case; perhaps these disclosures are not felt germane and do not rise to the level of even being considered. That said, there are ways we might increase transparency. The researchers suggest tying Open Payment data to disclosure forms. We might also standardize conflict of interest forms, so they don’t need to be redone every time a journal submission is made. And an easy change that we can make today is to move those disclosures to the top of the article so that you can apply those ‘grains of salt” as you read rather than after you have finished.
“Finally, this report was limited to financial COIs. Non-financial COIs in the form of strong intellectual, emotional, political, and religious convictions might exert at least as much influence as financial COIs.”
If nearly 48% of payments went undisclosed in two of our premier journals, the chance of us addressing the bias introduced by non-financial conflicts of interest will be more words than deeds.
[1] In this study, an undisclosed payment meant that the physician received a payment not disclosed in their conflict of interest statement to the journal, and the company making the payment offered “a product that could broadly be considered related to the area of inquiry.” For example, an author reporting on cardiovascular research receiving and not disclosing funds from a maker of blood pressure medications.
Sources: First, thanks to the "disinformation chronicles" for directing us to this research; it's author is decidedly against ACSH. Being open, curious, and non-judgmental has its advantages, Paul.
A cross-sectional examination of conflict-of-interest disclosures of physician-authors publishing in high-impact US medical journals BMJ Open DOI: 10.1136/bmjopen-2021-05759