Breastfeeding is recommended for an infant's first 12 months of life because of its correlation with improved health.
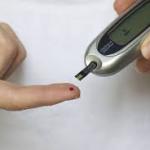
diabetes
A study published in Annals of Internal Medicine, from the University of Chicago presents a cost an
Insulin resistance is a hallmark of type 2 diabetes, and occurs in more than one type of body tissue. For example, insulin-resistant muscle will not respond normally when insulin directs it to take up glucose from the blood.
Although known mainly for their adherence to an older, simpler way of life, some Amish folks also have a genetic advantage with respect to longevity and the likelihood they'll develop diabetes.
By now, everyone who’s interested knows that there are 2 main types of diabetes — type 1(in which the pancreas doesn’t produce insulin) and type 2 (in which body tissues don’t or can’t respond appropriately to insulin), typically seen in adults.
When we think of the word cure, we think of it as the end when, in fact, it is often the end of a beginning.
As a society, we immediately understand a broken arm. A gaping wound. The wasted appearance of a body overrun by cancer.
Apparently, you can make any claim with an Asterisk (*), so long as the asterisk clarifies that your claim isn't true. In one of Dr.
Ask yourself how often you ever think about your ability to hear? How much you value it? How much you—and your loved ones—would be impacted if it were gone or profoundly diminished?
Type 1 diabetes – the kind that involves loss of the insulin-producing pancreatic beta cells — requires that insulin be injected daily, or several times daily.