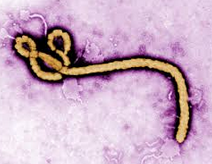
 Even in the archives of successful vaccine campaigns, this one really stands out.
Even in the archives of successful vaccine campaigns, this one really stands out.
In only one year, a vaccine that is astoundingly effective against Ebola, the highly contagious and often lethal virus that has gripped much of the world in fear, was miraculously discovered by an multinational group that consisted of scientists from 12 research centers, as well as the World Health Organization (WHO). The vaccine is manufactured by Merck.
The group s recent paper in the Lancet reported that individuals who were vaccinated within 10 days of infection were protected 100 percent (!) of the time. Even people who did not receive the vaccine until 21 or more days post-infection were protected 75 percent of the time. Considering that there wasn't even a therapy to treat Ebola, let alone prevent it, these results are even more impressive.
Just as amazing is the speed with which this vaccine was developed. In contrast, for perhaps the most famous vaccine in modern times, the Salk polio vaccine, took 10 years to develop. Polio was so feared that parents refused to let their children attend summer camp (it struck mostly in the summer). One epidemic after another swept through the US, causing paralysis (although only a small percent of the time) and sometimes death. The vaccine was so eagerly anticipated that when positive results were announced, church bells rang across the county.
The extraordinary breakthrough on Ebola was a result of collaborative efforts of doctors, drug companies, scientists, governments, universities, and funders, such as the Wellcome Trust.
But, the trials were considered to be so risky that no one wanted to conduct them. The WHO had to take charge. Dr Marie-Paule Kieny, the assistant director-general of the WHO said, nobody wanted to step into this role so we took the risk ¦ We believe that the world is on the verge of an efficacious Ebola vaccine.
Dr. Josh Bloom, the director of chemical and pharmaceutical sciences at the American Council on Science and Health said, I ve never seen anything like this. The rapid discovery and preparation of this vaccine shows what can happen when governments, agencies, companies, and medical research centers work together. It was less than a year ago when the US was in panic mode, as the CDC botched just about every effort to prevent the virus from entering the US. Now, ten months later, it s solved. A tip of the hat to all involved.
He quips, This might be a really good test of the belief system of anti-vaxxers. I ll chip in to buy Mike Adams a one-way ticket to Sierra Leone, and then we ll see how confident he is about his conspiracy theories concerning vaccines. Perhaps he would simply try to build his immune system with one of his supplements.
He quips, This might be a really good test of the belief system of anti-vaxxers. I ll chip in to buy Mike Adams a one-way ticket to Sierra Leone, and then we ll see how confident he is about his conspiracy theories concerning vaccines. Perhaps he would simply try to build his immune system with one of his supplements.
How valid are the data?
While there is no question that the vaccine works the circumstances under which the trials were conducted were far from ideal, concludes, Katie M. Palmer, writing for Wired. Her article, What 100 Percent Effective Means for That Ebola Vaccine discusses the statistical weakness in the vaccine trials.
Palmer explains, Based on the vaccine s early success, the trial s runners decided that all participants in the study should get it immediately after exposure. That s a perfectly reasonable, humane reaction, but it also means that the researchers will never be able to collect better data on the vaccine s efficacy.
In other words, in the absence of a placebo group, it is really hard to tell how effective the vaccine really was, because it is impossible to tell how many people who did not get the vaccine would have caught the virus, especially since some of the areas in which the vaccine was tested were already experiencing a waning of the epidemic. Additionally, the differences in how the trials were run make direct comparison difficult. The trials in Guinea and Sierra Leone were designed to answer different questions.
Dr. Bloom comments, There is a tradeoff in this case, but the price that is paid incomplete knowledge about how effective the vaccine was pales by comparison to the benefit of vaccinating as many people of possible. It would be unethical and inhumane to withhold the vaccine from anyone who was at risk of being infected in the middle of a public health crisis, especially since there are no other therapeutic options.
How should the vaccine be funded?
Having a successful vaccine available in a poor area, where most, if not all, people need to get it, raises another question: who is going to pay for it?
This question is addressed in a new perspective piece in the New England Journal of Medicine, in which lead author Dr. Stanley Plotkin noted that prior to the current vaccine, there were at least seven other encouraging candidates that had been studied in monkeys, all of which were abandoned.
Plotkin says, vaccines against them are not available because collectively we have not been willing or able to invest in the costly and complex development process that would be required to establish safety and immunogenicity, at a minimum.
He calls for a $2 billion seed money fund with contributions from governments, foundations, the pharmaceutical industry, and nontraditional sources, perhaps including the insurance and travel industries, and draws a parallel to the proposed $2 billion antibiotic-resistance fund. Research in both areas is badly needed.
Plotkin s take home message is that it is far better be proactive: The lesson we take from the Ebola crisis is that disease prevention should not be held back by a lack of money at a critical juncture when a relatively modest, strategic investment could save thousands of lives and billions of dollars further down the line.


