An Everyday Symptom Hides a Deeper Story
Constipation—often dismissed as a minor inconvenience—affects millions and can quietly erode daily comfort and well-being. Clinically defined as fewer than three bowel movements per week, it affects roughly 14% of the population, with higher rates among women, older adults, and people with Parkinson’s disease. In many cases, stool moves too slowly through the colon, allowing excess water to be absorbed and leaving it hard and difficult to pass. Beyond discomfort, chronic constipation also carries economic costs, estimated at $1,500 per person annually, and contributes to more than $1.5 billion in over-the-counter sales.
But in some patients, constipation is more than a routine digestive slowdown—it may be an early signal of something deeper.
Rethinking the Roots of Constipation
In Parkinson’s disease, constipation emerges years before the classic motor symptoms appear. This striking temporal relationship suggests that constipation might reflect early neurodegenerative changes. However, Parkinson’s traditional dopaminergic therapies provide little relief from constipation, implying that impaired motility, the classic “causes” of constipation, cannot fully explain the problem. Prokinetic drugs frequently fail to provide durable relief, suggesting that mechanisms beyond simple transit delay are involved.
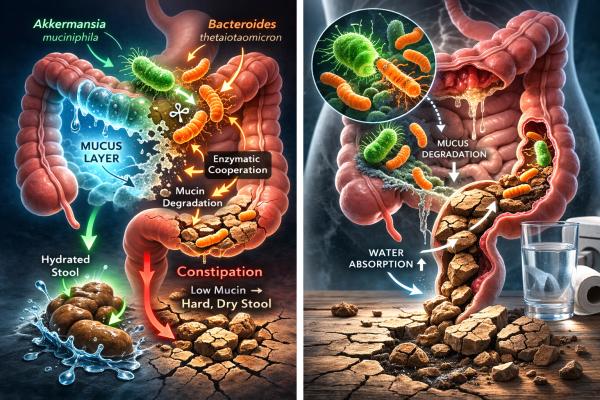
Another crucial player in this story is the intestinal mucus layer. This gel-like coating hydrates and lubricates stool while protecting the intestinal lining from mechanical stress. Its structural backbone is mucin, a large glycoprotein that gives mucus its slippery consistency and water-retaining properties. If the quantity or composition of mucin changes, stools could become drier and more difficult to pass.
If the mucus layer helps keep stool soft, what happens when something begins to erode it?
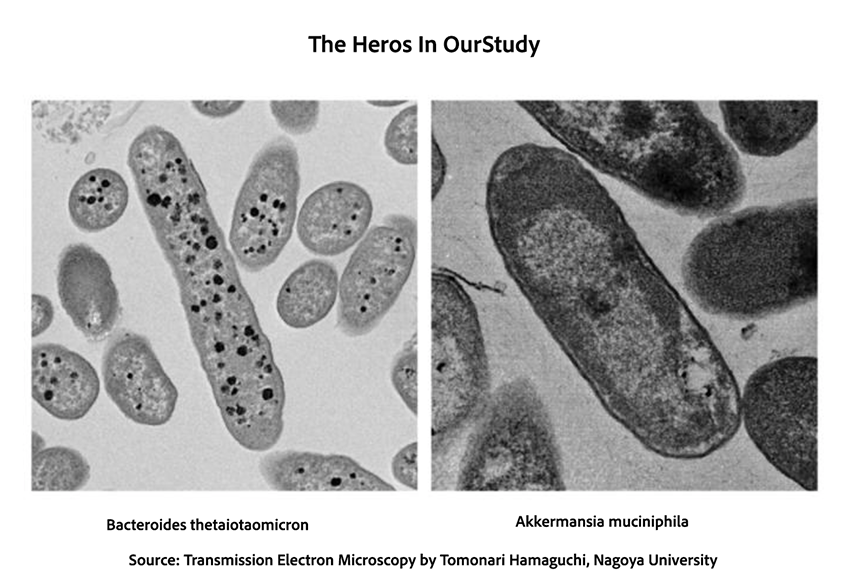 Constipation alters our bowel flora, leading the investigators to another potential culprit: Akkermansia muciniphila, a bacterium found in higher abundance in people with Parkinson’s disease and associated with firmer stool and slower transit. As its name suggests (muciniphilia = mucin-loving), it feeds on mucin. However, it cannot completely digest colonic mucin on its own. Another common gut resident, Bacteroides thetaiotaomicron, possesses the complementary enzyme needed to finish the job. Together, the two form a potential partnership.
Constipation alters our bowel flora, leading the investigators to another potential culprit: Akkermansia muciniphila, a bacterium found in higher abundance in people with Parkinson’s disease and associated with firmer stool and slower transit. As its name suggests (muciniphilia = mucin-loving), it feeds on mucin. However, it cannot completely digest colonic mucin on its own. Another common gut resident, Bacteroides thetaiotaomicron, possesses the complementary enzyme needed to finish the job. Together, the two form a potential partnership.
This reasoning led to the hypothesis that constipation, at least in a subset of patients, may be driven in part by “the multitudes” within our microbiome, rather than by motility defects alone.
The findings of the research were based on fecal samples collected from patients with Parkinson's disease, patients with chronic idiopathic constipation (constipation without a known cause), and healthy controls.
The Chain of Evidence
- Clinical Observation in Humans: In analyzing participants' fecal samples, they found higher levels of both A. muciniphila and B. thetaiotaomicron, along with significantly lower levels of fecal mucin, that lubricating protein that keeps stool hydrated. Statistical analysis indicated that the reduction in mucin was more closely associated with constipation than Parkinson’s Disease.
- Testing Bacteria in Mice: To determine whether these bacteria caused the problem, researchers used “sterile” mice raised without bacteria (gnotobiotic). When colonized with either bacterium alone, they did not develop constipation, and their mucin levels remained normal. However, when colonized with both, the mice recreated the human phenotype, developing constipation with less stool moisture, depleted fecal mucin, and fewer fecal “pellets.”
- Ruling Out Host Dysfunction: By analyzing the mice's colonic tissues, the researchers confirmed that the mice were not producing less mucin; the genes responsible for making and secreting mucus were functioning normally. The bacteria were simply consuming the mucus faster than the body could replace it. They were “cooperating” with one another.
- Proving the Mechanism: To confirm the role of this enzymatic cooperation, researchers created a mutant strain of B. thetaiotaomicron lacking the missing enzyme. Mice with both A. muciniphila and the mutant did not develop constipation, and mucin levels and stool hydration returned to normal.
The authors propose that a form of “bacterial constipation” may occur when microbial cooperation accelerates degradation of the colonic mucus layer, reducing lubrication and hydration and contributing to harder stools.
From Mechanics to Ecology
For decades, constipation has been framed as a mechanical or neurologic problem, but this work highlights that in at least some patients, constipation may also represent a biologically driven ecosystem disturbance. This study is valuable not simply because it identifies two bacteria associated with constipation, but because it exemplifies a broader shift in medicine: we are increasingly recognizing that the gut microbiome is not a passive passenger, but an active participant in human physiology.
The mucus layer, once viewed mainly as a protective coating, becomes a dynamic interface that our multitude within can modify or exploit. Constipation, traditionally considered a functional disorder, is reframed as potentially having a microbial subtype, driven by biochemical cooperation between bacterial species.
The work underscores how much remains unknown. The microbiome is extraordinarily complex, and identifying two organisms is only a small window into a vast network of interactions. It is still unclear how broadly these findings apply across the heterogeneous population of constipated patients, or whether these microbial patterns are causes, contributors, or consequences in different clinical contexts. Even the mucus layer itself, central to many of our gut reactions, remains incompletely understood in terms of its regulation, alterations, and microbial adaptation with age, diet, medication use, or disease.
The microbiome is not a collection of isolated organisms but an interdependent system. Any attempt to alter it may produce effects that ripple through the ecosystem—and through you and me, its human hosts.
Source: Bacterial constipation: Mucin-degrading intestinal commensal bacteria cause constipation Gut Microbes DOI: 10.1080/19490976.2025.2596809


