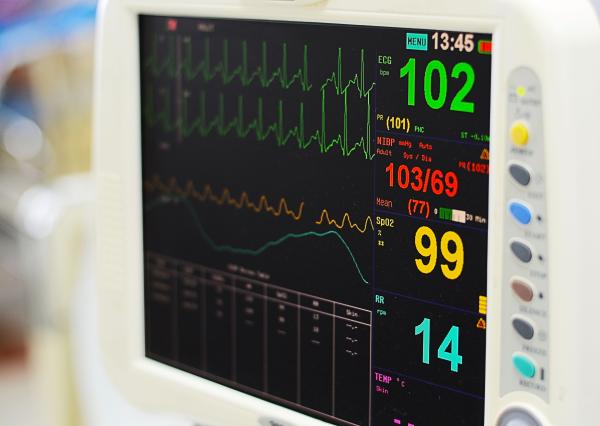
All too frequently, the things we do daily become routine. This is likely true of many tasks in a multitude of professions. It’s just that in certain fields, like medicine, seemingly mundane and tedious duties can—all too often— provide the most valuable knowledge of a patient’s well-being and genuine health status.
Vital signs matter. They matter most when done correctly and provide accurate data. Hence, why they are likely called “vital” signs.
Dismiss them or do them incorrectly and the bad information obtained will guide medical decisions on your behalf-- potentially toward a negative trajectory. Now, with electronic medical records, especially, this erroneous information will follow you and your future care may be directed based on these false results.
As I always say in healthcare, good information is priceless and an often proactive measure. Bad information can do harm. It is worse than no information.
Due to the extensive number of people involved in a patient’s care before even encountering the physician, great variability in conscientiousness and thoroughness abounds— no matter how “renowned” a facility or “well-regarded.” Institutions are only as strong as their weakest link and with an ever fragmenting health system being your own advocate in your care is becoming essential. (To learn more about optimizing your care, read my guide here: 10 Ways to Save Your Life or the Life of a Loved One).
Like with any vocation, you will encounter mostly stars and, hopefully, only a handful in the mix who opt to phone in their work. The difference in healthcare is the fact that whichever type of cog in the caregiving chain you encounter will record your specifics—reliable or not—and they will be interpreted as facts by physicians. Your treatment will be guided by that knowledge.
So, let’s dive into why letting a medical assistant or nurse or whomever take your vital signs correctly is so important. Don’t let inconvenience and annoyance usurp the big picture.
Why do we take Vital Signs?
The core vital signs of heart rate, blood pressure, temperature and respiratory rate (aka breathing rate) reflect a person’s level of wellness and severity of illness in that moment in time. When normal, these non invasively obtained values convey overall health and can provide needed reassurance while symptomatic or monitoring while on medication. When not, they guide level of urgency and inform regarding the need for aggressive intervention. They serve as a red flag which prompts a cascade of assessment that can compel early diagnosis or avert an impending status change.
When these quantities are known and performed correctly, they benefit acute and chronic disease treatment course, management and prevention. Trends over time advise a physician of an individual’s personal baseline and disease or illness progression and even drug influence. As norms are highly variable between gender, age, pre-existing medical condition and certainly when taking particular medicines, for instance, we know when situations have gone awry.
These numbers in the context of a comprehensive physical examination and history of a patient tell more about the basic functioning of organ systems than many unnecessary more invasive tests or studies. Areas of our central nervous system control our respiratory drive that allows for the effort to be made in the first place. Our level of hydration and effectiveness of our cardiovascular system are interpreted by these values. Blood volume and kidney condition can be initially apprised via collection of this data. The list goes on to illustrate their usefulness.
Heart Rate
Why do we take the heart rate? Believe it or not, it speaks volumes beyond one’s cardiac status. A rapid heart rate can trigger identification of a metabolic or endocrine issue like an overactive thyroid— one that can be easily corrected when understood as the etiology (aka cause). It can indicate a profound anemia that has incited the heart to pump faster to accommodate the blood loss. This might be a result of an adverse drug reaction, illicit or otherwise. And, of course, it as well as a slow heart rate can represent a primary and/or secondary problem of the heart (eg. an arrhythmia or even head trauma).
The movies always drive me bananas when I see the actor use his thumb to measure a pulse of a sick character. Your thumb has a pulse of its own, so not a preferred technique. The heart rate can be taken at the site of different arteries like the wrist or neck, for example. Listening to the heart itself with a stethoscope can achieve this as well.
Blood Pressure
Like our other signs, we know what is normal and what is not and when circumstances appropriately influence this value. There are times when all four extremity blood pressures inform, like in certain congenital heart defects. Central nervous system damage can antagonize levels. Of most critical import, is the recognition that this measure is a crucial tool in the health care provider arsenal.
When improperly obtained, the result is useless. When a tech or staff member attempts to take it over your sweater and coat, say “no thank you.” You get it done right, or don’t do it as that number will forever be carried along in your medical record and could negatively serve you. If the cuff barely fits around your bare upper arm and is about to burst open on first pump of the bulb, then you have the wrong sized cuff and the blood pressure will be inaccurate. If the result is so unusual for you and has been performed by an automated cuff, then requesting it be repeated manually is in your best interest, in particular, if time allows.
High blood pressure can be an indicator of more advanced heart disease. Or, kidney. And so forth… When it is low, dehydration can be the culprit. (1)
Temperature
Our bodies are extraordinary machines. When intact, they can maintain equilibrium in the craziest of circumstances. They have innate mechanisms to regulate our temperature. Early immune response can be represented by an escalation of it when in the face of an infection. Spinal cord injuries can impede your body’s ability to control it and repercussions ensue.
Drinking hot tea or a very cold drink right before taking a temperature is ill-advised. Unless you want to scare yourself or a health care provider unnecessarily and complicate things. As is arriving to your pre-operative clearance wearing many layers having run up four flights of stairs and permitting your temperature to be taken instantly upon arrival. Same with bundling your baby and practicing taking his temperature when there are no symptoms. In the former, a transient elevation could confuse the clinical picture and delay your procedure. In the latter, fever is taken very seriously in a newborn infant and could spark invasive tests when unbundling could be the simple answer. Recognize that “practicing” can do potential harm. The safest measure is to perform tasks when there is a reason to do so and in consultation with your pediatrician. Less can be more.
Hypothermia (aka temperature too low) and hyperthermia (aka temperature too high) along with normalization of core body temperature provide distinctive clues to primary problems and following their path aids in understanding of presence or absence of resolution.
Again, good data is wonderful. Bad data is worse than no data.
Respiratory Rate
This can be appreciated as simply as watching the chest rise and fall. Too fast a count can imply distress. It is a critical value when under anesthesia, in intensive care, being treated for asthma or pneumonia. A suppressed respiratory drive can be caused by narcotics, for instance.
Knowing norms in all life stages and with certain illnesses is key to interpreting properly severity of sickness. Along with gathering a patient’s pulse oximetry recording (aka another vital sign acquired by a finger probe device) these can allow for the evaluation of your oxygenation status. Are you getting enough? If not, why? And, the algorithm to solve the issue gets employed. Just be sure the value of your pulse ox result is recorded along with whether you are breathing room air or are on 100% oxygen. Each impacts the utility of the data.
In summary…
Additional indicators like weight, height, body mass index (BM), pain scales, Glasgow Coma Scores and monitoring your ins and outs with respect to fluid and urine are essential to continued interpretation of the core vital signs. Daily weights are crucial to proper management of the patient in congestive heart failure while accurate ones are necessary for correct dosage calculations in the pediatric set, those with kidney and liver disease and so forth. Don't take it while in winter gear and snow boots. Precisely timed and accumulated blood pressures and heart rates while lying down, sitting and standing (aka evaluating for postural or orthostatic hypotension) are imperative when assessing a patient’s fall risk.
Insist on good data in your health care. It is a high-priority in ensuring yours and your loved one’s well-being as you navigate the health care system. Your present and future doctors, nurses and care givers will appreciate it!
Notes:
(1) ACSH’s medical fellow, Dr. Kedist Tedla, recently wrote about the consequence of unequal blood pressures in the upper extremities, click here to review.