In Personalizing Nutrition - Automating The Science of Metabolomics and Personalizing Nutrition - Metabolomics and Glucose, I discussed the idea that our metabolic response to a meal, what is described as phenotypic flexibility, is a measure of the interaction of glucose, fat and protein metabolism. And that our metabolism is perhaps better measured by a standardized, test meal that mimics what we really eat as compared to solely the 75 grams of sugar found in an oral glucose tolerance test.
But can we use the metabolomics data of phenotypic flexibility in truly creating a more personalized, therapeutic diet? Consider the following paper, Personalized Nutrition by Prediction of Glycemic Responses
800 healthy and pre-diabetic individuals had a device implanted which allowed measurement of their blood sugar every 5 minutes for a week. [1] A quick note before we continue, the next part is complicated and requires some attention, if you prefer, this is a short video that summarizes the paper and its findings.
They begin by pointing out that no current method predicts the postprandial glucose response (PPGR) – that is, how eating food A or B might change our blood sugar. And that most diets directed at diabetes make recommendations based on carbohydrate content alone (the traditional American Diabetes Association, ADA diets) or perhaps the trendy glycemic index of the particular food.
They found that the PPGR was very reproducible for individuals eating the same foods frequently. Good, now we know that the test is reliable. They also found that for a given food, there was a high variability in PPGR between individuals – that is, for some people bread caused a glucose spike and for others, not so much. (Spoiler alert, pizza may be coming back)
The full dataset, the diet, the blood sugar response and the demographics were used to create a machine learning algorithm to predict PPGR. When the subjects were fed a standardized meal, predicting PPGR using models involving total calories (ADA diets) or even specific carbohydrates (glycemic indices) resulted in a 33 to 38% correlation with PPGR. The machine algorithm had a correlation of 68%. [2] Their computer algorithm was then validated using a one hundred person cohort, and a 70% correlation was achieved.
Most germane to our discussion the study found that some individuals were more sensitive to an equivalent amount of carbohydrates than others that increasing fat content, in general, reduces PPGR So, looking at an isolated element, blood sugar, is insufficient. You need to consider a more realistic meal in making nutritional recommendations.
In the final part of the study, the researchers created six iso-caloric diets based on algorithmic machine predictions that were ‘good’ and another six diets that were ‘bad’ in controlling PPGR. A registered dietitian, basing recommendations on the patient’s monitored data, created two sets of six iso-caloric ‘good’ and ‘bad’ diets. One treatment arm ate the algorithmic diets, the other the dietitian recommended diets, for two weeks. After one week ‘good’ and ‘bad’ diets were switched in each treatment arm. Participants were blinded to both the treatment arms and the diet they were eating in week 1 or 2. In both instances, ‘good’ diets resulted in less blood sugar fluctuation and a lower maximum.
So a more personalized diet, based on metabolomics resulted in better PPGRs whether designed in a bespoke manner by a dietitian or in a more automated way by a machine. And 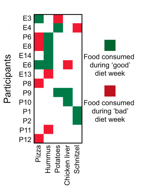 the final fact, I promised a few paragraphs ago – a good food component for some was a bad element for others. There it is in that first column, pizza good for some, not for all. (Yes, I see hummus in the next column, but really, hummus over pizza?)
the final fact, I promised a few paragraphs ago – a good food component for some was a bad element for others. There it is in that first column, pizza good for some, not for all. (Yes, I see hummus in the next column, but really, hummus over pizza?)
To answer the original question, yes, personalized nutritional advice can bring about better glucose management. And yes, it is possible to automate the process, using a machine generated algorithm, to scale the recommendations (increasing utilization will mean decreasing cost).
In Personalizing Nutrition - Automating The Science of Metabolomics I noted two companies that claimed to be providing scientifically personalized meals. Habit claimed to be more tailored and, based on my explanation here and in Personalizing Nutrition - Metabolomics and Glucose, it seems Habit’s nutritional advice does have the real possibility of being useful, with two additional caveats.
First, other studies have demonstrated that personalized dietary advice based on ‘individual dietary intake’ along with phenotypic and genotypic information is no better than advice based on individual dietary intake alone. That makes Habit’s use of genotypic information a bit more problematic.
Second, while the website does reference specific genetic variants that can affect sugar, fat, and protein metabolism in conversation with their scientists this information is used more to justify the recommendations stemming from the metabolic challenge than in formulating the recommendations in the first place.
How does Habit claim to work?
An Oral Glucose Tolerance Test (OGTT) requires an individual to go to a laboratory, drink their 75 grams of glucose and have blood drawn. Fairly inconvenient. Habit’s metabolic challenge is done at home. The genetic information comes from a swab of your cheek and the blood work is sent via a blood collection card which uses blood from a finger stick. The card separates the plasma and metabolites into a separate layer. These cards are reasonably accurate – around 97%. The cards and swab are then mailed to their reference laboratory. Once they have the results, a nutritional report and recommendations are made. These are presented and discussed with you by a registered dietitian. Habit will provide meals, specific to what they determined using their algorithm. [3]
What is the bottom line here? Habit is using a metabolic challenge drink to make nutritional recommendations. While the initial market is people seeking an edge in their health, the model has the potential to be very scalable and thus available to many individuals at a lower cost. If this holds up in the real world the way they claim it does in the laboratory then I think Habit demonstrates a valid path. A method that can be done at home, without first obtaining a physician’s prescription, without driving to a blood collection facility, may be a way to overcome that ‘last mile’ in dietary healthcare and facilitate getting useful nutritional information to people.
NOTES:
[1] Additionally they measured blood parameters, anthropometrics, physical activity, and self-reported lifestyle behaviors, as well as gut microbiota composition and function.
[2] Because the measured correlation of PPGR for the standardized meal for an individual when repeated (its reproducibility) was 71% the authors felt that the machine model correlation was near its possible limit.
[3] Habit is currently limited to the Bay Area in California during its rollout. Meal prices are comparable to those from the other websites offering prepared food or meal ‘kits.’




