Mental illness still carries a stigma in society, particularly for those who suffer from a severe form, such as schizophrenia or bipolar disorder. High-profile incidents, in which a mentally ill person commits a violent crime, has led to the stereotype that the mentally ill pose a dire threat to society.
It is certainly true that rates of violent crime are higher among the severely mentally ill than among the general population, with approximately 5 to 10% committing an act of violence within 5 years of diagnosis. Still, the vast majority of them never do so. The question, then, is how psychiatrists can identify the subset of patients who are most likely to become violent. Some risk assessment tools already exist, but most are either unreliable or overly complicated. Now, a team of researchers, led by Dr. Seena Fazel, has developed a model that accurately predicts which patients are unlikely to become violent.
The team collected data on 75,158 Swedish patients aged 15 to 65 who suffer from schizophrenia or bipolar disorder. Some of these patients committed a violent crime within one year of being discharged from a hospital or meeting with a psychiatrist. The model that the researchers built was based on a multiple regression of 16 different variables, such as socioeconomic status and drug use.
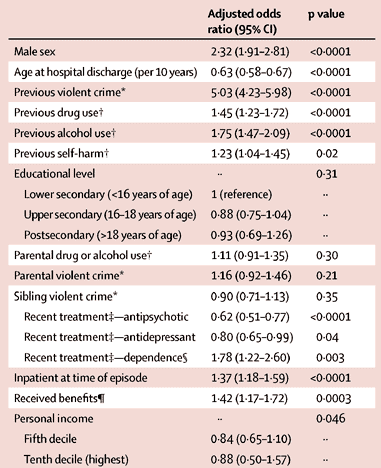 Dr. Fazel's team found that two factors greatly increased the likelihood that a severely mentally ill person would commit a violent crime: A history of violent crime (which increased the risk five times) and being male (which more than doubled the risk). On the flip side, the older a patient is, the less likely he or she is to commit a violent crime. (See chart.)
Dr. Fazel's team found that two factors greatly increased the likelihood that a severely mentally ill person would commit a violent crime: A history of violent crime (which increased the risk five times) and being male (which more than doubled the risk). On the flip side, the older a patient is, the less likely he or she is to commit a violent crime. (See chart.)
Other factors that were statistically significant but had a smaller impact on the risk of violence included prior alcohol or drug use, previous episodes of self-harm, and being an in-patient. It should be kept in mind, however, that these factors may not cause violence but rather serve as proxies for the severity of mental illness. Indeed, mentally ill people often "self-medicate," and severely mentally ill people are more likely to be hospitalized or institutionalized.
Importantly, the model had a negative predictive value of 99.5%. That means if the model predicts that a particular patient is unlikely to commit a violent crime, there is a 99.5% chance that the prognosis is correct. In other words, as the authors write, "of those identified as low risk, 199 of 200 did not in fact offend violently within 1 year."
Unfortunately, the positive predictive value was only 11%. That means if the model predicts a patient is likely to commit a violent crime, there is only an 11% chance that the patient actually will do so. Further research will be needed to improve this aspect of the model.
Identifying with accuracy those severely mentally ill patients who are probably harmless will allow psychiatrists, public health officials, and law enforcement to focus their limited time and resources on higher-risk patients. Thus, this model is a tremendous step forward.
Source: Seena Fazel, Achim Wolf, Henrik Larsson, Paul Lichtenstein, Susan Mallett, Thomas Fanshawe. "Identification of low risk of violent crime in severe mental illness with a clinical prediction tool (Oxford Mental Illness and Violence tool [OxMIV]): a derivation and validation study." Lancet Psychiatry. Online first. Published: 4-May-2017. DOI: 10.1016/S2215-0366(17)30109-8




