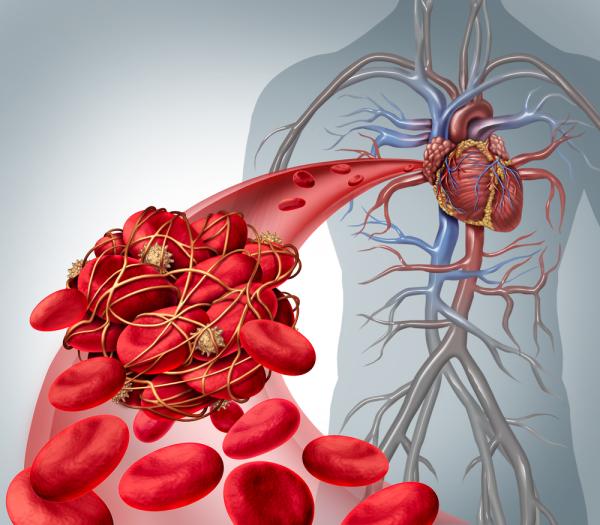
To be able to clot our blood is an extraordinary capability. However, too much of a good thing poses its own risks. Reducing your chances of developing pathologic clots will be addressed here.
According to the Centers for Disease Control and Prevention (CDC), blood clots adversely impact nearly 900,000 Americans and prompt roughly 100,000 premature deaths annually. Specifically, they recognize those presenting as deep vein thrombosis (DVT) and/or pulmonary embolism (PE) among the most substantial threats to public health. (1)
Our innate coagulation (aka clotting) cascade is quite a dynamic, but formidable system. When optimally effective, it initiates and manages retention of a balanced condition between not too much bleeding and not too much clotting. A steady state, if you will.
This permits us to heal from wounds when we experience trauma, albeit in nature or via surgical intervention. By first stopping the bleeding, it provides the essentials to repair the damaged vessel or injured anatomy. As a result, this involves a complex web of factors and influences that oversee the delicate dance to keep the seesaw between excessive bleeding and clotting equilibrated.
Avoiding too much or too little clotting and bleeding is its mission. When there is imbalance or impairment of a critical component to this cascade, a blood clot can become a hazard; for, not only can it locally impair blood flow —thereby halting delivery (partially or entirely) of vital nutrients like oxygen to tissues, but it also can travel elsewhere in the body. Where it impedes flow determines the extent of damage, how life-threatening and how aggressive medical measures can be.
For example, a pulmonary embolism involves the lung and respiratory tract. A major clot can be catastrophic in this location depriving the individual of being able to breathe and effectively take in oxygen. Death can be a consequence, especially if identification and appropriate intervention is delayed. In some circumstances, even that successfully achieved can’t prevent an untoward outcome.
Treatments exist to halt extension of clots and their menacing progression. They, too, entail frequent surveillance (e.g. blood testing, imaging modalities) to be assured they are not contributing to advancing the other extreme of bleeding, for instance. In a nutshell, they have their own risks. Often the alternative can be worse, so the benefits of them typically outweigh the risks.
And, this in itself is good news because it means a clot was actually diagnosed in a timely fashion to spare and preserve a life. In profound scenarios of clots that straddle the major airways or lead to severe brain ischemia (aka lack of oxygen to tissue due to blockage of blood flow), early diagnosis and intervention are life-saving and life-altering.
That said, the best offense in this health care realm is to avoid the clot entirely. Preventing one from happening is in your best interest.
Let’s review some key associations that should trigger conversations with your doctors about how to avoid this often preventable complication:
Hospitalization for Disease, Major Trauma or Surgery
Prolonged hospital stays where a person is immobile for a protracted period of time enhance one’s chances of forming a clot. Depending on the condition and clinical course, a patient is not risk-free once discharged. Awareness of symptoms or signs and close monitoring is as important upon release as it is while admitted— and, sometimes for months to follow.
Major orthopedic surgeries involving the pelvis, hip, or knee as well as abdominal ones pose the greatest risk of clot development. It is not just the surgery itself that triggers this, but is compounded by the principal injury if physical trauma was the culprit. Was it a severe accident? Were their major vessels injured or bones? Is the individual confined to a wheelchair or bedridden? If so, then for how long?
The post-surgical course can require the use of blood thinners to avoid this situation as well as getting the person out of bed as early as possible when safe to do so. To review the potential issues and the considerations of the surgeon after an operation, see Bill Paxton Dies of Surgical Complications.
Pregnancy and Postpartum Period
In general, pregnancy is considered a hypercoagulable state—one where a person is at higher risk of developing thrombosis (aka clots) in one’s blood vessels. This concern persists weeks after delivery. So, signs of shortness of breath in a new mom or swelling of the arm or leg without a known event should be evaluated with potential blood clots in mind.
Immobility
This covers a wide spectrum. As previously described in the hospital stay/surgery section, any medical condition that warrants confining poses a risk. As does sedentary living, in general, but in particular when sitting for long periods without uncrossing legs like in extremely long car rides or when flying. It is very important to make frequent stops in the former and walk around, while getting up often in flight and taking a stroll in the aisle is also crucial. Some need go a step further and take prophylactic medication if they had a prior clot or have a profound family history.
Modifiable Risk Factors
Smoking is a risk factor for clots. As is being overweight. Birth control or hormone therapy with estrogen raises one’s risk which is why it is paramount to let your doctor know if you are also a smoker or have a significant personal or family history of clots. Inactivity does not have to be a perpetual state of being. Shifting to a more active, healthy lifestyle benefits us all not just with respect to clots, but with respect to improving a host of physical conditions as well as our mental health and well-being.
Being 55 or older is associated with a greater risk and though it is not modifiable to change our age, taking charge of not doing what is modifiable is definitely within your control. And, will limit your burden if in this population.
Family and Personal History
Those with a known personal or family history of clots or clotting disorders need be especially careful. First, knowing the specific issues within your family will best guide your surgeon or regular physician to prevent such problems and avoid exposing you to certain dangers. Second, this understanding will guide your decisions so that you don’t unnecessarily add to this risk factor. For example, someone with a notable family history should even more so avoid smoking and being immobile.
Chronic Diseases like Cancer or its treatments, Heart or Lung Disorders, Diabetes
For these and more conditions, lengthy discussions with your care provider should take place so as to minimize the possibility of this complication and take steps to avoid it entirely. Close observation might also be vital. Treatments and medicines themselves can also be a compounding influence, so a comprehensive history is critical to eliminating problems or preventing their progression.
In Summary...
Though anyone can be at risk of developing a blood clot, the aforementioned should give food for thought and encourage you to have the discussion with your doctor to improve your lifestyle, assess your personal risk and learn ways to prevent clots especially in the context of requiring hospitalization or disease management.
It is also very important to talk about signs and symptoms that could be worrisome. Among them include but are not limited to the following: difficulty breathing, chest pain especially on deep inspiration, rapid or irregular heartbeat and pain or swelling of your arm or leg in particular when no known injury occurred as well as redness, discoloration or warmth to the skin. (2) Seeking emergent medical care is integral to improving your odds of a successful outcome. It is remarkable what can be done today to intervene.
Note(s):
(1) In the CDC’s “Stop the Clot, Spread the Word” campaign, they attribute blood clots to about 1 in 10 hospital deaths. Additionally, they report about 1/2 of all clots take place within 3 months of hospitalization or surgery and estimate about 50% lack proper prevention approaches.
(2) The following infographics and materials are wonderful resources: National Blood Clot Alliance (funded by CDC) or here.



