The findings are from the National Poll on Healthy Aging, a survey of a “randomly selected stratified group” of adults administered by phone or online. The results of the 2,163 participants were then scaled and weighted to reflect the population of the US as determined by the Census Bureau.
The poll asked questions found within the Yale Addiction Scale, a means of assessing, in the words of the developers, “signs of addictive-like eating behavior.” [emphasis added] The Diagnostic and Statistical Manual of Mental Disorders (DSM), currently in its fifth edition, is the repository of all mental health diagnostics. A few years ago, psychiatrists split addictions into two categories, addictions to substances, i.e., opioids or cocaine, and addictions to behaviors, notably gambling.
A “diagnosis” of addictive eating is based on the finding of three or more “symptoms” and evidence of clinically significant distress or impairment. The use of quotation marks in this last sentence is directly from the developers of the scale.
Here are the results of their poll. I have grouped, by color, questions aimed at similar concerns.

The most frequently noted symptoms, noted in green, were cravings for particular foods. 75% of us do not even have cravings, so can these “highly processed” foods be that addictive? It is reminiscent of the narrative of hell’s gateway, "reefer madness" in the 30s, and the prescription of opioid madness of today. The two questions in light red denote clinical distress or impairment, the source of 13% or 1 out of 8 of us. The Yale Addiction Scale would say that 13% reported a “mild” food addiction. These caveats suggest that the headline that 13% of us are addicted to highly processed foods is too sure of itself. [1]
The poll noted that women were twice as likely to meet the criteria for addiction to highly processed foods. But men are 25% more likely to be obese. Perhaps women are a bit more forthcoming in this self-reported poll, or have the social forces of marketing made them more self-conscious?
“Meeting criteria for addiction to highly processed food was also more likely for older adults who reported often feeling isolated from others (women 51%; men 26%).”
Could we argue that eating is a comfort for isolation and not an addiction? The authors of another poll on overeating point out, “It might not be that women and men view eating differently but rather that emotional eating is a more common coping mechanism for women.” And an additional study suggested that men and women differ in their comfort foods. Males chose “ warm, hearty, meal-related comfort foods (such as steak, casseroles, and soup), while females instead preferred comfort foods that were more snack related (such as chocolate and ice cream).” [2]
That 13% headline regarding our food addiction is meant to gather more attention than educate. But let’s spend a few moments discussing the idea of food addiction. For that, I looked at a review (see Sources) on the topic. Food addiction doesn’t fit easily into those two DSM categories of addiction; is food addiction a behavior or substance abuse?
There is no consensus, no settled science, on the possibility of food addiction because it is unclear what role food has in triggering “addictive behaviors,” and from a practical point of view, how will viewing it through the lens of “addiction” result in “beneficial change.”
The authors of the review suggest several agreed beliefs:
- Obesity has many roots -“Obesity is a heterogeneous disorder; addictive-like eating behavior is of clinical relevance for a subgroup of people with obesity” who display an “addictive phenotype.” [3]
- Obesity shares a reward system with other addictive behaviors - “Mechanisms implicated in substance-related and addictive disorders (e.g., reward functioning, executive control) play an important role in overeating.” But these Skinner-like mechanisms do not occur solely in those with obesity, and the APA has declined to classify obesity as an eating disorder.
- How and what we eat matters - The attributes of the food, individual differences, and the behavioral patterns of consumption contribute to addictive-like eating.
- The food industry is uniquely positioned - There are many contributing factors, including lower physical activity, but the food industry can “improve the dietary quality of foods” and nudge people through marketing towards healthier choices.
Much of the controversy revolves around a few key issues.
- Highly processed foods and addictive potential – One side argues that the combination of “rapidly absorbed carbohydrates (high glycemic index) and fat underlie the addictive nature of these highly processed foods, which is further enhanced by salt and other flavor additives.” Others argue that evidence of that effect is lacking and that in this most recent survey, 87% of individuals consume these addictive foods “without experiencing drug-related effects.”
- Operationalizing “food addiction” to evoke change – Some emphasize a substance addiction, which like other addictive substances, requires special labeling and regulation over their availability and use. Others emphasize a behavioral addiction, requiring better education and nudges, like taxing sugary beverages, removing “sweets” from schools, or reducing marketing to “vulnerable” populations.
- A scientific consensus on “whether a substance or behavior is addictive.” – There is no settled science on addiction. Misclassifying substances have the potential for great harm, as we have seen in the war on opioids, where many individuals were receiving high doses of addictive drugs and leading fully functioning lives without a trace of detrimental behavioral addictions. Misclassifying behavior has a similar potential and underlies our discussion of whether obesity is a disease.
Final thought
Could it be that our expanding waistlines are not due to addiction or Big Highly Processed Foods but to our inability to deal with abundance? Could our weight gains reflect that we are awash in calories? Here is a graph from The World in Data. In the last 60 years, we have increased our calories by roughly 30%. I doubt that our physical activity has kept pace. In the same interval, China doubled its daily supply of calories. China conducted its first nutrition and health survey in 2002 and found a rising rate of obesity that began in 1980, especially in the cities where calories were abundant, and public transportation and automation had reduced the number of calories expended in activity.
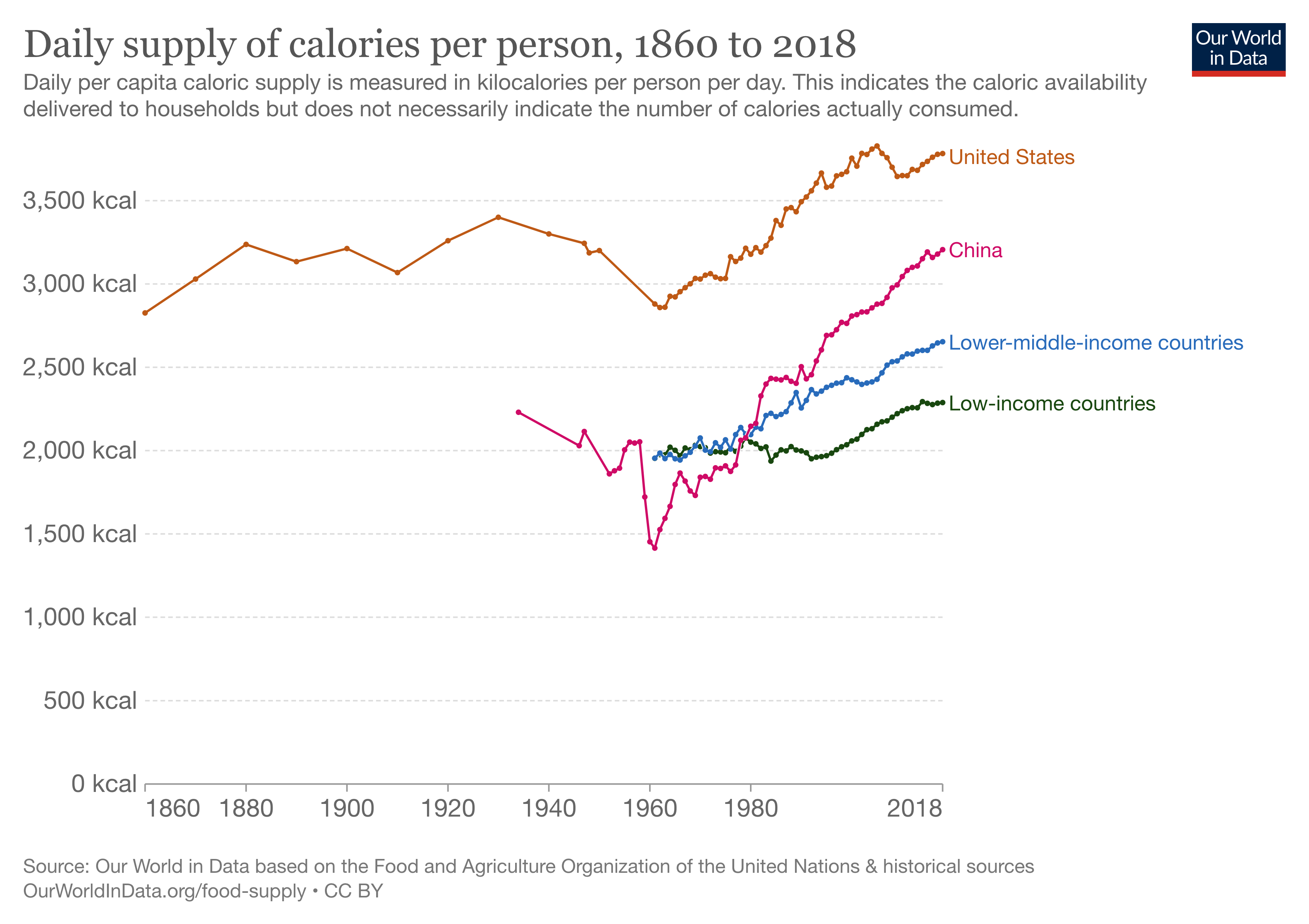
There is a clear association between our expanding waistlines and our expanding sources of cheap calories. Maybe thinking about food addictions is entirely wrong. What if we are like other living creatures, say plants, that grow uncontrollably when given large amounts of food and water?
[1] There is also a framing issue in the question being asked – they were “primed” to respond to certain food types; which foods actually gave them problems are unknown.
“This survey asks about your eating habits in the past year. People sometimes have difficulty controlling how much they eat of certain foods such as:
- Sweets like ice cream, chocolate, doughnuts, cookies, cake, candy
- Starches like white bread, rolls, pasta, and rice
- Salty snacks like chips, pretzels, and crackers
- Fatty foods like steak, bacon, hamburgers, cheeseburgers, pizza, and French fries
- Sugary drinks like soda pop, lemonade, sports drinks, and energy drinks
When the following questions ask about “CERTAIN FOODS” please think of ANY foods or beverages similar to those listed in the food or beverage groups above or ANY OTHER foods you have had difficulty within the past year.”
[2] This paper was authored by now disgraced Brian Wansink of Cornell; I could find no evidence that this paper, unlike others he has written, has been retracted.
[3] The phenotype is “marked by diminished control over consumption, strong cravings, overconsumption despite negative consequences, and repeated failed attempts to control intake.” It reflects the DSM-V description of addictive behavior and is measured to some degree by the Yale Food Addiction Scale.
Sources: Addiction to Highly Processed Food Among Older Adults University of Michigan Institute for Healthcare Policy and Innovation
The concept of “food addiction” helps inform the understanding of overeating and obesity: Debate Consensus The American Journal of Clinical Nutrition, DOI: 10.1093/ajcn/nqaa345




