The study looked at the immunological, not necessarily clinical, response in three settings:
- Individuals recovering from COVID without vaccination. (Vaccine-naïve)
- Individuals recovering from COVID with vaccination. (Hybrid)
- Individuals vaccinated without experiencing COVID. (COVID-naïve)
All of these individuals, additionally stratified as having mild or severe COVID, were from the “first wave” of the pandemic for viral type, and because this was a retrospective study, the three groups were not matched. As we might expect, individuals with severe COVID had more co-morbidities and were more likely male (60%) and older (median age 67). Blood samples were taken six months following immunization, except for those with severe COVID, where blood was sampled at nine months. There was no immunologic evidence of reinfection/infection during those intervals.
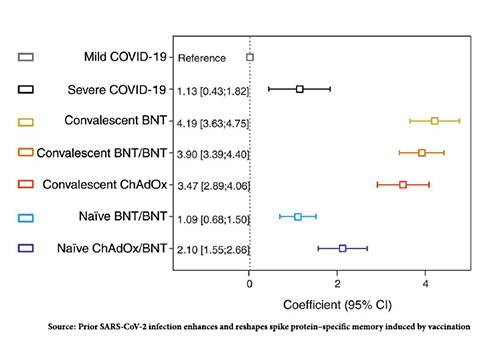 Levels of antibodies directed at the spike protein were highest in those patients with hybrid immunity and lowest among the unvaccinated [1], with the COVID-naïve having intermediary levels.
Levels of antibodies directed at the spike protein were highest in those patients with hybrid immunity and lowest among the unvaccinated [1], with the COVID-naïve having intermediary levels.
As measured by in vitro plaque reduction, the antibodies were more effective in the Delta variant and less so in the Omicron variant. But in both instances, hybrid immunity was stronger than the COVID-naïve response.
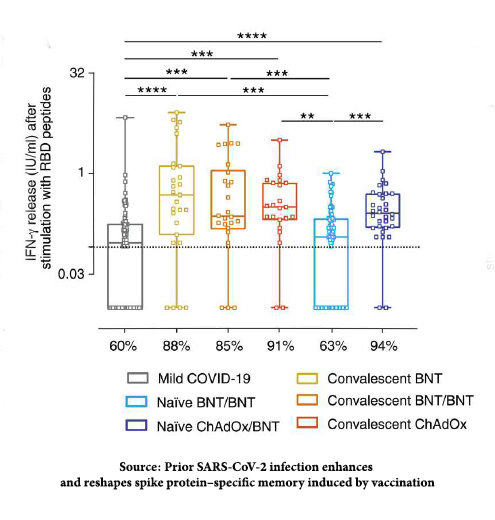 A greater T-cell response results in less severe COVID (inverse proportionality). As for antibodies, hybrid immunity elicited the most robust T-cell response. The researchers also noted that for the COVID naïve, immunization with a mixture of Pfizer and Moderna elicited a T-cell response comparable to hybrid immunity.
A greater T-cell response results in less severe COVID (inverse proportionality). As for antibodies, hybrid immunity elicited the most robust T-cell response. The researchers also noted that for the COVID naïve, immunization with a mixture of Pfizer and Moderna elicited a T-cell response comparable to hybrid immunity.
Finally, the researchers demonstrated that the components of the B cell memory of the spike protein, what they termed the mBC, was altered not only in terms of quantity but in their larger “landscape” or target areas. A heat map demonstrates the differences that the researchers identified.
The heat map shows the various memory cells using location and color to indicate their levels or amounts. In simpler terms, COVID infection combined with vaccination boosts and diversifies our immune response – just as clinical studies have suggested.
“…our data establish that SARS-CoV-2 infection followed by vaccination more efficiently primes the immune system than vaccination alone and builds superior serological and mBC responses….”
For us, the take-home message is having had a COVID infection is not as protective against reinfection as having subsequently been vaccinated. Whether a booster is necessary, especially as we will approach the fall and winter, is unclear. For those at increased risk who have been infected but not vaccinated, this study suggests that thoughtful consideration of getting an mRNA vaccine is worthwhile.
And for those of you searching for a bit more on what our COVID future looks like, at least immunologically, here is an update from Wired Magazine.
[1] more so for those with mild cases than severe ones.
Source: Prior SARS-CoV-2 infection enhances and reshapes spike protein–specific memory induced by vaccination Science Translational Medicine DOI: 10.1126/scitranslmed.ade0550