Cancer cells are smart. Very smart. They can evade the immune system using several different methods that shield them from detection. Thanks to the brilliance of scientists such as Jeff Bluestone, Jim Allison and Carl June, the rapidly flourishing field of cancer immunotherapy is providing an avenue for the immune system to overcome cancer's subversion. Revising features of immune cells enables the immune system to recognize cancer cells for what they are – and destroy them.
Carl H. June, MD, is a professor of immunology at the University of Pennsylvania Perelman School of Medicine. He developed what is known as Chimeric Antigen Receptor T-cell therapy (CAR-T) which is an engineered version of a patient's T-cells to recognize and kill cancer. In a recent interview with the Wall Street Journal, Dr. June describes how his research focused on infectious diseases early in his career – specifically the Human Immunodeficiency Virus (HIV) - which ultimately inspired CAR-T therapy some 15 years ago.
HIV is a type of retrovirus, which means that it replicates in a specific manner and it targets human T lymphocytes, also known as T-helper cells (aka CD-4 cells) – a component of our acquired immunity. If you think of infection as a battle, then consider T-cells as the sword and B-cells as the shield, in the war against bacteria and viruses. When HIV infects CD-4 cells, it replicates by integrating its DNA into the DNA of host cells utilizing its own cut-and-paste tools to do so – modifying its host genome. Gene editing techniques employ the same principle wherein scientists use viruses, like retroviruses, as vectors to introduce, edit, and delete genes within cellular genomes. (To learn more about gene editing click here)
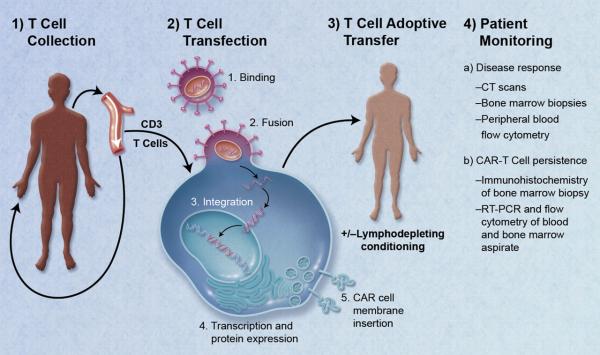
Dr. June's research focused on bullet-proofing the DNA of T-cells so that HIV would be prevented from replicating. In the same fashion, CAR-T cells are created by using viruses to combine the sword and shield function of immune cells as one feature on T-cells – a chimera. Once these chimeric T-cells recognize and destroy cancer cells, they then proliferate and become part of the immune system's long-term memory – acting as a surveillance system.
Just last month, the Food and Drug Administration (FDA) unanimously recommended approval of CAR-T therapy for the treatment of pediatric and young adult B-cell acute lymphoblastic leukemias. Many studies show impressive results with complete or near-complete remission. Advances in cancer immunotherapy have generated unprecedented levels of excitement from both the scientific and the tech sector. Scientists, like Jim Allison, an immunologist from the University of Texas M.D. Anderson Cancer Center in Houston, has earned himself legendary titles such as "rock star" and "warrior." Speakers in the field are presenting their findings to a sold-out house.
At its core, the "mirepoix" of cancer treatment is comprised of – chemotherapy, radiation, and surgery. Immunotherapy is the fourth pillar of what is no longer the "holy trinity" of cancer treatment. The novelty of this therapy, unlike the rest, is its precision and efficiency. Traditional treatments are non-discriminant. My go-to analogy is utilizing snipers in a tactical mission instead of dropping a bomb and annihilating an entire population and chalking it up to collateral damage. A bit violent but that's why it's called a "war on cancer." CAR-T therapy is not without serious side-effects in some, but overall, it inspires real hope that we are getting closer to a cure.