Here's the study, as always, in these types of data-dredging operations, observational. The question at hand was the concern that COVID-19 might be transmitted from one person to another through their eyes, not an unreasonable concern for physicians caring for eye disease, especially in a country, China, where 80% of the population has myopia (near-sightedness).
Over the period from late January to the end of March (which coincides with our concern about COVID-19 on surfaces and the "need" to disinfect packages, etc.), 276 COVID-19 positive patients [1] being hospitalized were recruited and their need and use of eyeglasses quantified.
The median age was 51, slightly more male than female, most "moderately" ill (cough, fever, fatigue), a third had co-morbidities, and 10.9% or 30 patients wore eyeglasses. [2] Disease severity was no different between those wearing eyeglasses and those not. Previous research had suggested that roughly 31.5% of this age group would have myopia, compared to the 5.8% who presented to the hospital with COVID-19. Is this the smoking gun?
"We hypothesized that eyeglasses prevent or discourage wearers from touching their eyes, thus avoiding transferring the virus from the hands to the eyes."
Is that the only reasonable conclusion? Indeed, from an ophthalmologist's perspective, it is all about the eyes, and eyeglasses are an excellent marker of eye disease. But it is also may be the marker for other fellow travelers. Myopia, the predominant global cause of visual disturbances, appears to be partly genetic and environmental (so what else is new?). No significant studies break down myopia by profession; here are the results from a small study, listed by decreasing frequency.
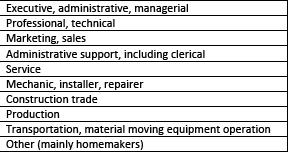 As you can see, individuals with myopia tend to work in situations that are not public-facing, meaning that they interact with a smaller, more consistent group. And as other studies have suggested, myopics tend to be more educated and found in higher-paying occupations. So eyeglasses are a good marker for higher education, higher income, both of which translate to lower exposure to COVID-19 in those early days last winter.
As you can see, individuals with myopia tend to work in situations that are not public-facing, meaning that they interact with a smaller, more consistent group. And as other studies have suggested, myopics tend to be more educated and found in higher-paying occupations. So eyeglasses are a good marker for higher education, higher income, both of which translate to lower exposure to COVID-19 in those early days last winter.
The accompanying editorial states:
"…the data suggest that the observed difference in wearing eyeglasses between the group of patients with COVID-19 vs. the general population is unlikely to have occurred by chance alone, but it does not indicate a causal relationship between wearing eyeglasses and preventing the disease."
Eyeglasses are a classic example of a confounding variable. Without any information on exposure, eyeglasses' use as a defining variable is too heterogenous – a marker of many things, the choice of which remains in the eye of the beholder (pun intended).
[1] The diagnosis was made using a throat swab with PCR testing. In the US, swabs are primarily nasal, as this yields higher identification of the virus's presence.
[2] Those patients who were nearsighted, about half wore their glasses more than 8 hours a day, those that were farsighted did not.
Source: Association of Daily Wear of Eyeglasses With Susceptibility to Coronavirus Disease 2019 Infection JAMA Ophthalmology DOI: 10.1001/jamaophthalmol.2020.3906