“Adults can do what they want, even though there’s simply no evidence that vapes help them to quit smoking. But our kids are not for sale. Their lives deserve our protection.” So wrote US. Rep. Raja Krishnamoorthi, D-Illinois, the author of legislation that would drastically increase the taxes consumers pay for purchasing e-cigarettes and related vaping products. Krishnamoorthi penned that sentence in response to Reason Magazine senior editor Jacob Sullum, who argued in a recent Chicago Sun-Times piece that “Bureaucrats and politicians seem determined to cripple a lifesaving alternative to smoking.”
In a subsequent story, Sullum added that vaping, though relatively unpopular among teenagers, has nonetheless helped drive down teenage smoking rates. Moreover, he explained, a growing body of evidence shows that e-cigarettes help adult smokers abandon combustible tobacco, which is undeniably far more harmful than vaping. I made many of the same points in this recent story: Farewell E-Cigarettes? FDA Effectively Bans Millions Of Vaping Products:
...[T]he evidence is clear that most junior-high and high-school students have no interest in vaping; those who do are already smokers trying to quit. Studies going back to at least 2016 back up this conclusion, and the evidence continues to accumulate … When we factor in the evidence that vaping helps adult smokers give up cigarettes in significant numbers, we have a sound scientific case that the smoking alternative meets the FDA's standard for protecting public health.
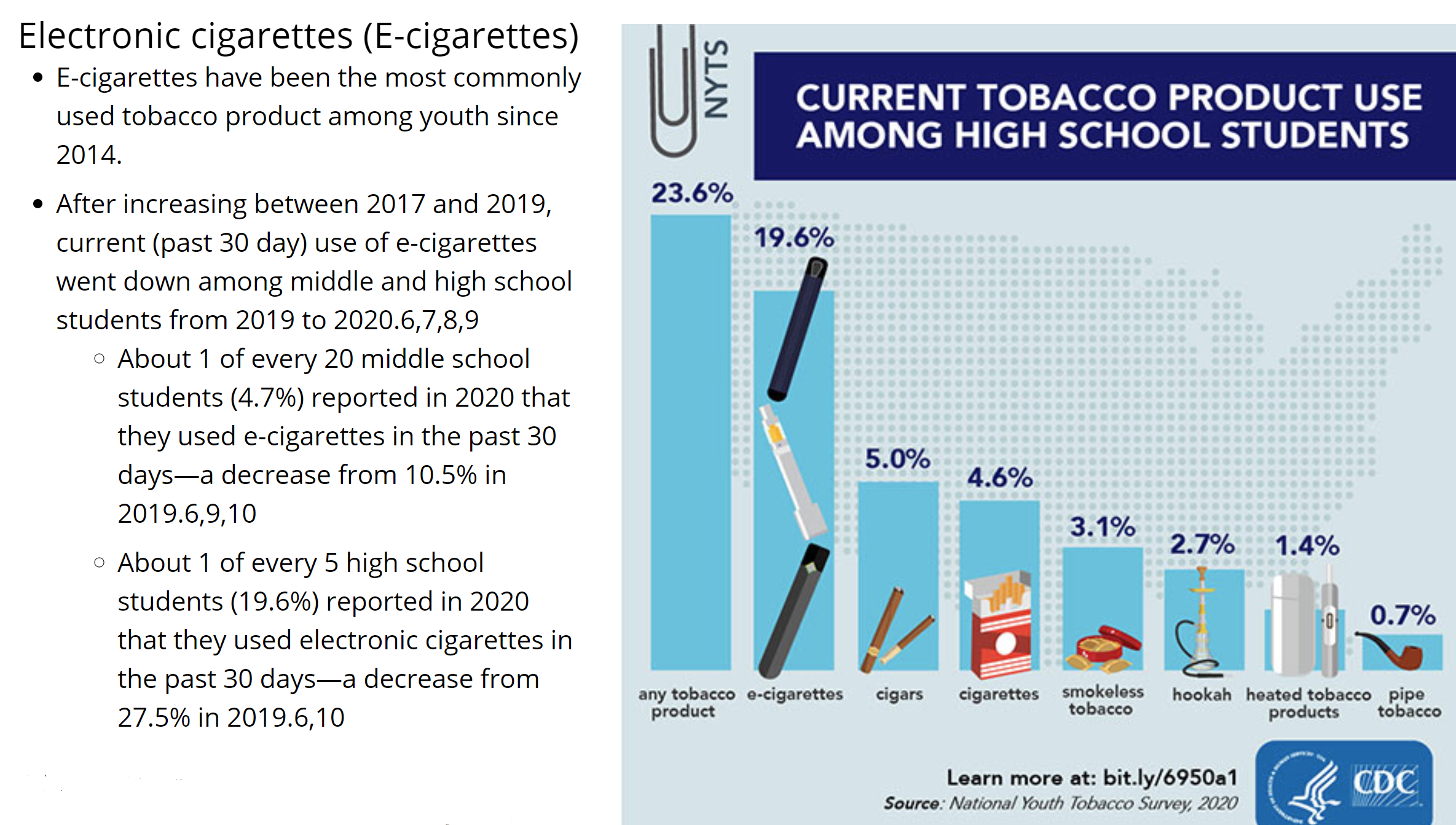
Credit: CDC
There's nothing else to say about the science; Krishnamoorthi just got the facts wrong in his letter to the editor. However, what deserves a little more scrutiny is the assumption that protecting children from nicotine necessitates limiting adult access to vaping products. We should be skeptical of this prohibition-inspired approach to tobacco control because it unnecessarily puts the lives of millions of smokers at risk.
Let's prevent teen vaping and promote smoking cessation
First things first. Everybody agrees that children shouldn't be using nicotine-containing products. Federal law rightly prohibits tobacco sales to anyone under 18, as well as marketing aimed at children. Companies that violate these regulations can be (and have been) severely penalized. The fact that teenage smoking and vaping are declining suggests that these regulations are working.
With those restrictions in place and the data on declining teen nicotine use in mind, it's reasonable to say that anti-vaping campaigns focused exclusively on children distract us from a serious and unresolved public health threat: adult tobacco use—which causes one out of every five deaths in the US annually, more than 480,000 every year. Writing in Nicotine and Tobacco Research in January, Rutgers University ethicist Monica Magalhaes outlined the severe costs that come with our misplaced emphasis on teen vaping:
The bulk of the disease burden caused by smoking happens later in life, not at the young ages when nicotine users become dependent: smokers die earlier (according to the CDC, smokers’ life expectancy is at least 10 years shorter than that of nonsmokers), and most diseases strongly linked to smoking, such as cardiovascular diseases, COPD, and several types of cancer, tend to not affect smokers in their youth.
COVID vaccine roll out as a model
I stress again that we need to do everything we can to prevent nicotine dependence in teenagers, but it's possible to do that while simultaneously protecting adult smokers, the group most vulnerable to tobacco-related morbidity and mortality. This isn't a novel approach either; we followed the same principle as we rolled out the COVID-19 vaccines last year.
On December 1, 2020, the CDC recommended: “that healthcare personnel and long-term care facility residents be offered COVID-19 vaccination first.” The next phase included “people aged 75 years and older and non–healthcare frontline essential workers,” followed by “people aged 65–74 years, people aged 16–64 years with high-risk medical conditions, and essential workers not included” in the preceding phase.
Public health officials didn't implement this plan because they were uninterested in protecting children from infection. Instead, they correctly recognized “that severe illness due to COVID-19 is uncommon among children,” as the American Academy of Pediatrics put it. From a public health perspective, it made sense to prioritize those most vulnerable to severe disease and death for vaccination—to follow a harm reduction approach to infection control. The same principle should guide our efforts to promote smoking cessation and prevent teen vaping.




