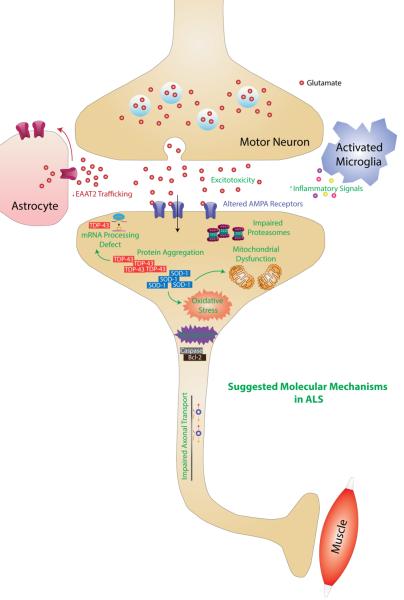
First, a very few words about ALS, Lou Gehrig’s Disease, amyotrophic lateral sclerosis. ALS is thankfully rare, primarily a gradual but inevitable deterioration of the motor nerves controlling voluntary function – walking, talking, and eating. Over a short time, 3 to 5 years, your body betrays your mind; first, by responding to your commands with less strength until you are confined to your house, to your room, to your wheelchair. Then it stops obeying completely. For a few, roughly 10%, your one-sided battle with ALS may last ten years or more.
What ALS doesn’t steal is your thought processes – Dr. Steven Hawkins is the exemplar. But that is a two-edged sword, an active mind locked within an increasingly unwilling body; a mind witnessing its inevitable day-to-day loss and, consequently, becoming anxious and depressed. ALS, for patients and their families, is not for the faint of heart. I think there has to be faith.
There is no curative treatment for ALS; the best 24/7/365 care will reduce complications and make life a bit easier, providing an unmeasured extension of a patient’s quality of life. Until last week, all our “medical science” had to offer were two drugs, one oral and one intravenous, that “slowed the decline” in an ALS patient's day-to-day life.
Enter Amylyx
For some time, the FDA has loosened the threshold for consideration of desperately needed drugs. The poster boy here is Biogen’s Aduhelm, which may or may not slow the progression of dementia but show efficacy in reducing a worrisome, yet not necessarily causal biomarker, amyloid deposits. [1]
In March, the FDA’s external advisory board considered the application of Amylyx Pharmaceuticals for its “experimental ALS drug,” which, like the other two approved drugs, slow the progression of ALS. At that time, the data from a single Phase II, a small study in humans of whether the drug provides a beneficial effect and raises any safety concerns. A version of those Phase II results has been published in the New England Journal of Medicine. Briefly,
- One hundred thirty-seven patients, 89 in the treatment group, 48 receiving placebo.
- 69% of the treatment group completed the trial, and 77% of the placebo group completed the trial.
- There were differences between the groups in their prior use of the two available ALS drugs and in the portions of their motor nerves primarily impacted.
- The rate of decline was less in the treatment group than in the placebo group as measured by a rating scale measuring the impact of ALS on “four subdomains of bodily function (bulbar, fine motor, gross motor, and breathing).”
- The rate of survival, the need for permanent or surgically managed breathing, and hospitalization, “although mostly in the same direction as the primary outcome, did not differ significantly between the two groups.”
Choose your goalpost. We have data suggesting improved function but no data showing improved survival [2]. There are other diseases where we improve the quality of life but make little difference in the long-term survival. The use of angioplasty and stents in patients with coronary artery disease presenting as angina reduces the episodes of chest pain but barely alters survival. On the other hand, the same procedures for a patient with a myocardial infarction can extend their lives. This is not a treatment dilemma solely for ALS.
What Changed?
Several factors may have played into the advisory committee’s change of mind.
- First, a reanalysis of the completed Phase II study demonstrated a possible survival benefit of 18 months – a long period in a world where the time from diagnosis to death is usually 36 to 60 months. The initial analysis put the survival benefit at 4.8 months greater than the placebo.
- Second, the drug was approved by Health Canada (their FDA) based on the same data and the requirement that the Phase III, much larger clinical trial results, would be submitted in 2024. This raised the genuine concern that “medical migrants” would find a way to obtain the drug through Canadian sources.
- Third, among the new data submitted was a study of the drug in Alzheimer’s patients. In an echo of Aduhelm, the new Amylyx drug “improved biomarkers associated with neurodegeneration.”
- Fourth, “The case for AMX0035 was supported by testimony from two well-known ALS researchers who spoke on behalf of Amylyx Pharmaceuticals, … as well as nearly two dozen other doctors, advocates, and patients who testified at the meeting’s open public hearing.”
“To deprive ALS patients of a drug that might work—it’s not something that I’ll feel terribly comfortable with. In the previous meeting it wasn’t that clear.”
- Liana Apostolova, MD, Indiana University School of Medicine, voting for the drug.
“That’s a huge deal because it’s a quarter to a half of an average patient’s lifespan” after diagnosis. “That’s something we’ve never had before.”
- Brian Wallach, an ALS patient and co-founder of patient advocacy group I AM ALS, through an interpreter.
As was the case for Aduhelm, I think there is more at play than simply making a choice when the data is uncertain. FDA leadership speaks of “regulatory flexibility,” but that belies what a clinician might say. Amylyx’s new drug is a possible incremental improvement in a disease with no good treatment options. It is something we can offer now. It is what a clinician would provide to those patients with faith; they would offer hope. And that is really what underlies the turnabout by the FDA advisory committee; the solace of hope gently shifts the balance of uncertainty.
“We are highly sensitive to the urgent need for the development of new treatments for ALS.” - Billy Dunn, director of the FDA’s Office of Neuroscience.
Writer’s Note: The ACSH recently lost a friend and donor in her struggle with ALS, and we have been casting about to find some way to honor her memory. The FDA’s external advisory committee chose to give hope where the patient’s best treatment lies in faith. May this article and our overall work be a bit of hope in the faith that our friend showed in us.
[1] Fierce Biotech reports that Biogen’s CEO and most of their Aduhelm team have been “side-lined,” a new term for let go, as the company saw no financially viable way forward with the drug after Medicare’s approved its use only in clinical trials, not for the entire population at risk.
[2] The Phase II study was not designed to demonstrate a statistical significance to survival, requiring far more patients and a longer study period.
Sources: Amylyx's neuron-protecting drug slows ALS decline in late-phase study Fierce Biotech
Amylyx's ALS drug faces tough FDA scrutiny ahead of 2nd advisory panel meeting Fierce Biotech
Trial of Sodium Phenylbutyrate–Taurursodiol for Amyotrophic Lateral Sclerosis NEJM DOI: 10.1056/NEJMoa1916945
ALS Drug Study Signals Progress Toward Treatment for Deadly Disease Wall Street Journal
Experimental ALS Drug Submitted to FDA for Approval Wall Street Journal
FDA advisers back Amylyx ALS drug, reversing earlier position BioPharmaDive