These authors, from the University of Michigan, concluded that their study provided:
“further evidence supporting PM2.5 reduction as a population-based approach to promote healthy cognitive aging.”
Such air pollution studies of cohorts and populations have piqued the public interest for 50 years, but this one is different and better than most:
- It is based on a defined cohort of about 28,000 individuals rather than entire populations.
- It differentiates PM2.5 from various sources, roughly accounting for differing PM chemistry.
- It includes estimates for other pollutants (PM10, NO2, ozone).
- Exposures are based on 10-y averages at individual residences.
- It compares results for different regression models of increasing complexity.
- It provides incident dementia estimates for a host of demographic and potentially confounding variables.
Here are some unadjusted risk ratios based on the presence of dementia, “yes,” or its absence, “no,” without accounting for interrelationships.
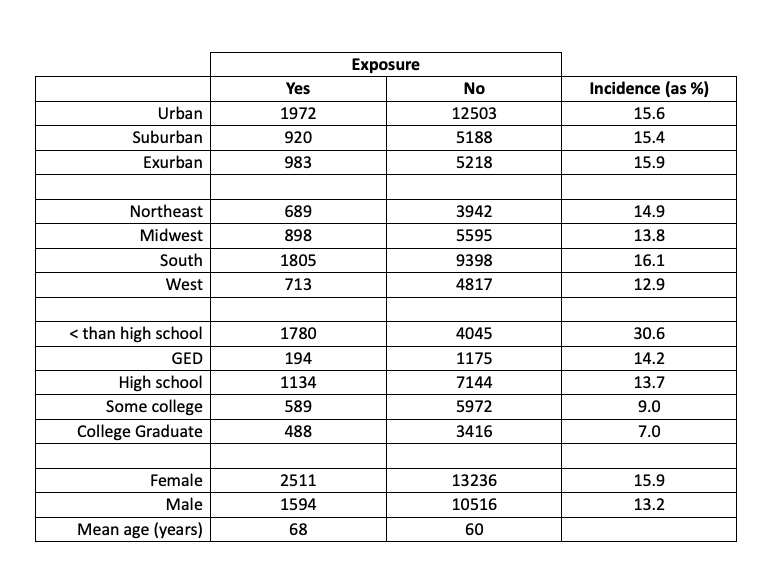 The stark differences are by education level, in that a high-school dropout has about four times the dementia risk as a college graduate. The overall risk of incident dementia over 20-y was about 17% (0.8%/y), similar to reports for the general public.
The stark differences are by education level, in that a high-school dropout has about four times the dementia risk as a college graduate. The overall risk of incident dementia over 20-y was about 17% (0.8%/y), similar to reports for the general public.
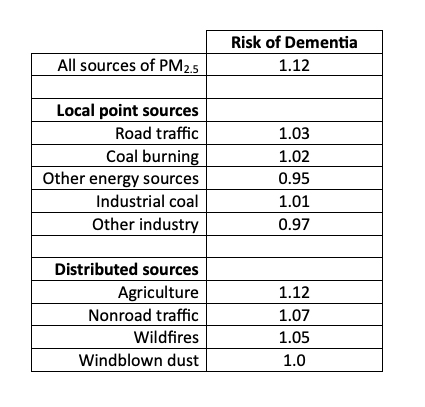 This new study presented risks of incident dementia for ten PM2.5 exposure categories and three statistical models. Estimates from the most complete model are shown in the table; risks associated with traditional point sources are much lower than those from distributed PM2.5 sources and essentially nil. Does this imply that the smartest live near power plants? The NO2 risk ratio was 1.15 and significant, but the ozone effect was negative (beneficial) but not significant.
This new study presented risks of incident dementia for ten PM2.5 exposure categories and three statistical models. Estimates from the most complete model are shown in the table; risks associated with traditional point sources are much lower than those from distributed PM2.5 sources and essentially nil. Does this imply that the smartest live near power plants? The NO2 risk ratio was 1.15 and significant, but the ozone effect was negative (beneficial) but not significant.
So, what’s wrong with this picture? A lot!
- Important individual risk factors were not mentioned: smoking, alcohol, exercise, body mass index, and income.
- Indoor air pollution was not considered.
- Temporal factors were not considered; wildfire exposure is sporadic and rare in much of the US.
Most importantly, differences in the physical properties of particles from various sources were neglected. Many PM studies suffered from this defect. Only nano-sized particles can enter the bloodstream and penetrate the blood-brain barrier, and such small particles comprise only a minuscule fraction of PM2.5 mass. Agricultural and other dust particles have zero chance of entering the brain. Nanoparticles are found in vehicle exhaust, but this study reported nil effects from “road traffic” PM, notwithstanding the significant effects of NO2.
Finally, the authors talk about “reducing” PM to improve brain health, but their analysis is based solely on spatial distributions averaged over ten years, with no analysis of benefits from reduced emissions. Temporal exposure changes were not considered, nor were latency or exposures before the study period.
The one conclusion with which I can agree is the ubiquitous “more research is needed.” I would add that better peer review is needed as well.
Source: Comparison of Particulate Air Pollution From Different Emission Sources and Incident Dementia in the US JAMA Internal Medicine DOI: 10.1001/jamainternmed.2023.3300



