Consider this a sort of Public Service Announcement about the nuances of prenatal testing (and, in an odd way, about the selection of individual pronouns).
mutation
Pre-exposure prophylaxis (PrEP) is one of several historic breakthroughs in the four-decade battle against HIV/AIDS.
As if the Delta variant hasn't been a big enough pain in the a##, pretty much the last thing we need is an "improved" version.
Two years ago, many of you probably had never even heard of many of these terms. Now they're flying around left, right, and center, as are misstatements, misunderstandings, and misdeeds.
It's a bit of an oversimplification, but not by much. One molecule of "vinegar" is responsible for a whole lot of disease and deaths all over the world.
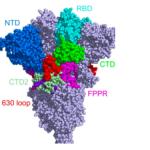
Everything mutates. Random changes to the DNA (or, in the case of some viruses like coronavirus, the RNA) occur, and this can create new traits. Some of these traits are advantageous, and natural selection favors them. This is called evolution.
While Americans were (sort of) celebrating the Fourth of July, the coronavirus kept raging on. Some relevant developments and analysis have occurred in the past few days that might shed a little more light on how the pandemic will unfold.
Mutants are everywhere. And no, I’m not talking about the creatures you find in video games, comic books, or Saturday morning cartoons. We’re the real mutants—you, me, and everyone you know. It’s a fundamental part of being alive.
Many of us are aware of the mutation of the BRCA gene which