The baseline cohort consisted of 10,552 individuals, 55% women. The overall incidence for hip fractures was 789/100,000 in women, 240/100,000 in men – somewhat less than the nationally reported figures.
Results
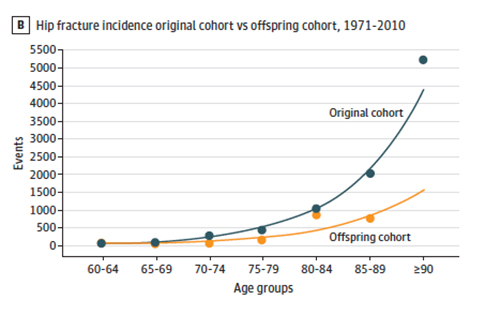
Good news to report! Overall, there was a decrease in hip fractures by 4.4% annually over 40 years, slightly greater for men than women. Age of onset of hip fractures also declined, as you can see in the graph. (Eighty-five seems to be the new seventy-five, at least for hip fractures)
 Most risk factors demonstrated little change over the 40 years with two exceptions, tobacco and heavy alcohol use. Tobacco declined from 38% to 15%, a 60% reduction; alcohol consumption from 7% to 4.5%, a 36% reduction. Of course, smoking and drinking often go together. When the risks were considered separately, smokers did not experience a beneficial decrease in hip fractures. How heavy drinkers fared is a bit more confusing, the researchers reported only the hip fractures in “individuals who were never heavy drinkers.” Not reporting the rate of hip fractures in heavy drinkers is a significant omission when your abstract recommends “continuing to encourage public health interventions for smoking cessation and heavy drinking.” [Emphasis added]
Most risk factors demonstrated little change over the 40 years with two exceptions, tobacco and heavy alcohol use. Tobacco declined from 38% to 15%, a 60% reduction; alcohol consumption from 7% to 4.5%, a 36% reduction. Of course, smoking and drinking often go together. When the risks were considered separately, smokers did not experience a beneficial decrease in hip fractures. How heavy drinkers fared is a bit more confusing, the researchers reported only the hip fractures in “individuals who were never heavy drinkers.” Not reporting the rate of hip fractures in heavy drinkers is a significant omission when your abstract recommends “continuing to encourage public health interventions for smoking cessation and heavy drinking.” [Emphasis added]
Among the study’s stated limitations
- all participants were “exclusively White”
- the incidence of obesity and hip fractures overall was lower than the national average
It is not hard as a physician, to recommend smoking and heavy drinking cessation for hip fractures, or general health. But is this paper adding anything new to our knowledge, or is it just more evidence that the advice is good? How do smoking and drinking result in hip fractures – falling down drunk is not the correct answer. What specific mechanisms involving nicotine and alcohol result in hip fractures? It turns out that that osteoporosis, reduced bone mineral density or BMD, is the gateway in many instances to hip fractures. The underlying physiology is complicated – no surprise there. Two review papers from Osteoporosis International shed both light and shade on the underlying mechanisms. [1]
“The pathophysiologic mechanisms underlying osteoporosis in cigarette smokers have not been fully explored.”
Spoiler alert, the same holds for alcohol. Caveat aside, here is what we believe to be the case. The biologic pathways appear quite similar.
Tobacco Use
- Calcium, a necessary mineral in the formation of bone, is influenced by parathyroid hormone (PTH), and Vitamin D. While studies have shown Vitamin D deficiencies in smokers, there is no consistent finding for PTH. They conclude, “smokers have an unhealthier lifestyle such as low calcium/vitamin D intake and lack of exercise that affects calciotropic hormones and overall bone health.”
- Estrogen, available in both women and men, is protective, reducing the resorption of bone. [2] This is why bone loss is more common in post-menopausal women and the elderly in general. Smoking can reduce the effective levels of estrogen. Testosterone also may play a role in bone health, although its impact is not well studied.
- Nicotine may have a direct effect on the cells of bone formation, osteoclasts absorbing bone, and osteoblasts creating bone. But those effects are complex, a code word for unclear.
- They conclude that “Cigarette smoking is associated with lower BMD [bone mineral density] in a dose-related and duration-related fashion. … The deleterious effects of tobacco use on bone health may be reversible. Multiple mechanisms link tobacco use to greater fracture risk, and the understanding of these underlying mechanism(s) require careful clinical and basic investigation …”
Alcohol use
The impact of alcohol on bone mineral density is contradictory, in part, because studies use both self-reports of alcohol consumption as well as different descriptions of what constitutes light, moderate, or heavy drinking.
- The dose-response is not linear as it is with tobacco. “…low alcohol consumption (one glass per day) is generally beneficial to bone tissue; however, when this is increased to two or three glasses per day, the effects can be positive or negative, depending on the sex, age, hormonal status of the patient, and the type of beverage consumed.”
- The deleterious effects of alcohol seem to occur in the early years of life when bone mineral density is increasing. “Almost all epidemiological studies of alcohol use and human bone health indicate that chronic heavy alcohol consumption, particularly during adolescence and young adulthood, can dramatically affect bone health and may increase the risk of developing osteoporosis later. Alcohol slows bone turnover, perhaps through the cells making new bone, the osteoblasts, but “the specific mechanisms by which alcohol affects bone are poorly understood.” [3]
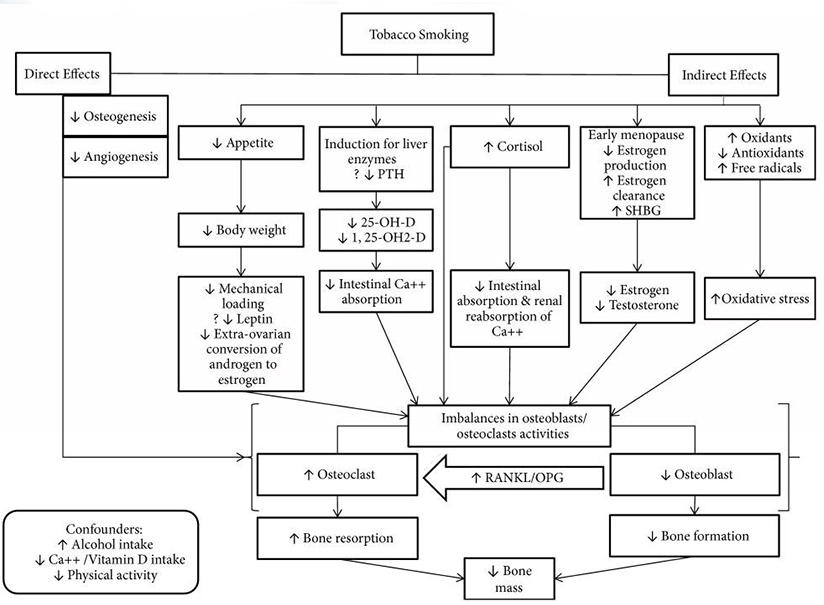
For those who prefer pictures to words, consider these images.
And this
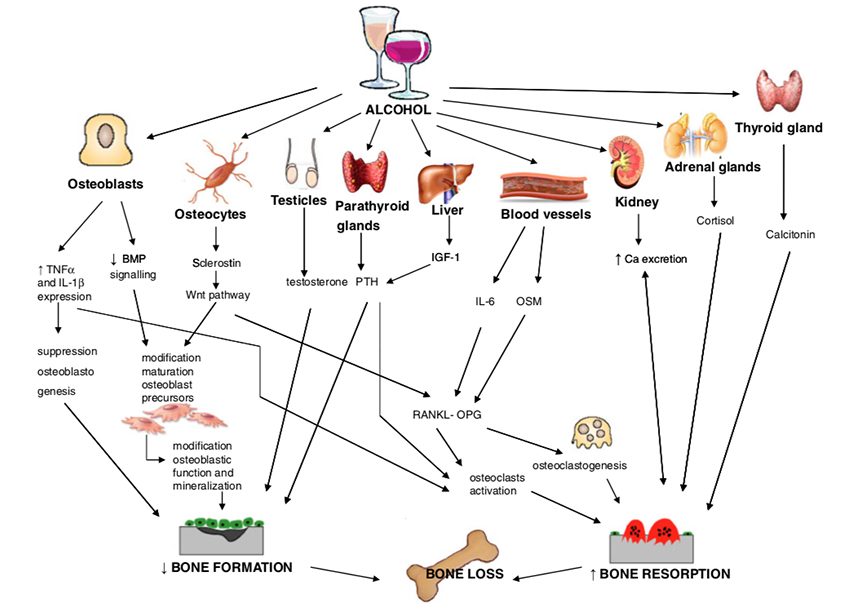
Tobacco and alcohol impact much of our metabolism, in ways we can identify, and others shrouded in a lack of information. Everyone’s metabolism is just a tiny bit different so that observational studies will always be imprecise – that is nature. There are no magic bullets that ameliorate unhealthy behaviors beyond never starting or the ancient dictum, everything in moderation.
[1] The effects of smoking on bone Osteoporosis International DOI:10.1007/s00198-012-1940-y and alcohol and bone: review of dose effects and mechanisms Osteoporosis International DOI: 10.1007/s00198-011-1787-7
[2] bone, despite its seeming constant nature, is like all other tissue, continually undergoing remodeling, with areas being added and subtracted.
[3] Alcohol and Other Factors Affecting Osteoporosis Risk in Women, National Institute of Alcohol Abuse and Alcoholism
Source: Incidence of Hip Fracture Over 4 Decades in the Framingham Heart Study JAMA Internal Medicine DOI:10.1001/jamainternmed.2020.2975




