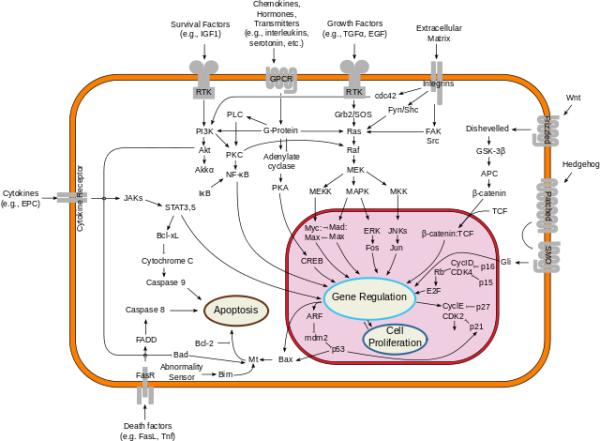
Plasma surrounds the white and red blood cells accounting for slightly more than half of your total blood volume. It is the home of the “secretome,” a host of proteins that serve as inter-cell communicators. These proteins are the foot soldiers in both homeostasis and disease, carrying messages from one area of the body to another. While we have studied these messengers in isolation, we are only beginning to look at them dynamically, how they change over time and their relationship to one another. Looking at the interactions opens up a new world of understanding.
Using about 5,500 plasma sample of Icelanders [1] researchers characterized the plasma proteins based on their physical similarity and the presence with other serum proteins, their "known associates." These protein characterizations formed a network contained 27 different modules, encompassing 85% of the proteins present.
- Modules had distinct, although overlapping, functions.
- Modules reflected protein contributions from a variety of tissues sources; there was no sole contributor.
- Within the module, one protein was identified as the "hub," reflecting “the collective behavior” of the module to a higher degree than others within the grouping.
Using the participants' medical information, the researchers were able to associate the protein modules with diseases, like heart failure and type 2 diabetes. While some modules were not associated with any disease, others were associated with some or all. Then using the participants genomic information (another application of GWAS) they found that specific areas of the genome regulated messenger proteins of the same cluster – raising the possibility that variations in our DNA sequence shape our network, our secrotome.
Conjecture
Let me take these findings and speculate as a clinician, on how this knowledge reflects and alters our understanding of the underlying cause of disease. First, genetics plays a role in the expression of our chemical “sensors and integrators of complex disease.” Second, we can stratify those sensors and integrators into groups with similar functions. Third, the presence or absence of these functional clusters is associated with specific diseases.
Could the genetic variations, and each of us in unique in our secretome profile, be our predisposition to disease? Consider this example. Our arteries are not inert tubes, but are dynamic structures, rebuilding themselves continually. What if there was just a slight change in the chemical signals involved in the rebuilding; and as a result, the rebuilt artery was every so slightly weaker. Now add in another variable, like hypertension where the pressure inside the weakened artery is increased. The combined effect of an ever so subtle genetic variation and high blood pressure would become expressed phenotypically as an aortic aneurysm, a bulging of the artery's weakened wall. Or perhaps it is not high blood pressure, but stress and the release of hormones that cause our blood pressure to be higher. A recognition that a genetic variation results in the predisposition to specific a disease and is not the cause of the disease helps to explain a host of contradictory findings - disease is a result of interactions, and some of the phenotypes we use are too heterogeneous, we continue to compare apples to oranges.
The network uncovered by the researchers reveals different associations and can provide us with biomarkers of disease predisposition. Introducing the relationships of genetics, signals and phenotypic disease brings us deeper into the mystery of how we age.
[1] Part of a prospective study of aging, these participants are “deeply phenotyped and genotyped.”
Source: Co-regulatory networks of human serum proteins link genetics to disease Science DOI: 10.1126/science.aaq1327